WEF aims to make vaccine for Covid-19 a global public good
It is leading network to raise production capacity and ensure equitable access
Sign up now: Get ST's newsletters delivered to your inbox
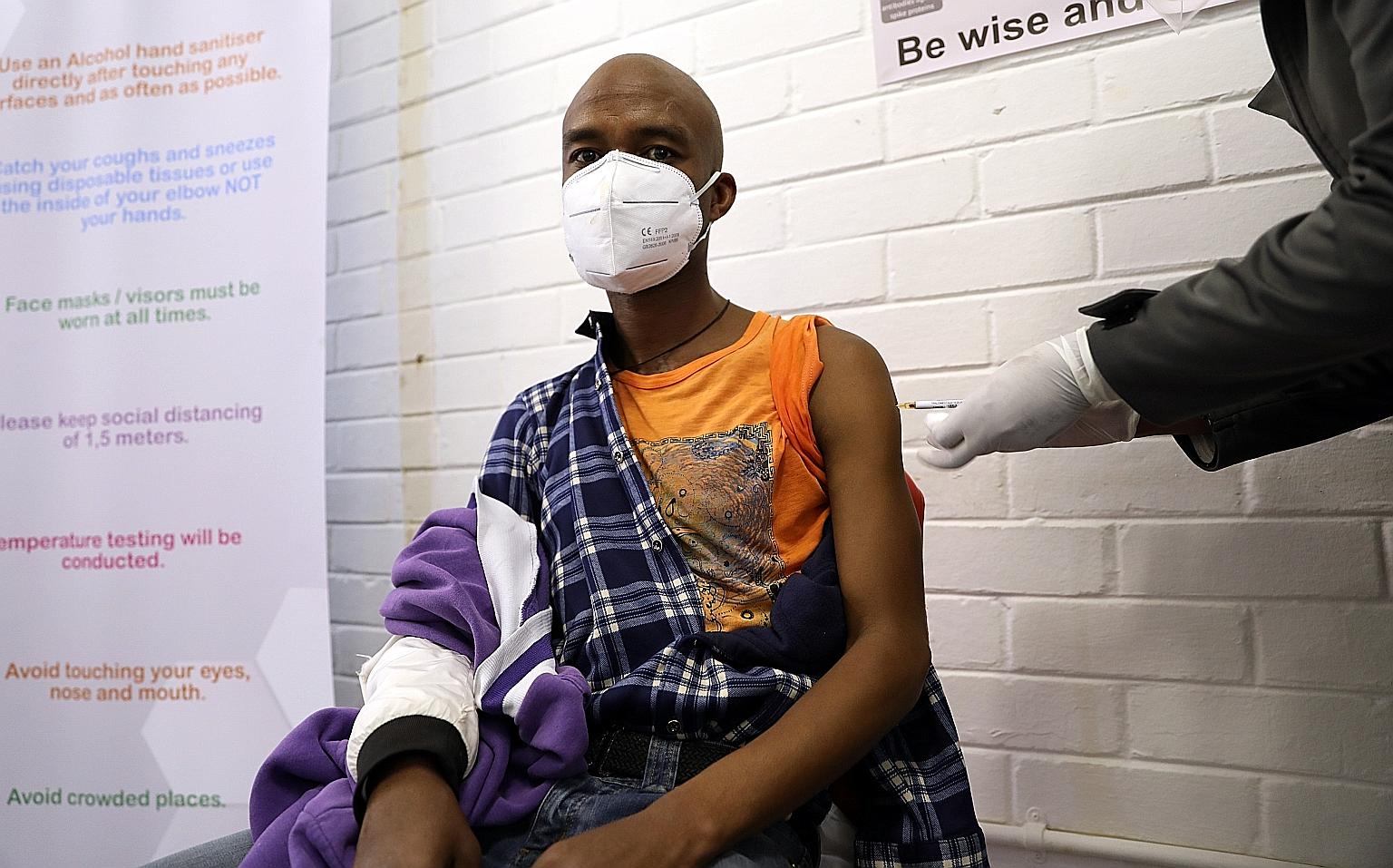
A man getting an injection during a clinical trial for a potential Covid-19 vaccine at the Baragwanath hospital in Soweto, South Africa, on June 24. The world faces problems of how to produce enough vaccines to meet global demand, and how to ensure it is adequately distributed to those who need it most.
PHOTO: EPA-EFE
The world has faced no other crisis in recent times that has so highlighted the need for global cooperation.
As governments continue to battle the coronavirus pandemic amid a spate of new infections, after initial containment, it has become increasingly clear that we will not be able to fully return to life as we knew it until there is a vaccine for the deadly disease.
But even after a vaccine is created, there will be subsequent problems of how to produce enough of it to meet global demand, and how to ensure it is adequately distributed to those who need it most.
The World Economic Forum (WEF) has come up with an ambitious plan to address these issues, seeking to turn a traditional marketplace practice on its head.
Its goal is to make the vaccine a global public good, whose availability and affordability would not be at the mercy of market forces. It would also not cater only to the interests of certain groups or nations.
DITCHING THE OLD WAYS
Key to the plan is the WEF's proposal to depart from the practice of exclusive, bilateral agreements between vaccine researchers and manufacturers.
Instead, manufacturers across the globe would scale up and then pool their production capacities as they are paired with the most promising researchers' vaccines.
Traditionally, exclusive two-way pacts are signed early on in any vaccine development process to maximise profits for both sides. This ties up already-limited global manufacturing capacity before an effective vaccine is even found.
Such agreements also potentially create tremendous amounts of wastage as manufacturers have to start producing large quantities of a promising vaccine candidate, while it is still being tested to ensure it is ready for distribution once proven effective. But if ongoing tests find it unsuccessful at any stage, the doses made will all have to be destroyed.
