Risk of dangerous blood clots linked to moderate Covid-19: European study
Sign up now: Get ST's newsletters delivered to your inbox
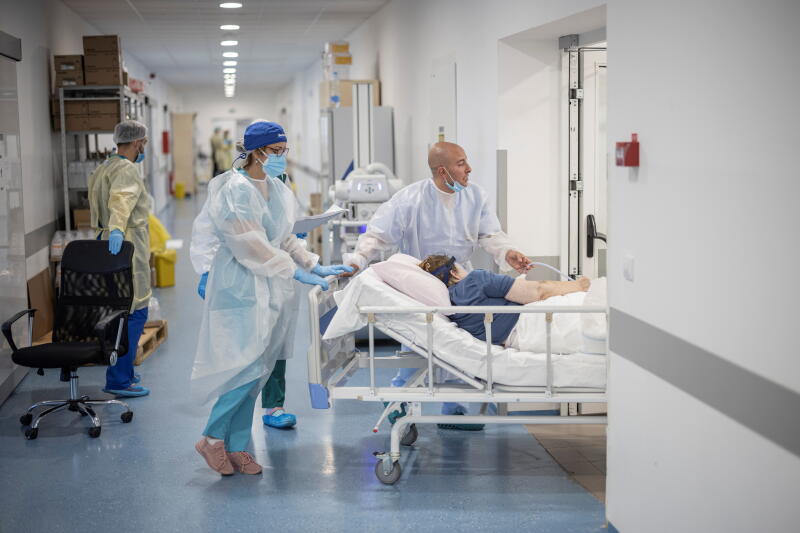
The researchers tracked 2,292 patients who came to hospital emergency rooms with mild or moderate Covid-19 but without VTE.
PHOTO: REUTERS
LONDON (REUTERS) - A European study has found an elevated risk of a life-threatening blood clot called venous thromboembolism (VTE) in Covid-19 patients who were not critically ill.
The blood clot risk had previously been associated with severe Covid-19. The researchers tracked 2,292 patients who came to hospital emergency rooms with mild or moderate Covid-19 but without VTE.
Four weeks later, VTE had developed in roughly one of every 200 mildly ill patients who had not been hospitalised and nearly five of every 200 moderately ill patients overall, the researchers reported on Friday (Oct 8) in Thrombosis Research.
They conclude that doctors caring for mildly and moderately ill Covid-19 patients need to be aware of these risks, "especially in patients with moderate Covid-19 requiring hospitalisation".
In hospitalised, moderately ill Covid-19 patients who have high levels of the d-dimer protein in their blood - indicating a higher-than-average risk for dangerous blood clots - treatment with high doses of the blood thinner low-molecular weight heparin (LMWH) significantly reduced the odds of clot formation and death, according to data from a clinical trial.
The incidence of VTE or death was 28.7 per cent in the high-dose group, compared with 41.9 per cent in patients getting a standard dose.
After accounting for patients' various risk factors, that was a 32 per cent reduction in risk with high-dose heparin, the researchers said on Monday in a report published in JAMA Internal Medicine.
The researchers said they launched the trial "because we saw patients getting blood clots and dying in front of us while on standard doses of preventative heparin," said study leader, Dr Alex Spyropoulos of the Feinstein Institutes for Medical Research in New York.
"We were able to prove... that d-dimer levels more than four times the upper limit of normal are able to predict a very high-risk group of hospitalised Covid-19 patients - and giving therapeutic doses of heparin in these patients works," Dr Spyropoulos said.
"This is practice changing now."


