ScienceTalk: The science behind a Covid-19 RNA vaccine
Sign up now: Get ST's newsletters delivered to your inbox
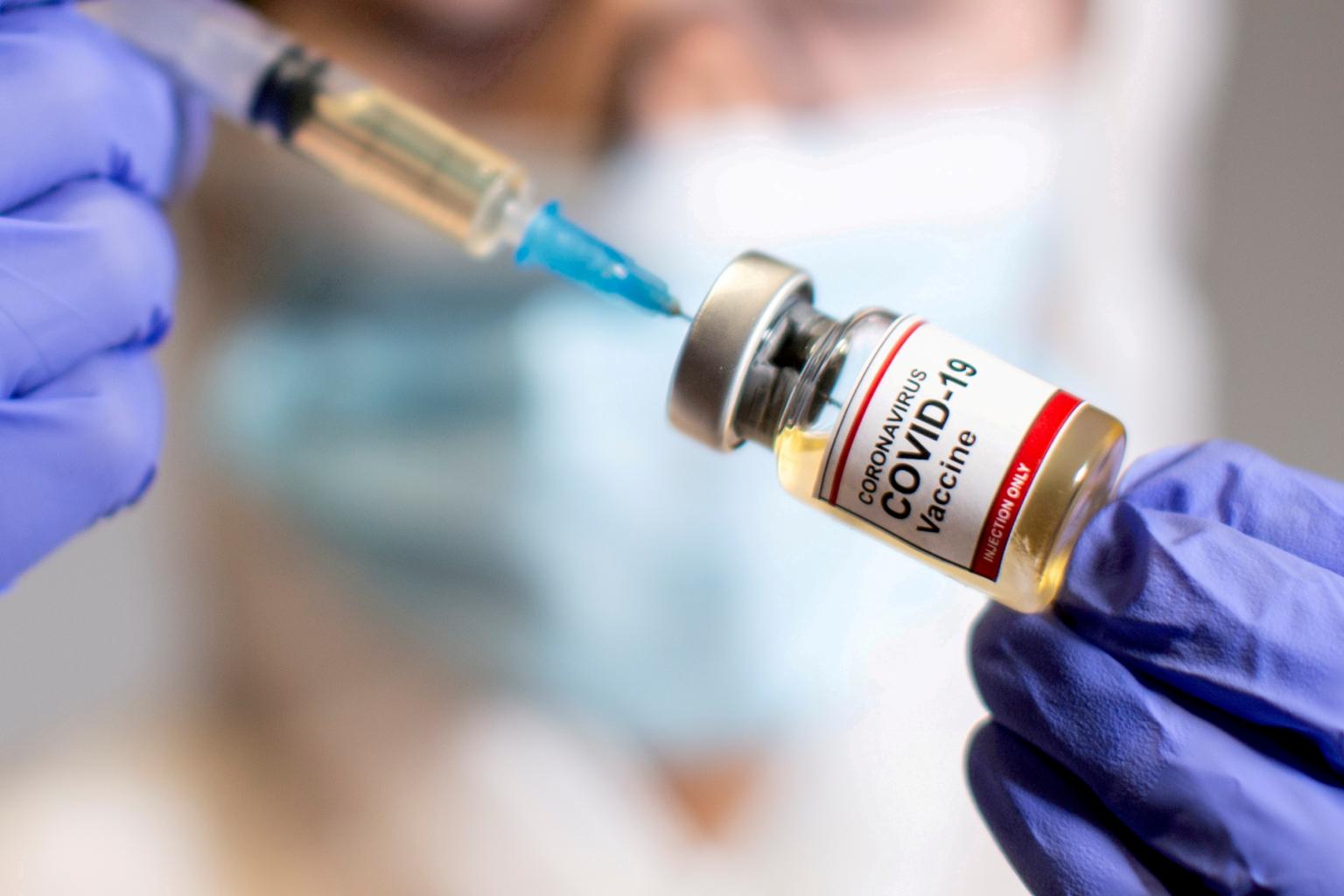
Many commonly used vaccines also contain RNA. Live viral vaccines all contain viral RNA.
