Singapore scientists create blood cells from skin cells
Sign up now: Get ST's newsletters delivered to your inbox
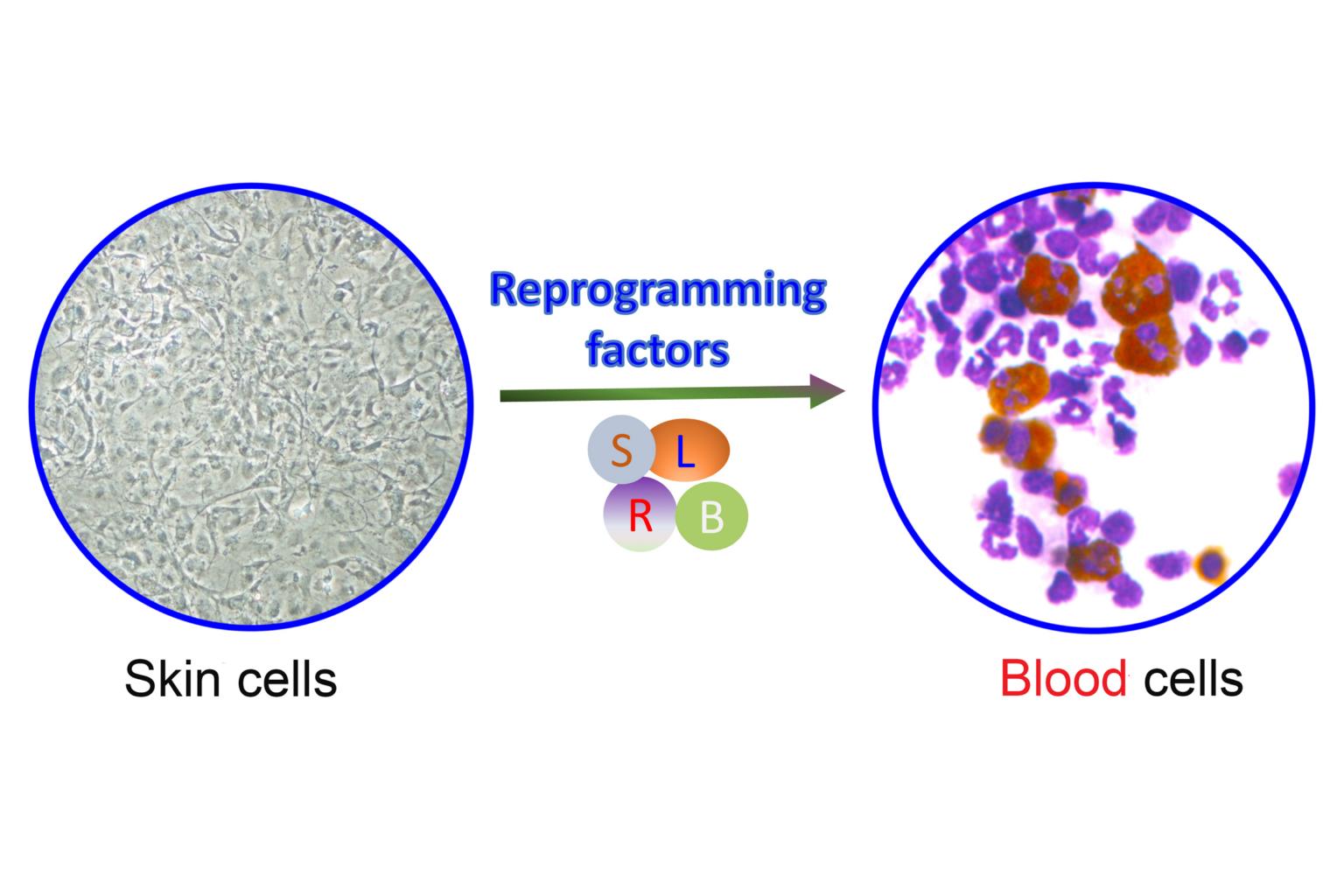
A*Star scientists have succeeded in making blood cells from mouse skin cells through "direct reprogramming" - adding to the skin cells a mixture of chemicals that normally occur in blood cells.
PHOTO: Genome Institute of Singapore, A*Star
Singapore scientists have transformed skin cells into blood cells in mice and are going to try to apply the technique to human cells.
The conversion can potentially lead to a robust source of new red or white blood cells to treat patients who need blood transfusions or have immune disorders.
The study, led by researchers from the Agency for Science, Technology and Research's (A*Star) Genome Institute of Singapore (GIS) and Institute of Molecular and Cell Biology, was published earlier this week in the journal Nature Communications.
They said it is a major challenge of regenerative medicine to make new blood cells for healthcare needs. While there were previous efforts to generate mouse blood cells from skin cells, the resulting cells lasted only two weeks once injected back into mice. In contrast, the blood cells made in the latest study held out for several months.
The researchers changed skin cells to blood cells by adding to the skin cells a "cocktail" of four chemicals that normally occur in blood cells. "On the face of it, skin cells and blood cells couldn't be more different from each other," said Dr Cheng Hui, the lead author.
Dr Kyle Loh, a former GIS intern who is now at Stanford University's School of Medicine, said: "This is not only of practical importance for regenerative medicine... but it is also interesting from a fundamental biological perspective that two very different cells - skin and blood - can be interconverted."
In 2010, scientists in Canada converted human skin cells into various blood components, including red and white blood cells and platelets, using similar methods to the latest study.
But the Canadian study's reproducibility is debatable, said Dr Jonathan Loh Yuin-Han, one of the A*Star study's co-authors. "Six years after its publication, we have not come across another study which can repeat it."
GIS' executive director, Professor Ng Huck Hui, said of the A*Star study: "If researchers (can) extend what they did with the mice to human cells in the foreseeable future, it can translate into tangible benefits for the patients in need."
The prospects of human cell conversion go beyond skin and blood. In January, a global team including researchers from the Duke-National University of Singapore Medical School developed a "world atlas" program that uses big data to rapidly determine what chemicals are needed for converting almost 200 different types of human cells.


