News analysis
Eligible individuals who refuse Covid-19 vaccine endanger themselves and others
Sign up now: Get ST's newsletters delivered to your inbox

A Covid-19 vaccination drive under way at Senja-Cashew Community Club on Feb 22, 2021. Once the vast majority of the population is protected against Covid-19, Singapore should be able to fully open its borders.
ST PHOTO: GAVIN FOO
SINGAPORE - Singapore has purchased enough vaccines for everyone here so that all who are eligible can get vaccinated.
Once the vast majority of the population is protected against Covid-19, Singapore should be able to fully open its borders, and life can start returning to normal.
But that can happen only if everyone who is eligible gets vaccinated.
The question is: Will all such people be willing to get inoculated?
If significant numbers don't, it can jeopardise the entire programme.
This is because eligible people who do not get vaccinated not only put themselves at risk - which we can argue is their choice - but will also endanger children and those who, for medical reasons, are not suitable for the vaccine.
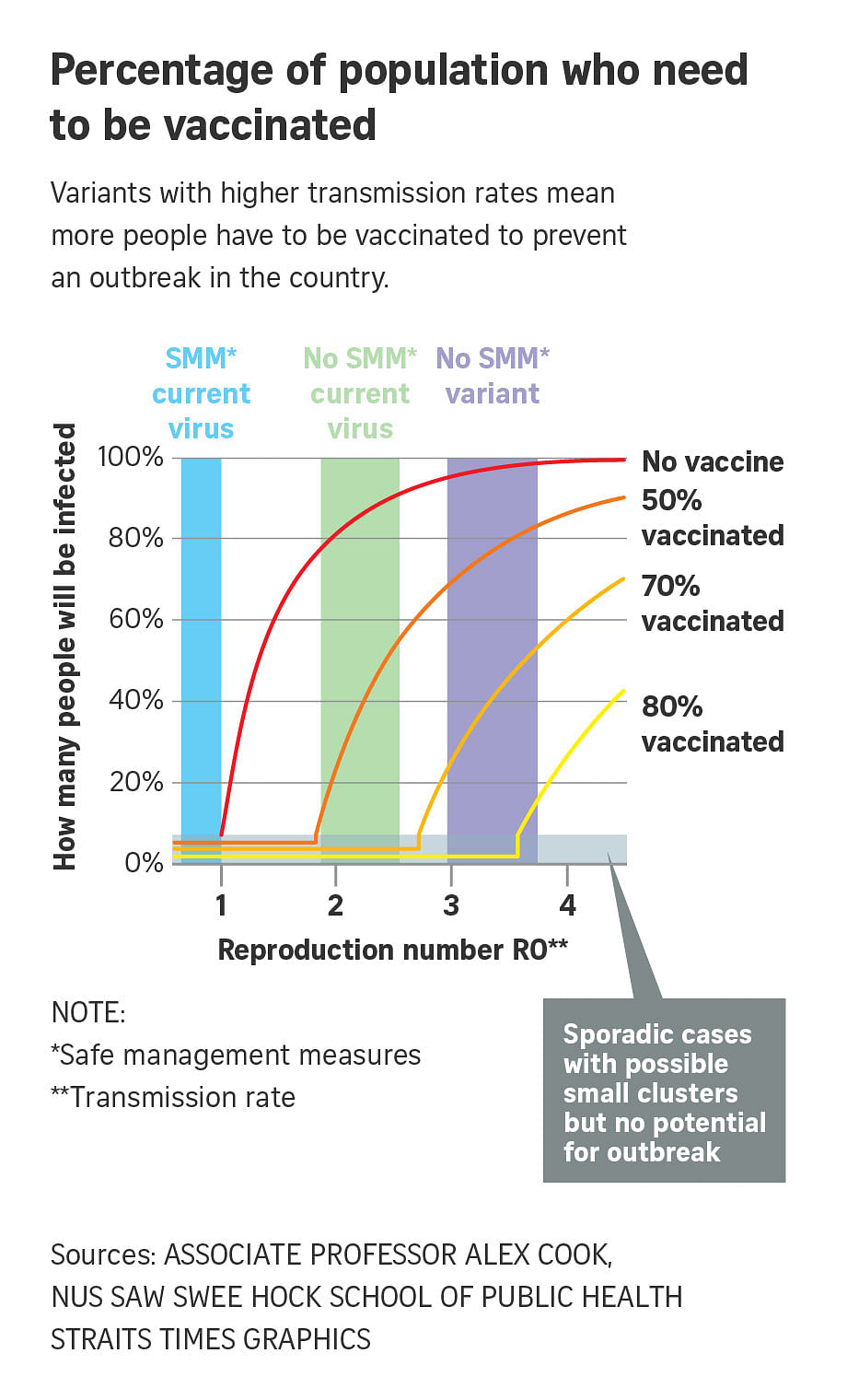
Associate Professor Alex Cook of the National University of Singapore (NUS) Saw Swee Hock School of Public Health said the percentage of people who need to be vaccinated depends on the R0 - the reproduction number - or how transmissible the virus is.
The higher the R0, the larger the number of people who need to be vaccinated to achieve herd immunity in the country.
The various measures countries have put in place to prevent the spread of the virus have made the computation of the R0 difficult.
Experts estimate it to be between two and three, which means one person will likely infect two to three others.
Assuming an R0 of 2.5 and vaccine effectiveness of 90 per cent, Prof Cook said 67 per cent of the population will need to be vaccinated to prevent an epidemic, although small clusters of cases may still occur.
However, some new variants, such as B117 from England, are said to be 50 per cent to 70 per cent more transmissible, which pushes up the R0 to about four.
Any R0 that is above one would result in rising numbers. The higher the number, the faster the spread.
The 1918 flu pandemic that is estimated to have killed 50 million people had an R0 of between 1.4 and 2.8.
