Coronavirus: Record rush to find vaccine for Covid-19 is cause for optimism
Sign up now: Get ST's newsletters delivered to your inbox
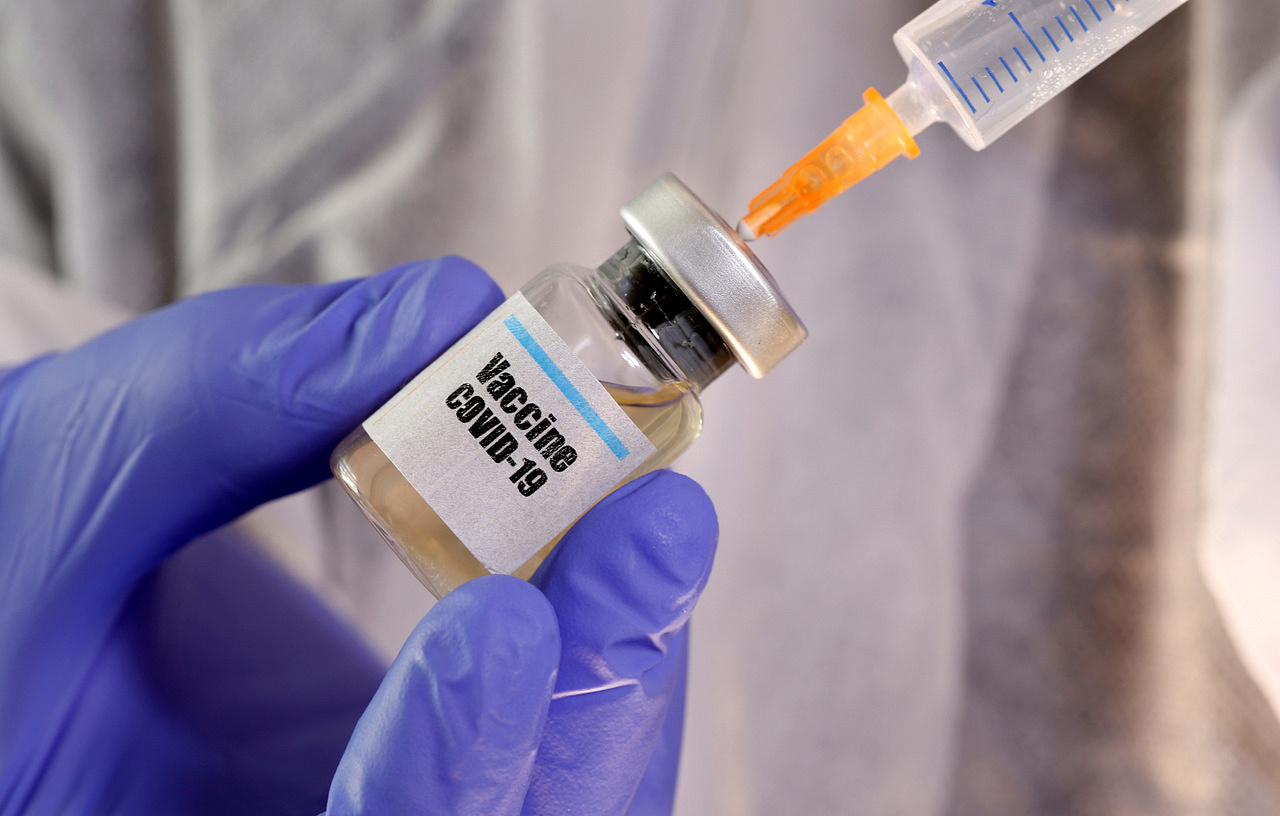
Normally, the timeline for a vaccine is around 10 to 15 years.
PHOTO: REUTERS
WASHINGTON - The Covid-19 crisis has triggered an urgent, unprecedented global effort to develop a vaccine, with the consensus among experts that the earliest one could be available for public deployment 12 to 18 months from now.
According to a paper uploaded on the website of the journal Nature, as of April 8, the global Covid-19 vaccine research and development landscape includes 115 vaccine candidates.
Of these, 78 are confirmed as active and 37 are unconfirmed, meaning their status cannot be determined from publicly available or proprietary information sources.
To be sure, the 12 to 18-month timeline would be unprecedented.
