Not just coughing and sneezing - talking and singing can also spread Covid-19: NUS study
Sign up now: Get ST's newsletters delivered to your inbox
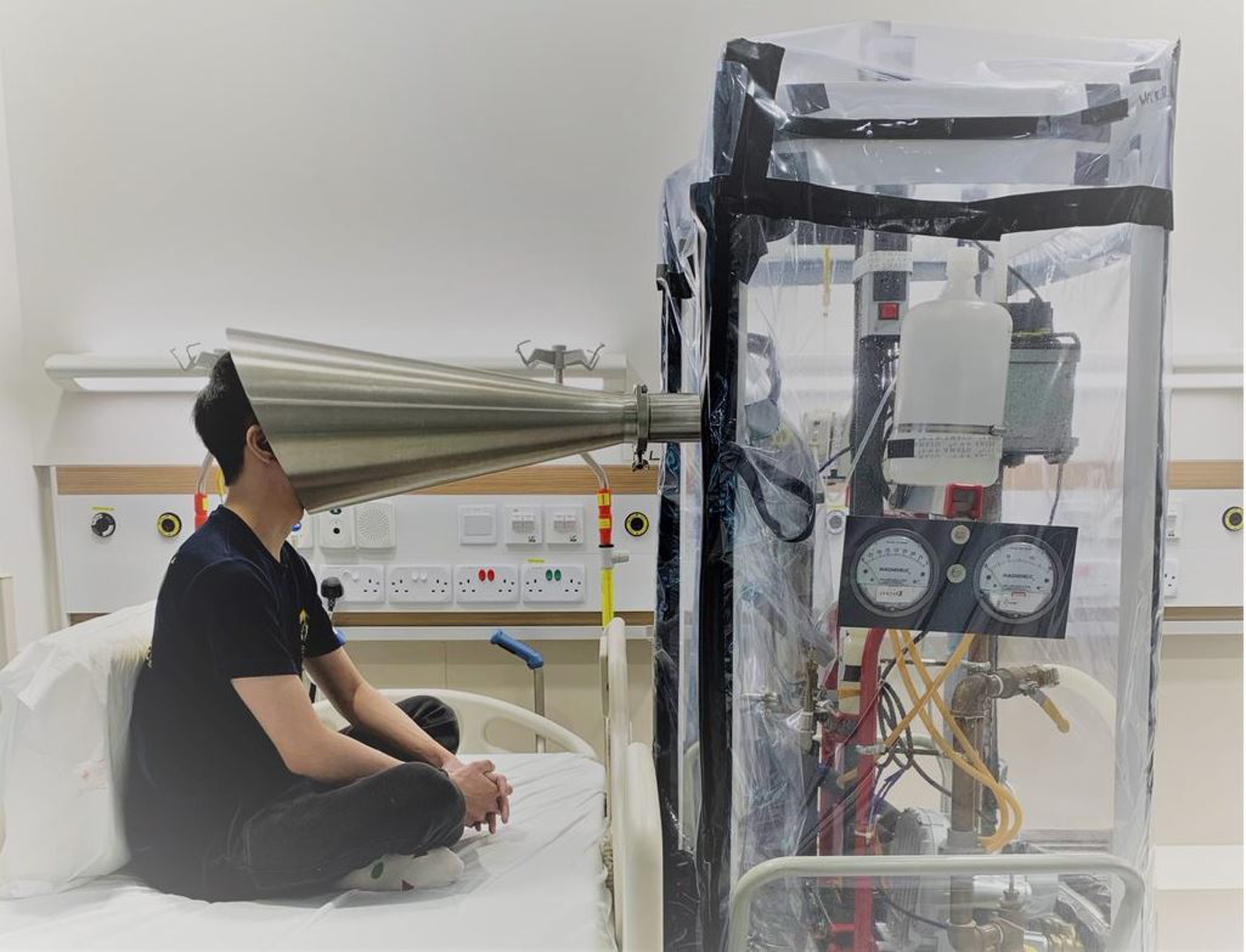
NUS researcher Douglas Tay in a hospital room at the NCID demonstrating how the Gesundheit-II exhalation aerosol particle collection equipment is used.
PHOTO: NATIONAL UNIVERSITY OF SINGAPORE
SINGAPORE - A new study by a National University of Singapore (NUS) team has found that an infected person can spread Covid-19 by exhaling fine aerosol particles when breathing, talking and singing, not just though droplets when coughing or sneezing.
