Covid-19 vaccinations in overdrive in Singapore
Singapore aims to vaccinate two-thirds of people here against Covid-19 by National Day, but not everyone wants the shots. Should the vaccination be made mandatory at some point? Insight examines this and other vaccine-related issues that have surfaced.
Sign up now: Get ST's newsletters delivered to your inbox

Observers say vaccination has changed the face of the Covid-19 disease, which is poised to become endemic.
PHOTOS: LIM YAOHUI, ST FILE
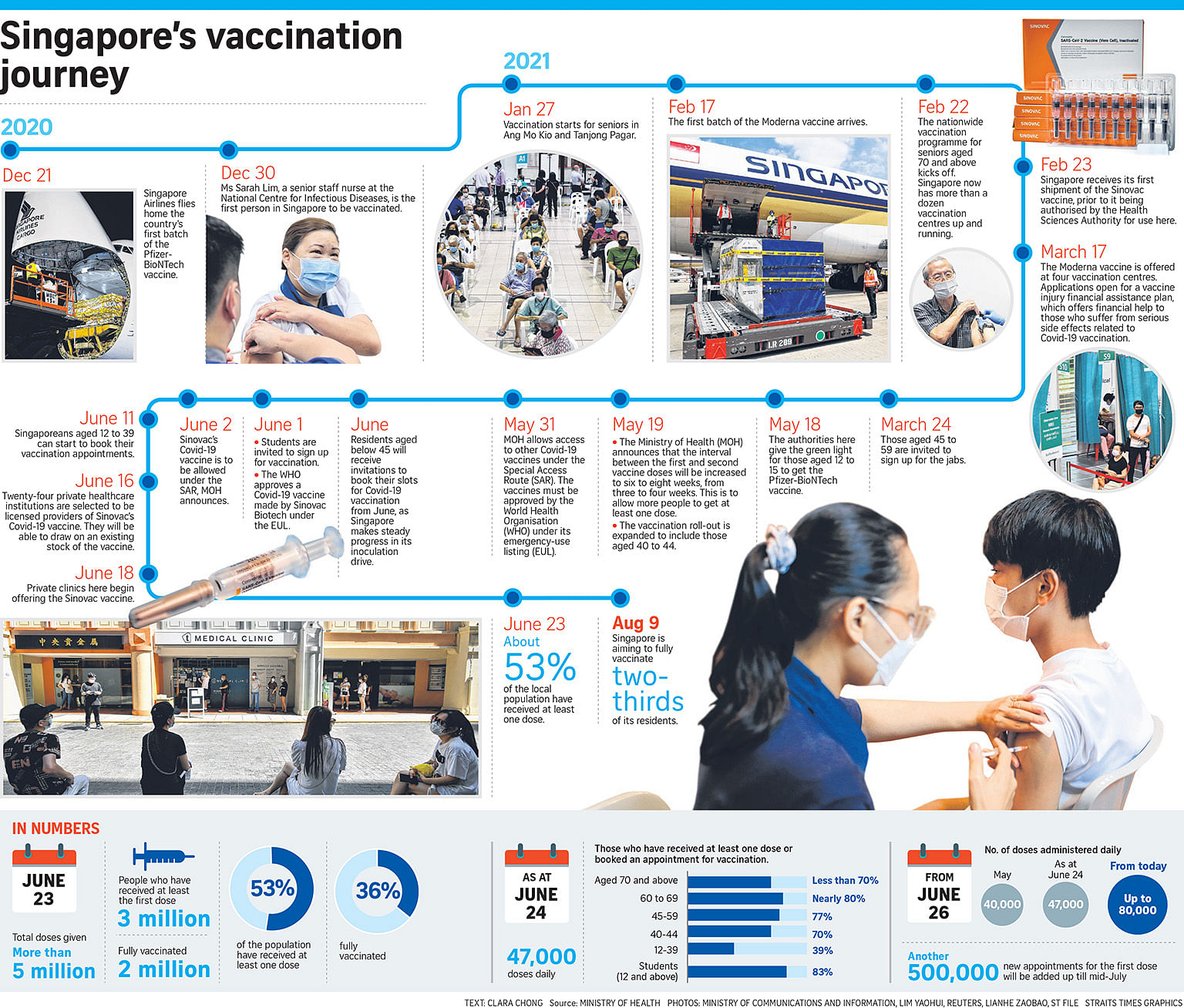
SINGAPORE - Six months, five million doses, and over half the population at least partially vaccinated.
