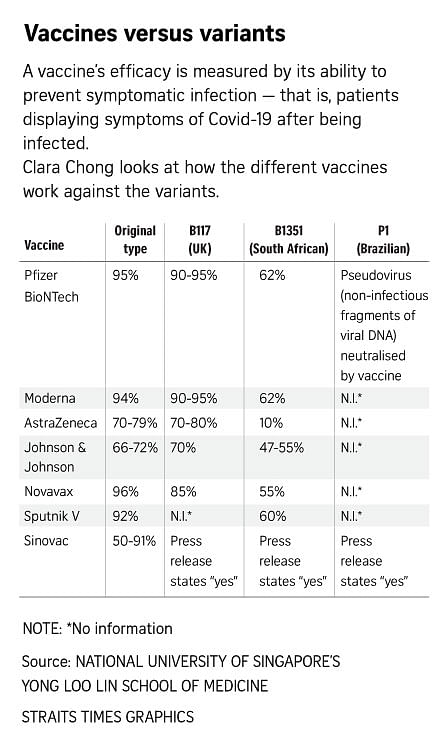
Covid-19 mRNA vaccines best at protecting against variant strains
Sign up now: Get ST's newsletters delivered to your inbox
mRNA vaccines were found to induce high levels of neutralising antibodies.
PHOTO: ST FILE
SINGAPORE - Covid-19 vaccines that use mRNA technology have been found to be the best at preventing symptomatic infection from variant strains, a comparison of the efficacy levels of different vaccines against the variants has shown.
mRNA vaccines, notably the ones developed by Pfizer-BioNTech and Moderna, involve injecting snippets of the virus' genetic material - and not the whole virus - into the body to stimulate an immune response.
mRNA vaccines were found to induce high levels of neutralising antibodies against the original strain, as well as against Britain's B117 strain and the Brazilian P1 variant. However, these levels of neutralising antibodies decline when used against South Africa's B1351 variant.
Neutralising antibodies bind to specific, important sites of the virus, preventing it from starting its invasion.
The success of mRNA vaccines is likely due to the high levels of antibody and T-cell response they induce in the body, according to Associate Professor David Allen from the National University of Singapore's Yong Loo Lin School of Medicine.
"Antibodies have the capacity to block infection entirely... and when it comes to limiting spread and severity of infection in an individual that has already been infected, both T-cells and antibodies play a role," Assoc Prof Allen said.
The more traditional inactivated vaccines make use of killed virus particles. These may elicit lower responses or none at all.
People with low levels of neutralising antibodies may still be protected from Covid-19 if they have robust T-cell immunity.
The immune system depends on the T-cells, a type of white blood cells, working together with antibodies to eradicate the virus.
These findings were shared in a monthly webinar, titled "Season Two of Covid-19: Updates from Singapore'' last Thursday (March 25). The webinar brought together local and international experts to discuss the latest medical and scientific finding around the coronavirus.
The show was hosted by Assoc Prof Allen, who is also the Associate Vice-President of Health Innovation and Translation in NUS; Professor Dale Fisher, group director of Medicine at the National University Health System and chair of the World Health Organisation's Global Outbreak Alert & Response Network (GOARN); and Dr Louisa Sun, an associate consultant with the infectious disease team at the National University Hospital and Alexandra Hospital.
Work on variant-specific vaccines has already started globally, said Dr Richard Hatchett, a special guest of the show. Dr Hatchett is chief executive of the Coalition for Epidemic Preparedness Innovations (CEPI) - an international coalition set up to prepare for future infectious disease threats.
But challenges remain. Although global vaccine-sharing scheme Covax aims to deliver some two billion doses this year, the scarcity in vaccine supply remains the key bottleneck.
"Vaccine supply is a major issue right now that will gradually improve... We have at least nine manufacturers currently that are massively scaling up their production, and those vaccines will become available over time," Dr Hatchett said.
Here are some other highlights from the hour-long webinar:
On allergies
Q: What should individuals with anaphylactic reactions do since they cannot receive the Covid-19 vaccination for now?
A: As the Singapore vaccination programme is still being ramped up, vaccination guidelines will keep being updated. Current vaccination recommendations are unlikely to be the finalised versions. There are also other vaccine candidates which are being currently reviewed. With time, there should be options for everyone to be vaccinated.
Q: Should individuals with chronic stable medical conditions get vaccinated?
A: Yes, they are encouraged to get vaccinated. But if you have a newly diagnosed serious medical condition, and are receiving intense treatment or frequent medication, then you should postpone the vaccination until your condition stabilises.
Q: Can I get vaccinated if I have had surgery in my limbs?
A: Yes you can get vaccinated. But local site reactions are quite common for mRNA vaccines, so it will be good to wait for the post-surgical healing process to be over before proceeding with the vaccination.
On Sinovac
Q: Different trials in different countries have reported different efficacy levels for Sinovac. Is this of concern?
A: Calculating efficacy is a highly complex affair. There is an interplay of different factors such as participation numbers, prevalence and rate of transmission of Covid-19, the presence and effectiveness of existing public health measures as well as testing strategies.
Hence, trials that have been done cannot be compared head to head, as even the recruitment of trial participants has been very different. For instance, Indonesia recruited only the general public while Brazil recruited only healthcare workers. Trials have also been done under very different pandemic situations, with places like Brazil experiencing a very rampant Covid-19 outbreak. Hence, these factors will also influence vaccine efficacy, and official data will be needed from Sinovac before conclusions can be drawn.
The efficacy of mRNA vaccines is also very high and that has unfortunately set the bar unfairly high for other vaccine candidates. A successful vaccine is one that is safe and can achieve an efficacy of over 50 per cent.
The next webinar will be held on April 22.