Covid-19 mixed-vaccine regimen requires studies to assess efficacy, safety: Experts
Sign up now: Get ST's newsletters delivered to your inbox
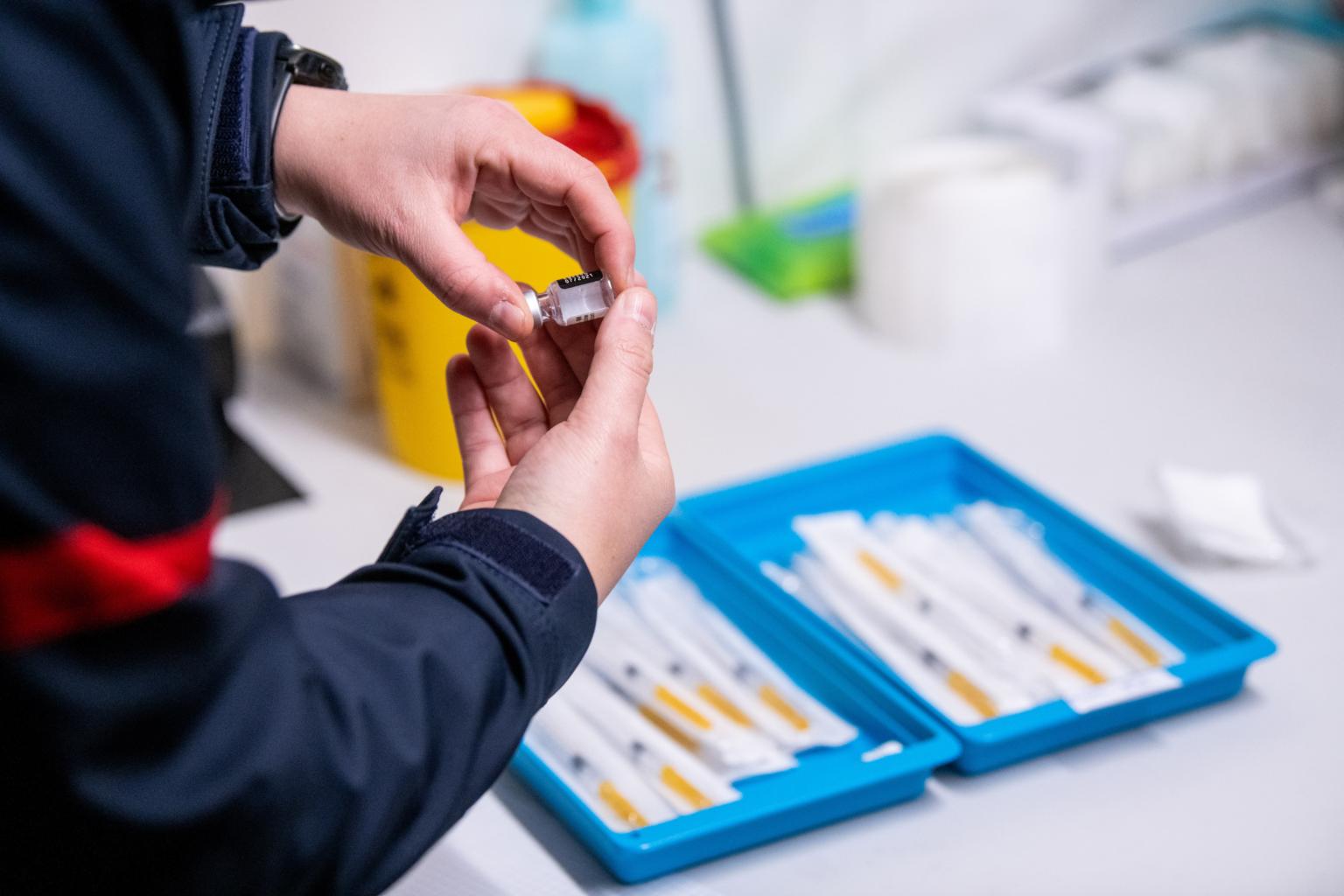
There has not yet been any data from clinical trials to assess the outcome of combining vaccines.
PHOTO: BLOOMBERG
SINGAPORE - Mixing Covid-19 vaccines is possible and could even be beneficial at inciting a more robust immune response to the coronavirus.
But experts warn that more studies are needed to ascertain the effectiveness of such a regime, and to determine that doing so will not produce any side effects.
The experts were responding to queries from The Straits Times, following news that other countries are considering a mixed-vaccine regimen.
Earlier this week, for instance, local media in China reported that the country is considering the mixing of different Covid-19 vaccines for its inoculation programme.
The BBC had reported last December that scientists in Britain and Russia were teaming up to trial a combination of the Oxford-AstraZeneca and Sputnik V vaccines to see if protection against Covid-19 could be improved.
Dr Zenaida Reynoso Mojares, head of vaccine clinical development at the International Vaccine Institute, told ST that the idea of mixing vaccines is still being discussed and studies are under way, to meet emergency needs and possibly assist in the formulation of public health policies in the future.
She added: "Since Covid- 19 vaccines are developed in various platforms, whether or not different vaccines can complement each other to produce positive immune responses cannot be ascertained in the absence of further clinical studies."
Professor Ooi Eng Eong of Duke-NUS Medical School, who is co-developing a Covid-19 vaccine with American firm Arcturus Therapeutics, said that in theory, mixing can take advantage of the strengths of the different forms of vaccines.
For instance, messenger-ribonucleic acid (mRNA) vaccines, such as those from Pfizer-BioNTech or Moderna, can be first administered to train the body to recognise the spike protein of the coronavirus, he said. This will cause the body to generate antibodies and T cells - elements of the human immune system - against the spike protein.
The booster dose can then be a protein sub-unit vaccine, such as the one from Novavax, to refine the antibody response against the virus, Prof Ooi added.
Both vaccines leverage different platforms.
An mRNA vaccine involves injecting a person with snippets of the viral genetic code, which commandeers the human cell to start producing the spike protein of the virus. In this way, the vaccine uses the body as a factory to produce the spike protein - which the immune system recognises as the invader, and begins to mount a response against it.
A protein sub-unit vaccine, on the other hand, contain "ready-made" pieces of the spike protein, which are manufactured in the laboratory.
But Prof Ooi said the main problem with mixing Covid-19 vaccines is that there is no efficacy data to guide such vaccine regimens.
"We would not know if the vaccine efficacy would remain at greater than 90 per cent if the second dose, after the mRNA vaccine is given as a first dose, is anything other than the same mRNA vaccine," he said.
Two vaccines, both mRNA ones, are approved for use in Singapore - Pfizer-BioNTech and Moderna. Clinical trials have shown that both vaccines are more than 90 per cent effective at preventing Covid-19.
Prof Ooi said there has not yet been any data from clinical trials to assess the outcome of combining vaccines.
Dr Mojares added that separate clinical trials will be needed to test for any interference on the immune response as well as safety evaluation.