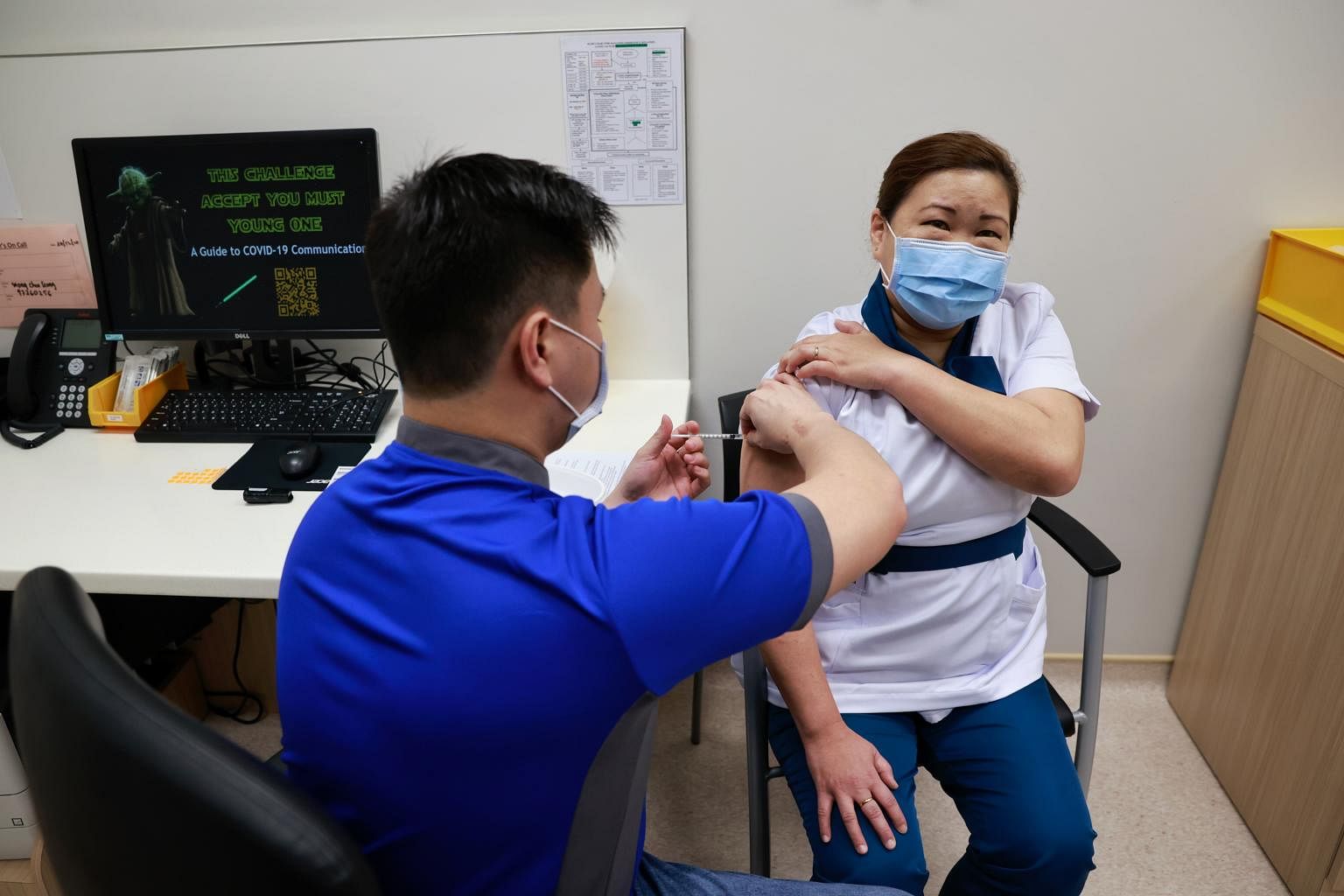
Singapore's quest to protect its people against Covid-19 continues apace since a senior staff nurse - Ms Sarah Lim, 47 - became the first person here to receive the Pfizer-BioNTech vaccine on Dec 30 last year.