Prof Cook said a virus with an R0 of four would mean 85 per cent of the population need to be vaccinated to prevent an outbreak, if no other mitigating measures are in place.
"Then we'd be in trouble and some safe management measures will have to continue," said Prof Cook, as these figures also assume that vaccination prevents transmission - and the jury is still out on that.
All that has been proven is that the vaccines significantly reduce severe illness and deaths.
However, Prof Cook said that realistically, there should be some reduction in transmission from people who have been vaccinated.
Professor Teo Yik Ying, dean of the NUS Saw Swee Hock School of Public Health, pointed out that some vaccines have been found to be less effective against the variants from England and South Africa.
Professor Ooi Eng Eong of Duke-NUS Medical School, who specialises in viral research and immunology, agreed that some variants "could present challenges for the current versions of Covid-19 vaccines".
But he added that this is currently only theoretical, and based on antibodies needed, without looking at the role of T cells.
"Vaccines that generate good T cell responses, in addition to antibodies, would not be significantly impacted by these variants and would remain highly efficacious," he said.
The concern is that not all vaccines do that.
Prof Teo said: "If the effectiveness of vaccines does decrease as a result of these new variants, we will actually need to vaccinate more people to achieve the level necessary for herd immunity."

<p>Hotel staff getting their Covid-19 vaccine shots at a vaccination centre in Raffles City Convention Centre on 28 January 2021.</p>
PHOTO: ST
Those eligible for the vaccine account for roughly 85 per cent of the population, since more than 10 per cent are children aged 15 and younger for whom the vaccine is currently not recommended.
There are also people who, for medical reasons, should not be vaccinated.
To protect these vulnerable people, it would help if everyone else is vaccinated, to cut the spread of the coronavirus in the country.
People who refuse to get vaccinated do so for various reasons, such as fear, misinformation or even complacency, given the low community spread here.
They may also be anti-vaxxers who refuse all vaccines.
