NTU scientists discover how brain generates energy to clear waste linked to Alzheimer’s
Sign up now: Get ST's newsletters delivered to your inbox

(From left) PhD student Lai Kei Onn, Nanyang Assistant Professor Anna Barron and research fellow Wong Jia Hui are part of the team of 12 researchers from NTU who discovered how the brain powers the clearing of waste.
PHOTO: NTU
SINGAPORE - A team of 12 researchers from Nanyang Technological University (NTU) has shed light on how immune cells in the brain produce energy to clear toxic waste which would otherwise build up to cause Alzheimer’s disease.
The team’s discovery, which was published in the journal Proceedings Of The National Academy Of Sciences on Feb 14, could lead to the development of new drugs to treat Alzheimer’s, for which there is no cure yet and which accounts for 60 to 70 per cent of dementia cases, according to the World Health Organisation.
In Singapore, there were 82,000 people living with dementia in 2018 and this number is expected to increase to 152,000 by 2030.
One key indicator of the disease is the build-up of protein plaques between nerve cells in the brain.
Led by Nanyang Assistant Professor Anna Barron from NTU’s Lee Kong Chian School of Medicine, the team found that there are two ways microglia cells in the brain generate energy to clear the protein plaques.
The first way is through a specific protein known as the translocator protein. Found in the power-generating parts of cells known as mitochondrion, the study showed that this protein is critical for the microglia to generate their own energy to clear the toxic waste.
In mice with Alzheimer’s disease that had the protein genetically removed, the microglia could not produce enough energy to clear the toxic waste, resulting in the disease worsening.
“We found that microglia lacking the translocator protein resembled damaged microglia observed in ageing and Alzheimer’s disease,” said Prof Barron.
In the absence of the translocator protein, the microglia cells produce energy through a second method, using an enzyme known as hexokinase-2. This enzyme binds onto the mitochondrion in the microglia cells. It then converts sugars into energy that can be used for clearing the brain’s waste.
But this method was found to be inefficient and prevented the microglia from clearing the waste effectively. The researchers also discovered that this second method was activated when microglia cells were exposed to more toxic forms of brain waste, just as it happens in Alzheimer’s disease.
The team said this could help explain how microglia fail in patients with Alzheimer’s and when people age.
The researchers then tried to find a way to stop the microglia from using hexokinase-2 to produce energy. They suspected it had something to do with the hexokinase-2’s ability to stick to the microglia cells’ mitochondrion, which they sought to “switch off”.
To “switch on and off” this sticking ability easily, the scientists genetically modified microglia cells extracted from mice so that when blue light was shone on them, the hexokinase-2’s sticking ability was turned off.
The scientists found that when the enzyme lost its ability to stick to the mitochondrion, the microglia cells were forced to stop using the inefficient method of energy production, improving their ability to clear the waste by nearly 20 per cent.
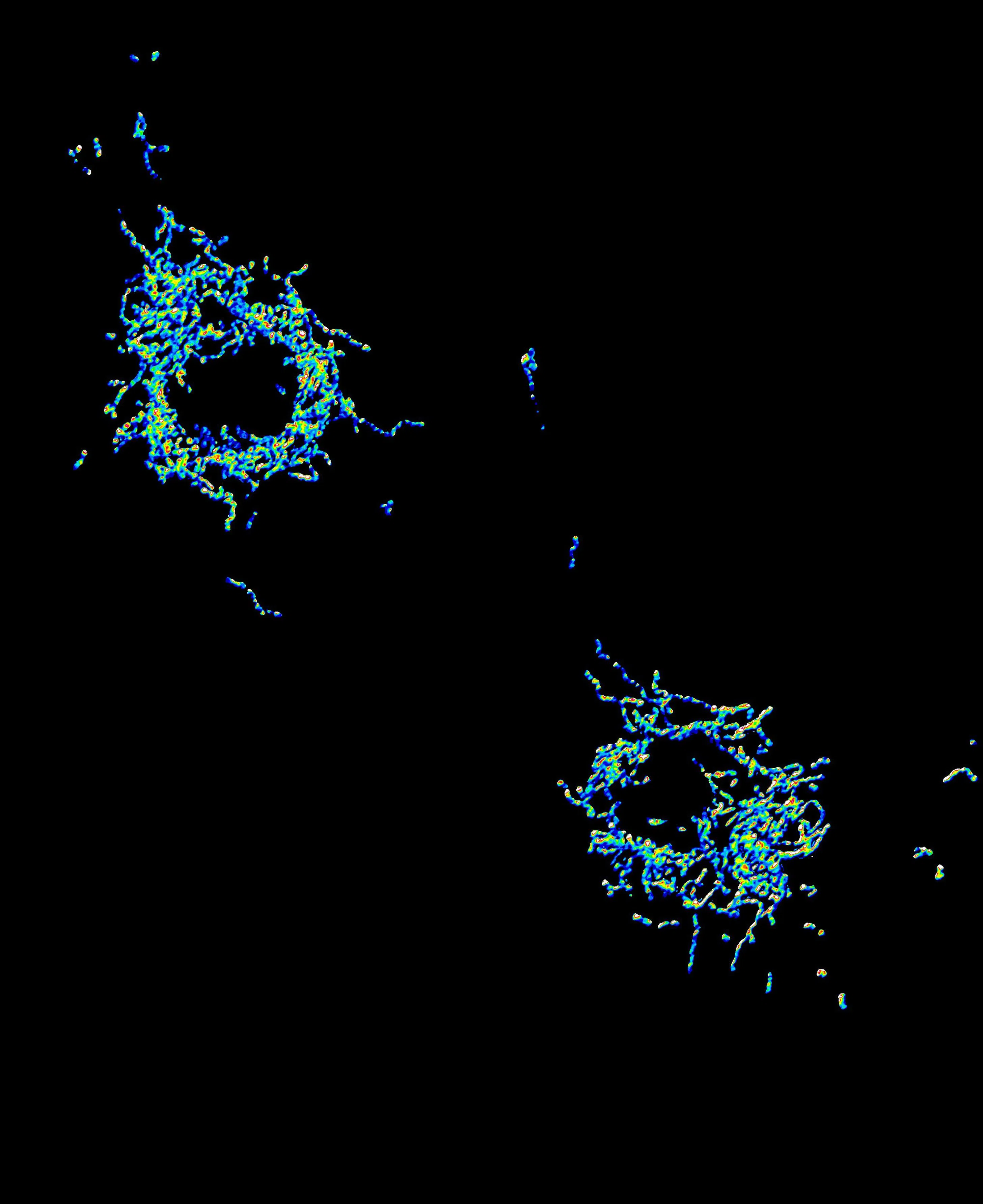
An image showing the enzyme hexokinase-2 stuck all over the mitochondria of brain immune cells called microglia. Mitochondria are the power stations of cells.
PHOTO: NTU
Prof Barron said that her team’s findings provide a basis for them to develop drugs that can act specifically on how the microglia cells produce energy in order to curb Alzheimer’s.
For example, such drugs could target the hexokinase-2 enzyme’s ability to “stick”.
Dr Yeo Tianrong, a senior consultant neurologist at Singapore’s National Neuroscience Institute who was not involved in the research, said that Prof Barron and her team were able to gain new insights into how microglia generated energy to remove waste in the brain.
Said Dr Yeo: “The study by Prof Barron’s team highlights the possibility that, one day, we can harness the intrinsic capability of microglia to mop up the brain’s toxic waste by re-configuring its energy generating framework.”