She received her second dose on Jan 20 and has been "in good health and am feeling absolutely fine", she said this month.
As the population heads towards herd immunity, observers say vaccination has changed the face of the disease, which is poised to become endemic. Vaccinated individuals can expect to be much less severely ill if they are infected, and are likely to have continued protection if they get regular booster shots.
In the meantime, how many more fence-sitters on the question of vaccination will be converted is still unclear, raising the prospect of vaccine haves and have-nots.
At a press conference on Thursday, the multi-ministry task force tackling Covid-19 gave a preview of this, announcing that larger gatherings as well as testing in lieu of stay-home notice may be allowed for people who are vaccinated.
But experts in infectious diseases, sociology, law and urban planning told The Straits Times that while containment strategies for outbreaks continue to be refined, Singapore's policies regarding vaccinations are not likely to change very much.
People will still have a choice on whether or not to be inoculated, said Professor Ooi Eng Eong, an expert on emerging infectious diseases at Duke-NUS Medical School.
"I do not think mandatory vaccination is necessary for successful disease prevention. We should balance our rights to health and freedom to choose," said Prof Ooi, whose own vaccine, which he co-developed with pharmaceutical company Arcturus Therapeutics, is still under trial.
Both he and Singapore Management University (SMU) law don Eugene Tan said efforts to persuade people of the benefits of vaccination will continue.
Associate Professor Tan noted that as the vaccines have only emergency-use approval, they are unlikely to become mandatory - but "nudges" will keep coming from the Government.
"There will be a concerted effort to encourage and educate people on the benefits of vaccination. To add to the confidence level, the Government will likely maintain the vaccination insurance programme as well," said Prof Tan, referring to the Government's Vaccine Injury Financial Assistance Programme.
The scheme supports people who suffer adverse effects from their Covid-19 jabs.
Currently, only vaccinations against diphtheria and measles are mandated by law in Singapore, noted infectious diseases expert Paul Tambyah, president of the Asia-Pacific Society of Clinical Microbiology and Infection.
Despite this, the acceptance rate of optional vaccines for infants - such as the BCG and hepatitis B vaccines - is close to 100 per cent, said Professor Tambyah, who thinks it is likely to be the same case for coronavirus vaccines as their safety and effectiveness are proven over time.
Singapore was aiming for half of its residents to be fully vaccinated by August, and at least 75 per cent by October. But due to the delivery of vaccines being brought forward, it has set a new target of having two-thirds of the population fully vaccinated by National Day.
Efforts to boost the vaccination rate should factor in why some people are resistant to the idea and allay their fears, said Professor Paulin Straughan, a sociologist at SMU.
Pointing to the long queues that formed at clinics offering the more traditional Sinovac vaccine earlier this month after it was allowed for use here under the Special Access Route framework, she said some people clearly still have doubts about the Pfizer-BioNTech and Moderna mRNA vaccines used in Singapore's national vaccination programme.
"It shows that they had fears which relate to how the vaccines are derived. In short, they are not holding out because of wilfulness, but rather, genuine concerns. So we should try to better understand, and in the long run, take an inclusive stance," she said.
Vaccine discrimination
Some argue that people who remain set against vaccination should not be eligible for subsidised healthcare if they become infected with Covid-19.
