KUALA LUMPUR - When Madam Fiari Suhaimi and her five-year-old son visited a clinic on the outskirts of Kuala Lumpur in June for a routine check-up, she assumed it had in place health protocols to prevent Covid-19 infections.
Instead, they found themselves in the same waiting room as a family who they later learnt had tested positive for the virus.
Several days later, she, her son and her husband also tested positive, with the Delta variant of the coronavirus.
"We were waiting for our turn at a clinic, when a family of four came out of the consultation room. We continued waiting in the same area as them for about 15 minutes before my son was called in," the administration clerk told The Straits Times (ST).
"We returned to the waiting area after that. That's when we heard the nurse casually telling the family that they had all tested positive and were to self-quarantine at home. I was horrified," she said.
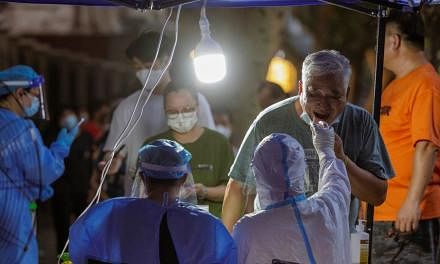
Daily Covid-19 cases in Malaysia have continued to chart record highs, fuelled by the more transmissible Delta strain. On Wednesday (Aug 4), new daily infections spiked at 19,819 cases, the highest since the pandemic began, while the daily death toll hit 257, also a record.
Malaysia's health chief Noor Hisham Abdullah had previously warned that the number of new cases would increase as the Delta variant, which can be easily transmitted by air, has been detected in almost every state.
Madam Fiari, 35, said she had assumed that the clinic would sanitise its premises regularly and keep potential Covid-19 patients in a separate area.
After she and her family tested positive, the health ministry said they might have been exposed to the virus at the clinic. However, only genome sequencing can conclusively pinpoint if they were indeed infected there.
Experts, however, say lax measures at private clinics are not the only factor at play.
"It's not impossible (for it to happen) because most clinics have poor airflow as they were converted from normal shoplots. They don't have a negative pressure room to treat patients with infectious illnesses like in hospitals," Professor Sazaly Abu Bakar, director of the Tropical Infectious Diseases Research and Education Centre at Universiti Malaya told ST.
"GPs have never experienced handling infectious diseases of this scale before, so I don't think it's just poor protocols practised by them," he said, referring to general practitioners.
Professor Sazaly added that GPs must now consider improving their clinics' air circulation and it is something that "needs to permanently change".
"Not just for Covid-19 but also for measles and influenza. Before this, people took these things for granted, but Covid-19 teaches us not to take airflow for granted - it's critical and pivotal," he said, adding that patients should be screened before they enter the clinic.
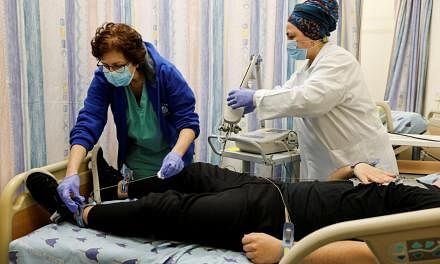
Meanwhile, the fear of randomly contracting the virus has also led some to stop seeking medical help.
Madam Hazlina Hussein, 42, an advertising executive, told ST: "My (six-year-old) son is overdue for his chickenpox vaccine and I have been delaying it because I am very worried about the high number of cases in Kuala Lumpur. I know his vaccine is important, but now that private hospitals are treating Covid-19 patients, I don't know if it is safe to go to one."