SGH creates portable chambers that convert wards, ICUs into negative pressure isolation rooms
Sign up now: Get ST's newsletters delivered to your inbox

Dr Tan Zihui, associate consultant at SGH's department of anaesthesiology, entering a medical ICU fitted with the SG-Sparc system.
PHOTO: SINGAPORE GENERAL HOSPITAL
SINGAPORE - A hospital has created portable systems that can convert wards, intensive care units (ICU) and operating theatres into negative pressure isolation rooms within hours to house patients with infectious diseases.
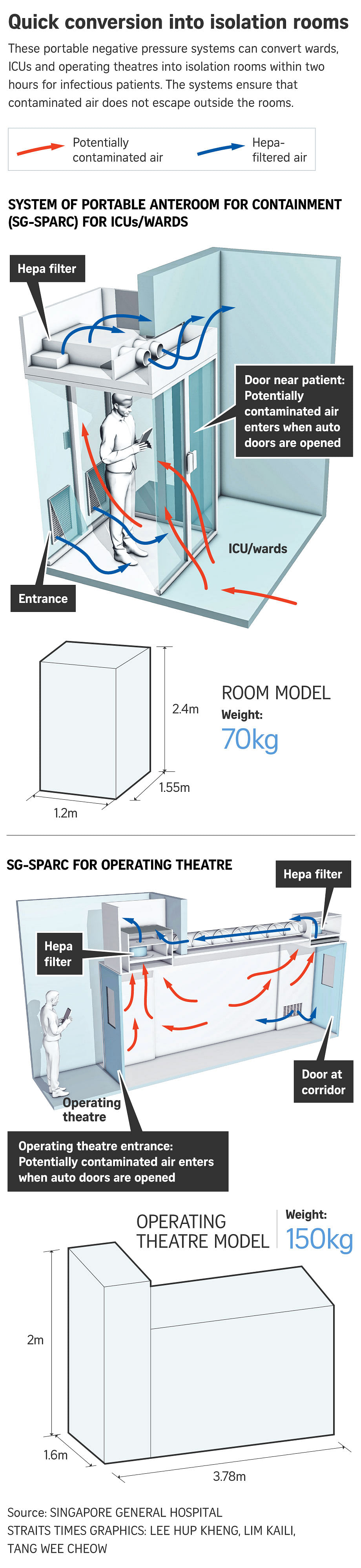
One of the two transparent chamber-like systems at Singapore General Hospital (SGH), called the System of Portable AnteRoom for Containment (SG-Sparc), can be fitted behind the entrance of a ward or ICU. It measures 1.2m by 1.6m, and is 2.4m high.
After any gaps between the entrance and the system are sealed, a Hepa filter unit at the top of the system is powered up to create a negative pressure environment within the patient's room, so that infectious droplets and air from the room cannot seep outside into the corridors.
The chamber has two doors, one at the entrance of the ward and one inside the ward, facing the patient. When the inside door opens for medical staff to enter or leave the room, contaminated air flows into the chamber and through the Hepa filter, so that clean air re-enters the room.
The 70kg system takes an hour to set up and was installed at SGH's Medical ICU in July. One more of the same type will be added to the Medical ICU soon.
The collapsible SG-Sparc can also be fixed to single- and multiple-bed wards with infectious diseases patients. The size of the system is customisable, and each takes two weeks to fabricate.
The other SG-Sparc system, used in operating theatres, is larger to allow an ICU bed, ventilator and medical staff to pass through. Measuring 3.8m by 1.6m and with a height of 2m, the system prevents droplets from escaping the room while surgical operations, including aerosol-generating procedures, are performed on infectious patients.
The 150kg chamber takes two hours to set up. One system has been installed in an operating theatre in SGH.

The two systems were developed by anaesthesiologists from SGH, in collaboration with local biomedical incubator The Biofactory. The project was funded by SingHealth Duke-NUS' Urgent Covid-19 Research Fund, with contribution from The Biofactory.
Compared to existing systems, SG-Sparc has a combination of advanced features such as contactless sensors and a higher rate of air filtration, which makes it the first of its kind, said Dr Mavis Teo, a consultant at SGH's Department of Anaesthesiology.
In a room fitted with the system, the air can be filtered up to 300 times an hour, compared to an operating theatre where the air is filtered 12 times an hour. Medical staff can open the system's doors by waving at the sensor without touching it.
The inventions come at a time when existing numbers of isolation rooms abroad are insufficient to support the Covid-19 surge. It is also costly and time-consuming to build isolation rooms.
An SG-Sparc system costs half as much as renovating an ICU room into an isolation room, said Mr Gabriel Tan, The Biofactory's programme director.
Said Dr Teo, who is the project's co-investigator: "We have seen how hospitals in Italy, in the UK and USA - all quite well-developed countries - struggled when they ran out of negative pressure isolation rooms during the Covid-19 pandemic."
"It got us thinking if there is a way for us to very quickly and temporarily convert existing patient rooms, especially ICU rooms, to care for infectious patients when the need arises," she added.
SG-Sparc has received strong interest from local and overseas hospitals, said Mr Tan.
To ensure and test the system's ability to contain viruses, scientists from the Agency for Science, Technology and Research's Institute of Bioengineering and Nanotechnology released live non-pathogenic viruses into a simulated patient room installed with SG-Sparc. No microbes escaped from the room.
SG-Sparc is the third collaboration between SGH and The Biofactory, after SG-Safe, a foldable swab test system, and SG-Safer, an isolation X-ray booth.