Dr Tan Ern Ser, a sociologist at the National University of Singapore (NUS), said: "My personal take is that people should be responsible for the conscious, informed decision they made in regard to vaccination. This principle would also be fair to those who have complied."
But experts agree it is unlikely that people who decline to get vaccinated will be subjected to lower-quality or more expensive healthcare should they be infected with the disease.
They cautioned that treating unvaccinated people differently would be discriminatory.
Dr Woo Jun Jie from NUS' Institute of Policy Studies, who researches urban planning, does not see this happening. "I don't think there will be great disparity between vaccinated and unvaccinated individuals, and certainly it is important to note that there are people who are not able to receive the vaccine for various reasons."
Several experts made comparisons with how healthcare providers do not penalise smokers when they use medical services, even though it is scientifically proven that smoking is the main risk factor for many diseases.
Prof Tan said that as long as the coronavirus remains a significant public health threat, the imperative to ensure that those infected get prompt medical assistance will remain.
Singapore Medical Association president Tan Yia Swam told ST she was confident that doctors and healthcare workers would not shirk their professional responsibilities.
"Regardless of any personal feelings I might have towards anti-vaxxers, my duty to them as a doctor comes first. As a citizen, it might feel unfair - but the unfairness could just as well apply to any other chronic illness where someone does not take personal responsibility for his own health," she said.
"Can I blame a smoker for getting lung cancer? How about non-smokers who get lung cancer? There is no clear cause and effect sometimes."
She added that recommendations will be made about the need for regular booster shots once more data on the long-term effectiveness of the vaccines is available.
Vaccine cost
In Parliament on May 11, Trade and Industry Minister Gan Kim Yong, who co-chairs the multi-ministry task force tackling Covid-19, hinted at how much the vaccination programme has cost when he said the average cost of each vaccine regime is roughly $100.
A significant part of the cost is in the logistics required, such as setting up vaccination centres and mobilising healthcare professionals, he noted.
This would put the price tag for all vaccinations so far at no lower than $250 million.
Prof Ooi said free vaccines and healthcare for coronavirus patients in the longer term could mean that Singaporeans will have to pay higher taxes, given the need to mobilise more public resources.
But he added that should the public be charged for the jabs, some level of subsidy will be needed to ensure that price does not become a deterrent to getting vaccinated.

SMU's Prof Tan pointed out that although the Government will "very likely" continue to commit the necessary resources to ensure people are kept safe from Covid-19 through means such as vaccination, the issue of financial sustainability will become relevant if the pandemic is going to be long-drawn.
Such a situation could arise if more infectious and deadly variants of the virus emerge. Earlier this week, India announced that it had labelled a new mutation of the highly infectious Delta strain of the coronavirus - dubbed Delta Plus - as a variant of concern because of its possible increased transmissibility.
Prof Tan suggested co-payment as one way to manage such costs, or that employers include vaccination in their medical benefits for workers.
Insurance schemes could also include the shots as part of their comprehensive coverage, and financial assistance should be set up for people who cannot afford the shots themselves, he added.
Dr Woo said using public funds for vaccination might not be sustainable if the jabs have to be administered regularly, as some health experts are suggesting. "In the long term, it may no longer be feasible to continue paying for Covid-19 treatments out of public coffers, especially when the vast majority of the population would have been vaccinated," he said.
Some experts, such as NUS' Dr Tan, said that once Covid-19 becomes endemic, treatment and vaccines may be subsidised for some time and that the Government would take a calibrated approach to any change to this.
Any kind of fees the public will have to pay will not happen so soon, they surmised.
Prof Tambyah said that what may occur is that small administrative fees for providers dispensing the vaccines could be passed on to the public, as is done now for the human papillomavirus vaccination for Secondary 1 female students.
"In Singapore, once something is given for free, it is hard to start charging for it," he noted. "The vaccines may remain free, but once the vaccination centres close, the polyclinics and GP clinics which will eventually be administering the vaccines will probably be allowed to charge an administrative fee."