Meanwhile, researchers whose vaccine candidates prove effective may find themselves bound by such agreements to only a few exclusive manufacturers with production capacity that falls far below the global demand.
-
30m
Number of the first doses of pharma giant AstraZeneca's potential vaccine that Britain has secured.
300m
Minimum number of doses of AstraZeneca's vaccine that the US has pledged up to US$1.2 billion (S$1.7 billion) to obtain.
"Judging by the manufacturing solutions currently being designed for Covid-19 vaccination, the best-case scenario for vaccine delivery outside of the G-7 countries is in the magnitude of a few hundred million doses, when up to four billion doses could be required to address the needs of the most vulnerable populations on the planet," Mr Arnaud Bernaert, head of WEF's Shaping the Future of Health and Healthcare department, told The Straits Times late last week.
"There must be a better way."
This better way, Mr Bernaert posits, can be achieved through a global vaccine manufacturing network.
Known as the Manufacturers Alliance for Global Equitable Access to Coronavirus Vaccines (Manage-Cov) Consortium, the WEF-led network aims to create additional vaccine production capacity of several billion doses for distribution to populations in low-and middle-income countries. It held its first inaugural summit last Friday.
The consortium will create a pairing mechanism between its pool of participating vaccine researchers and manufacturers, so that the manufacturers have the flexibility to select which researchers' vaccine candidates to produce based on each one's progress, rather than be tied down to any one company via an exclusive contract.
Vaccine candidates in the pool for selection would be those that have reached select clinical evidence criteria during the final phase three of clinical trials, when the drug is tested in groups of at least thousands of people across multiple countries.
If a candidate is confirmed safe and effective at this phase, it would be considered ready to be produced for use in large quantities.
BENEFITS FOR ALL
While participants in Manage-Cov's arrangement may forgo their traditional exclusive rights to control supply of a successful vaccine to maximise profits, Mr Bernaert said vaccine researchers "will benefit through access to the manufacturing hubs in the network, financial compensation for knowledge transfer, and revenue from increased market access".
"Vaccine manufacturers will (also) benefit through the option of selecting among a pool of late-stage vaccine candidates, financial support to increase manufacturing capacity, and workforce development and training," he said.
Dr K. Srinath Reddy, president of the Public Health Foundation of India and a member of the Indian Council of Medical Research Covid-19 task force, agrees with the need for such an unconventional arrangement.
"The entire population of the world is susceptible to this new virus," he told ST on Monday. "The financial investment, production capacity and distribution chain needed to immunise the global population will require global solidarity at a level never before witnessed in public health."
To help the most vulnerable populations in developing countries gain access to the eventual vaccine as quickly as possible, plans are being drawn up on how to distribute it.
The WEF is working with leaders in the field of vaccine allocation - such as the World Health Organisation (WHO), the Coalition for Epidemic Preparedness Innovations (Cepi), and Gavi, the Vaccine Alliance - "to ensure optimal distribution in accordance with the principles of universal access, equity and ethical prioritisation", Mr Bernaert said.
It is a lofty ambition.
The pharmaceutical industry is largely driven by profit - to make the most out of its costly research investments, players supply only to those most able and willing to pay for the drug created.
Political leaders, too, are most motivated to secure supply for their own populations first, especially when many of these research projects have been heavily funded by national governments.
Britain has already secured the first 30 million doses of pharma giant AstraZeneca's potential vaccine, the world's front runner in the race for a cure.
Not one to lose out, the United States has pledged up to US$1.2 billion (S$1.7 billion) to obtain at least 300 million doses of AstraZeneca's vaccine as soon as October.
But nation-focused strategies may not be the most effective way to combat a pandemic.
"Unprotected populations anywhere can initiate fresh waves (of the coronavirus)," Dr Reddy said. "The rich countries have to invest in a vaccine for global protection to safeguard themselves, both in terms of their health and economic investments. Subsidising vaccine production for low-and middle-income countries is a small price to pay to achieve these objectives."
Asked if researchers would find sufficient motivation to get on board with such a solution, he added: "Even if some companies or countries seek to establish exclusive rights or erect distribution barriers, the large number of candidate vaccines now under trial suggests that successful vaccines will not be held captive to narrow domestic or commercial interests."
THE MORAL IMPERATIVE
Some state leaders have adopted a more enlightened approach, realising that immunising the world's most vulnerable groups against the coronavirus as soon as possible is one of the most crucial steps towards stopping the global spread of the disease and bringing societies - and economies - back to normalcy.
"A global pandemic requires a coordinated global response, especially in scientific research and government actions," Singapore's Prime Minister Lee Hsien Loong noted in a Facebook post on Sunday.
"We will maximise our chances of tackling Covid-19 by working together," he said.
Others, such as British Prime Minister Boris Johnson, French President Emmanuel Macron and German Chancellor Angela Merkel, have agreed that world leaders have a moral duty to ensure that a coronavirus vaccine is made available to all.
Almost €16 billion (S$25 billion) has been pledged towards the European Union-led Coronavirus Global Response programme, which will help develop coronavirus tests, treatments and vaccines, as well as to support the world's poorest and most marginalised communities.
Recipients of the funds include WHO, Cepi and Gavi - all three of which are working with the WEF to ensure equitable access to an eventual vaccine.
AstraZeneca said early last month that it had also signed agreements with Cepi, Gavi and India's Serum Institute to ensure that its potential vaccine is supplied to low-and middle-income countries.
As the world gradually comes around to recognising the importance of vaccine multilateralism in the long-drawn battle against the coronavirus, India's Dr Reddy puts it well: "No country is safe until every other country is safe."