The authors of the study on Wednesday (Aug 11) said the research findings reinforce the need for infection control measures - such as social distancing, mask-wearing and increased room ventilation - especially in an indoor environment, where airborne transmission of the virus is most likely to occur.
The study, led by researchers from NUS and conducted at the National Centre for Infectious Diseases (NCID), showed that talking and singing can produce two types of viral particles - fine aerosols (less than 5 micrometres in size), and coarse aerosols (larger than 5 micrometres).
The fine aerosols generated from both types of activities contained more viral particles than coarse aerosols, said Professor Paul Tambyah, an infectious diseases expert from the NUS Yong Loo Lin School of Medicine.
Prof Tambyah, a co-author of the paper, said while there was no linear relationship between the size of an aerosol particle and the amount of virus it carries, the size can give researchers a clue as to how much virus or parts of a virus are present in an aerosol particle.
Associate Professor Tham Kwok Wai, from the Department of the Built Environment at the NUS School of Design and Environment, said while previous studies had established the relative amount of aerosols produced through breathing, talking, and singing, none of them measured the amount of Sars-CoV-2 virus particles each activity can to generate.
"Therefore, our team's work provides a foundation for estimating the risk of transmission of infection (for each activity)," said Prof Tham, who was the leader of the study.
The paper was first published online in the journal Clinical Infectious Diseases on Aug 6.
The team had studied 22 Covid-19 patients who were admitted to the NCID from February to April. Each of them was asked to perform, on the same day, three separate activities that involved exhaling air, which produced respiratory particles.
The activities were 30 minutes of breathing, 15 minutes of talking in the form of reading aloud passages from a children's book, and 15 minutes of singing different songs.
They rested between the activities.
While the participants were carrying out these activities, a specially designed equipment known as the Gesundheit-II was used to collect the respiratory particles that were generated.
The participants were required to place their head at the cone-shaped inlet of the equipment. The cone served as a ventilation hood where air was continuously drawn around the participant's head, allowing the collection of particles exhaled into the connecting sampler.
Aerosols were collected in two sizes - coarse and fine. The sample viral load was then quantified using a method known as reverse transcription-quantitative polymerase chain reaction (RT-PCR).
Project co-leader Kristen Coleman, from the Duke-NUS Medical School, said: "We observed that Covid-19 patients who are early in the course of illness are likely to shed detectable levels of Sars-CoV-2 RNA in respiratory aerosols."
However, the amount of virus expelled from talking and singing varied among patients, she noted.
"Some released more virus from talking, as they may have spoken loudly during the experiments, though the underlying reason for why their viral loads were higher compared to singing, still remains unclear," Dr Coleman added.
Studying super spreaders
Prof Tambyah noted that swab samples from two of the 22 patients had such high viral loads that their samples accounted for half the total amount of virus collected in the study.
This was despite the fact that all the participants had low CT (cycle threshold) values, which would presumably signal high viral loads in their diagnostic swab tests.
The CT value refers to the number of cycles it takes for the RT-PCR test to detect the virus.
A patient with a high viral load suggests that he is still incubating the virus and is infectious.
"This reflects the phenomenon of (virus) dispersal or super spreaders and hopefully the next phase of the study will help us better understand this phenomenon," Prof Tambyah said.
He added that the amount of virus collected in the aerosol particles in the recent study was too low and attempts to culture the virus proved unsuccessful.
Reduce exposure
The authors said to reduce one's exposure to fine-particle aerosols in indoor environments, the existing safe management measures are important, along with increased room ventilation and more efficient air-cleaning technologies.
"In situations involving singing, safe distancing among singers, as well as the averting and filtering of airflow from choir to audience, such as by deploying air curtains, are important considerations.
"For situations involving talking, determining airflow patterns and minimising exposure through seating and furniture configurations, distancing, and air movement alteration, such as the use of fans, including desk fans, are practical options that can be taken to lower the risk of Sars-CoV-2 transmission," said Prof Tham.
The researchers are now looking to establish the infectiousness of airborne aerosols, or live virus, that is emitted through talking by infected people.
They are also planning to use the same methods to determine if the aerosol viral load associated with the new variants - especially the Delta variant - is higher than previous strains.