The fastest a vaccine has ever been developed have been the one for mumps (four years) and Ebola (five years).
Normally, the timeline for a vaccine is around 10 to 15 years. In some cases, such as with the HIV virus, vaccine development has been unsuccessful.
BALANCING HOPE WITH REALISM
"Science is science, and we have to be realistic," says Dr Maria Elena Bottazzi, Associate Dean of the National School of Tropical Medicine at Baylor College, which is working to develop a vaccine.
"We have never seen a vaccine develop in an accelerated manner besides those two.
"To tell the people in 12 to18 months we're going to have a vaccine without having the evidence raises hopes," Dr Bottazzi said.
"But that doesn't mean we shouldn't be optimistic or aggressive in our aspirational goal, to say this time we are trying to achieve a goal of two years.
"Scientists can say it is an aspirational goal, we think we could do it, the reality is we have never done it before.
"But today we may be better positioned than maybe five years ago because we have better technology (and) we have had previous experiences with Sars and Mers, so maybe that also can help us."
Sars emerged in 2003 from China and Mers in 2012 from the Arabian peninsula. Both are coronaviruses with high fatality rates, but cases now are rare.
"We should be optimistic because we have been able to achieve goals before, using the Ebola example, though there are other diseases where we have not been able to.
"That doesn't mean we don't try, and we are doing everything possible," Dr Bottazzi said.
"We need to keep high trust that it is possible, but we also don't want to do it too fast in case it damages people and damages the trust that vaccines are the best public health intervention as long as they are done with all the safety protections and we make sure we evaluate carefully the efficacy of the vaccine."
UNPRECEDENTED SCALE AND SPEED
The Nature paper noted: "The global vaccine R&D effort in response to the Covid-19 pandemic is unprecedented in terms of scale and speed.
"Given the imperative for speed, there is an indication that vaccine could be available under emergency use or similar protocols by early 2021.
"This would represent a fundamental step change from the traditional vaccine development pathway, which takes on average over 10 years, even compared with the accelerated five-year timescale for development of the first Ebola vaccine."
This will necessitate novel and innovative vaccine development strategies as well as innovation in regulatory processes and manufacturing capacity, said the authors .
Of the 78 confirmed active projects, 73 are currently at exploratory or pre-clinical stages, the paper said.
"The most advanced candidates have recently moved into clinical development, including mRNA-1273 from Moderna, Ad5-nCoV from CanSino Biologicals, INO-4800 from Inovio, LV-SMENP-DC and pathogen-specific aAPC from Shenzhen Geno-Immune Medical Institute."
"Of confirmed active vaccine candidates, 56 (72 per cent) are being developed by private/industry developers, with the remaining 22 (28 per cent) of projects being led by academic, public sector and other non-profit organisations," the paper said.
"Although a number of large multinational vaccine developers… have engaged in Covid-19 vaccine development, many of the lead developers are small and/or inexperienced in large-scale vaccine manufacture," it added, stressing that it will be important to ensure coordination of vaccine manufacturing and supply capability and capacity to meet demand.
PHASE ONE TRIAL
Several vaccine developers have plans for human testing this year. One of them is the Emory Vaccine Centre at the Emory University School of Medicine in Atlanta, Georgia.
Emory University is one of 10 sites that have facilitated testing of vaccines and therapeutics for infectious diseases in particular, for decades. It is currently in phase one trials of a vaccine.
"This particular vaccine was actually developed by NIH (National Institutes of Health, in Bethesda, Maryland) and by Moderna," explained Dr Nadine Rouphael, Associate Professor at the Division of Infectious Diseases at the Emory University School of Medicine.
"And then the manufacturing of this vaccine was supported by the Coalition for Epidemic Preparedness and Innovation."
Dr Rouphael told The Straits Times that in this phase one trial - the first time the vaccine has been given to humans - 45 subjects between the age of 18 and 55 will be enrolled.
"They will receive two doses, separated by four weeks. And really the idea here is to make sure that this vaccine is safe.
"We will also gather information about how their immune system will respond to the vaccine in preparation for future phase two and phase three trials.
"We don't know if the vaccine can protect from infection. But we're checking to make sure it's safe.
"A normal vaccine might take up to 10 years to have a candidate that's used by the general public," Dr Rouphael said.
"I think the timelines here are much more compressed, obviously because of the urgency of the pandemic."


