Covid-19 vaccines and you: How safe are they?
Sign up now: Get ST's newsletters delivered to your inbox
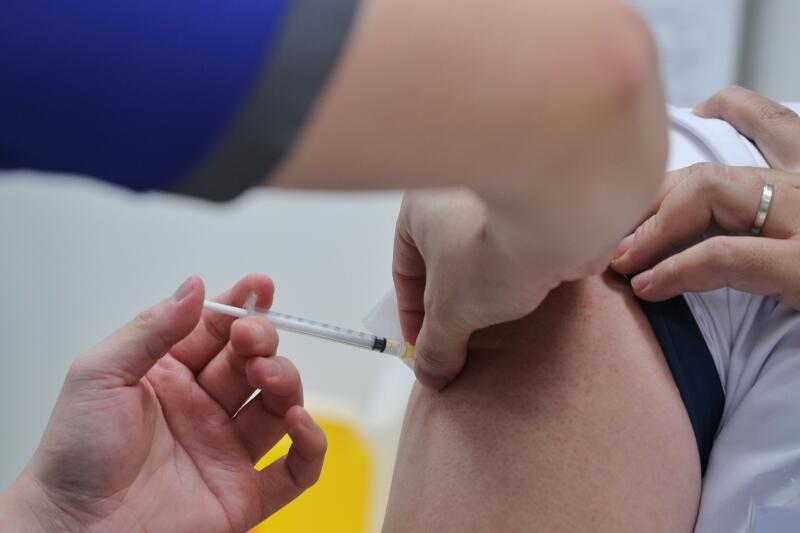
Phase 3 trials are much larger, usually involving thousands to tens of thousands of people.
PHOTO: AFP
SINGAPORE - Covid-19 vaccinations have started in Singapore for healthcare front-liners and will be rolled out to the elderly and the rest of the population progressively. From safety to efficacy and the nation's vaccination strategy, Insight answers all the key questions.
Q: How safe are Covid-19 vaccines?
A: Multiple steps are being taken to ensure any Covid-19 vaccine approved for use in Singapore is safe.
First, the data must point to safety in animal studies before the vaccine is allowed to be tested on humans.
Even when clinical trials begin, there are numerous phases involved.
The first two phases of clinical trials, known as early-phase trials, are carried out mainly among smaller groups of up to hundreds of volunteers to test the safety and efficacy of a vaccine.
In these stages, researchers look out for dangerous side effects and analyse patient samples to see how the human immune system is responding to the vaccine.
Phase 3 trials are much larger, usually involving thousands to tens of thousands of people. These are often held across multiple jurisdictions or countries.
For instance, the Phase 3 trial of the Covid-19 vaccine by Pfizer-BioNTech - the only vaccine approved for use in Singapore - involved more than 43,000 people. Another leading Covid-19 vaccine front runner, developed by Moderna, had a Phase 3 trial involving more than 30,000 people.
Once late-stage clinical trials have concluded, the data will be reviewed again by the Health Sciences Authority (HSA) before a vaccine is approved for use in Singapore.
This means all vaccine candidates undergo a multi-step "screening" process, and must pass safety checks at each stage before proceeding to the next.
Q: But if safety checks are robust, how could a Covid-19 vaccine be developed in such a record time, considering that it usually takes about a decade for a vaccine to be rolled out?
A: There are a number of reasons for the record pace at which Covid-19 vaccines were developed.
One was funding. During the pandemic, more funds were ploughed into vaccine development, accelerating the pace of research.
For instance, Time magazine reported last month that the United States alone put US$12.4 billion (S$16.4 billion) into vaccine development and manufacturing under its Operation Warp Speed programme.
A 2018 paper published in medical journal The Lancet noted that developing a single epidemic infectious disease vaccine from pre-clinical trials to the end of early-phase trials could cost between US$31 million and US$68 million, assuming no risk of failure.
Another reason is that two leading vaccine candidates, by Pfizer-BioNTech and Moderna, use new messenger RNA (mRNA) technology. This involves injecting just snippets of the coronavirus' genetic material - and not the whole virus - into the human body to stimulate an immune response.
Traditional vaccines, on the other hand, use a live or weakened virus injected into the body to teach it to recognise the invader.
Vaccines that use mRNA technology do not require manipulating the actual virus, and are safer and quicker to produce.
As Moderna co-founder Robert Langer, the David H. Koch Institute Professor at the Massachusetts Institute of Technology, said: "With traditional vaccines, you have to do a lot of development. You need a big factory to make the protein, or the virus, and it takes a long time to grow them.
"The beauty of mRNA is that you don't need that. If you inject nanoencapsulated mRNA into a person, it goes into the cells, and then the body is your factory. The body takes care of everything else from there."
Third, regulators like HSA are now also allowing pharmaceutical companies to submit real-time data on a rolling basis, instead of only at the end of each phase of the trial.
Such rolling submissions allow regulators to conduct a simultaneous real-time review of the data available to date, instead of waiting for all the data to be gathered before they review it.
This can halve the time it would normally take to have a new vaccine approved, while ensuring that relevant safeguards are in place.
Q: Should I avoid taking a Covid-19 vaccine if I am afraid of getting severe allergic reactions?
A: As with all established vaccines and medications, there is a small risk of very rare but serious adverse events, including allergic reactions, that may occur post-vaccination.
Those who receive the Covid-19 vaccine will be watched for 30 minutes after the jab so that any severe allergic reactions such as anaphylaxis can be detected and treated promptly.
A new programme will also be introduced to provide support for those who experience serious side effects related to Covid-19 vaccines administered here.
Health Minister Gan Kim Yong told Parliament that this new programme by the Health Ministry will give peace of mind to those receiving the vaccines, although few are expected to need it.
More details on the vaccine injury financial assistance programme will be announced later, he said.
Q: Which groups of people should wait before receiving the Covid-19 vaccine?
A: Those with a history of severe allergic reactions should not take the Covid-19 vaccine yet.
Other groups, such as pregnant women, immunocompromised individuals and those under the age of 16, should also hold off on receiving the shots, as large-scale clinical trials have not involved such volunteers.
This means there is not yet enough data to evaluate the safety of Covid-19 vaccines for these groups of people.
Mr Ryan Richardson, chief strategy officer and managing director at BioNTech, told The Straits Times in an interview this week that studies to determine safety and efficacy in these sub-groups are ongoing.
He said the full data set for the effects of the vaccine on pregnant women is still being collated.
But in terms of age groups and ethnicity, the data collected so far indicates no serious side effects. The company is also closely monitoring the vaccination campaigns being rolled out, he said.
Q: There were reports that people died after taking the Pfizer-BioNTech vaccine. Is it really safe?
A: There were reports that six people died during clinical trials of the Pfizer-BioNTech vaccine.
But Mr Gan said in Parliament that only two of the six individuals were given the vaccine; the other four had the placebo. Investigations revealed no causal relationship between the vaccine and the two individuals' deaths.
Q: Will mRNA vaccines change my DNA?
A: No, they will not. As an article in the scientific journal Nature noted last month: "The RNA does not enter the nucleus where the cell's genome resides, and is degraded by the cell within a day of the injection."
The mRNA vaccines involve injecting snippets of the genetic material of the coronavirus into the human body. After injection, human cells "read" this mRNA sequence to build viral spike proteins - which enable the virus to infect human cells. This trains the body to recognise a key part of the virus - the spike protein - without exposing it to the whole virus.
The body will then begin to manufacture "soldiers" such as antibodies and killer T-cells to get rid of the foreign invader.