PHOTO: REUTERS
Ooi Eng Eong and Eugenia Ong For The Straits Times
Follow topic:
SINGAPORE - In just 10 months, a vaccine developed by Pfizer and BioNTech has been approved by Britain for emergency use to prevent Covid-19. Another by Moderna is being evaluated for emergency use authorisation by several regulators, including the United States Food and Drug Administration (FDA).
This 10-month timeline for vaccines to get from concept to licensing is ground-breaking; most take more than 10 years to reach this stage.
Both these vaccines deliver the spike gene of Sars-CoV-2, the cause of Covid-19, in the form of RNA or ribonucleic acid.
This allows the body to recognise and fight the virus should it try to infect the person.
There are several other RNA vaccines in the pipeline, including the one our team at Duke-NUS Medical School is working on in partnership with Arcturus Therapeutics. Here is the science behind such vaccines:
How RNA vaccines work
In the case of Sars-CoV-2, RNA vaccines contain the genetic code for the characteristic spike protein of the virus.
When they are injected into our bodies, our cells read the code, and produce and present the spike protein to our immune system. Our immune system then reacts and develops memory immune cells to respond specifically to the Sars-CoV-2 spike protein.
Upon Sars-CoV-2 infection, the memory immune cells will be quickly activated to shut down infection and prevent us from getting Covid-19.
Such vaccines contain only the spike gene of the virus, but lack the other Sars-CoV-2 genes required to generate new viruses, so vaccination will not cause the virus to spread in the body or make a person infectious.
The vaccines, however, will very likely remain effective against the many mutations of the virus because the immune system is able to recognise and target many different parts of the spike protein.
Although RNA vaccines have not been licensed for use in humans previously, they have been tested in clinical trials with excellent safety profiles so far.
Many commonly used vaccines also contain RNA. Live viral vaccines, such as the yellow fever vaccine - arguably the best vaccine in the world today, along with measles, mumps and rubella vaccines - all contain viral RNA. Despite that, these vaccines are among the safest and most effective vaccines in the world.
Side effects
Some who took part in Covid-19 vaccine clinical trials have experienced pain from the injection. Some also experienced transient redness and mild swelling at the injection site.
Systemic side effects, such as headache and low-grade fever, are also common following vaccinations. This is mostly caused by our immune response. Our immune cells talk to one another by secreting chemicals. These naturally produced chemicals, besides shaping the immune response, do also have unintended effects.
A common one that we all encounter when our immune system responds to a viral infection is the metallic taste in our mouths. However, all these side effects are mild.
It is important to note that these side effects have come from phase one trials, which test a range of doses to find the highest vaccine dose that can be given to maximise immune response while keeping side effects tolerable.
In contrast, a Phase 3 trial would test only a fixed dose that balances the benefit of immunisation while minimising side effects.
Lasting protection
We do not know how long immunity will last following vaccination. It is possible that it could wane with time and we may need booster shots.
The public health authorities carry out surveillance to detect Covid-19 among vaccinated individuals, should this happen.
Such surveillance would guide decision making on whether and when booster doses should be given to sustain immunity.
The journey to developing a Covid-19 vaccine has been truly remarkable. It now adds a vital piece to our ability to push back Covid-19 and bring the pandemic under control. However, vaccines do not save lives. Vaccination does.
About the writers:
Prof Ooi is a clinician-scientist and a Professor in the Programme in Emerging Infectious Diseases, Duke-NUS Medical School. He is also the Co-Director of the Viral Research and Experimental Medicine Centre (ViREMiCS) within the SingHealth Duke-NUS Academic Medical Centre. He is Duke-NUS' principal investigator of the partnership with Arcturus Therapeutics to develop Lunar-CoV19 as a Covid-19 vaccine.
Dr Ong is a Senior Research Fellow in the Programme in Emerging Infectious Diseases and ViREMiCS. She is leading the effort to apply genomic analyses to evaluate the performance of Lunar-CoV19 in clinical trials.