The Government has promised that Covid-19 vaccination is voluntary, unlike for diphtheria and measles where immunisation is compulsory by law.
So it is up to people to decide if they want the protection.
But is a decision not to get vaccinated fair to others?
Will their fear, stubbornness or selfishness put those who are unable to get vaccinated at higher risk?
Said Prof Cook: "If there are substantial vaccine refusals among those who are able to be vaccinated, it does potentially put those who genuinely cannot be vaccinated for health reasons at risk of harm."
If Singapore is unable to "get below the critical threshold", outbreaks would still happen, he said, and some would reach high-risk unvaccinated people.
While both the Pfizer and Moderna vaccines Singapore is using give very high levels of protection, they are not 100 per cent effective.
"We will be operating in quite tight margins until children can be vaccinated," he added.
For the rest of the population, should unvaccinated people get infected and become severely ill, payment for the cost of their treatment, whether through insurance and/or subsidies, comes out of everyone's pockets.
One solution is to mimic what the Government has done with regard to citizens and permanent residents who left the country after March 27, in spite of warnings not to do so.
For them and others who returned this year, the Government no longer bears the cost of tests, quarantine and any treatment they might need - since it was their decision to leave the country, or not to return within the stipulated period.
They may, however, tap subsidies and claim against their medical insurance if such treatments are covered by their plans.
These people may have had very valid reasons for the timing of their travel or return.
But should people who put themselves at risk of getting the disease, when a vaccine is available, be allowed to use government subsidies and insurance to pay for their tests and treatment?
Since it is their choice not to get the protection offered, they should be willing to bear the consequences of their decision - be it illness or the cost of treating it.
Full coverage would of course be extended to people who are not eligible to be vaccinated, or who get infected in spite of the vaccine.
The Government has already gone the extra mile by offering compensation of $225,000 should there be permanent severe disability or death as a result of getting a Covid-19 vaccine.
It does not do this for any other vaccine, including those on the national immunisation list.
Similarly, to support the vaccination drive, all the insurers offering Integrated Shield Plans will cover any complications arising from the vaccine.
Again, they do not all normally cover for vaccination-related illness or treatments, although the basic MediShield Life does.
Nothing is 100 per cent safe, not even the safest of vaccines.
It is a matter of weighing the risk of taking the vaccine against the risk of getting the disease.
The Health Sciences Authority (HSA) receives around 340 reports a year of vaccine-related adverse reactions. But no one has died here in the past decade as a result of getting vaccinated.
The HSA spokesman said: "Similar to medicines, no vaccine is completely free of side effects.
"Fever, pain or swelling at the injection site and rash are common side effects associated with vaccines such as seasonal influenza and pneumococcal vaccines.
"These are known side effects that are generally associated with vaccinations and usually resolve within a few days."
A recent article in the Journal of the American Medical Association reports that there were 66 cases of anaphylaxis, or severe allergic reaction, out of 17.5 million doses of Pfizer-BioNTech and Moderna vaccines administered between Dec 14 last year and Jan 18 this year.
Of these, 34 were treated in an emergency department.
Of the remaining 32 who were hospitalised, 18 needed intensive care, of whom seven had to be intubated.
This works out to 4.7 cases per million doses for the Pfizer-BioNTech vaccine and 2.5 cases per million doses for the Moderna vaccine.
These are far better odds than the 22,000 deaths per million people infected globally, and 318 deaths per million population.
Even in Singapore where the spread has been relatively well controlled, the Covid-19 fatality rate stands at 485 per million people infected, and five deaths per million population.
No matter how you look at it, it would be better to get vaccinated than to risk getting the disease.
The question that doubters must ask themselves is not what are the risks they face if they take the vaccine, but what are the risks they face by not getting vaccinated once Covid-19 measures are eased - as they surely will, one day.
When that day comes will largely depend on how many people have been vaccinated, and on the vaccine remaining effective against any mutated strains.


