New programme to improve standard of emergency care outside of hospital
Sign up now: Get ST's newsletters delivered to your inbox
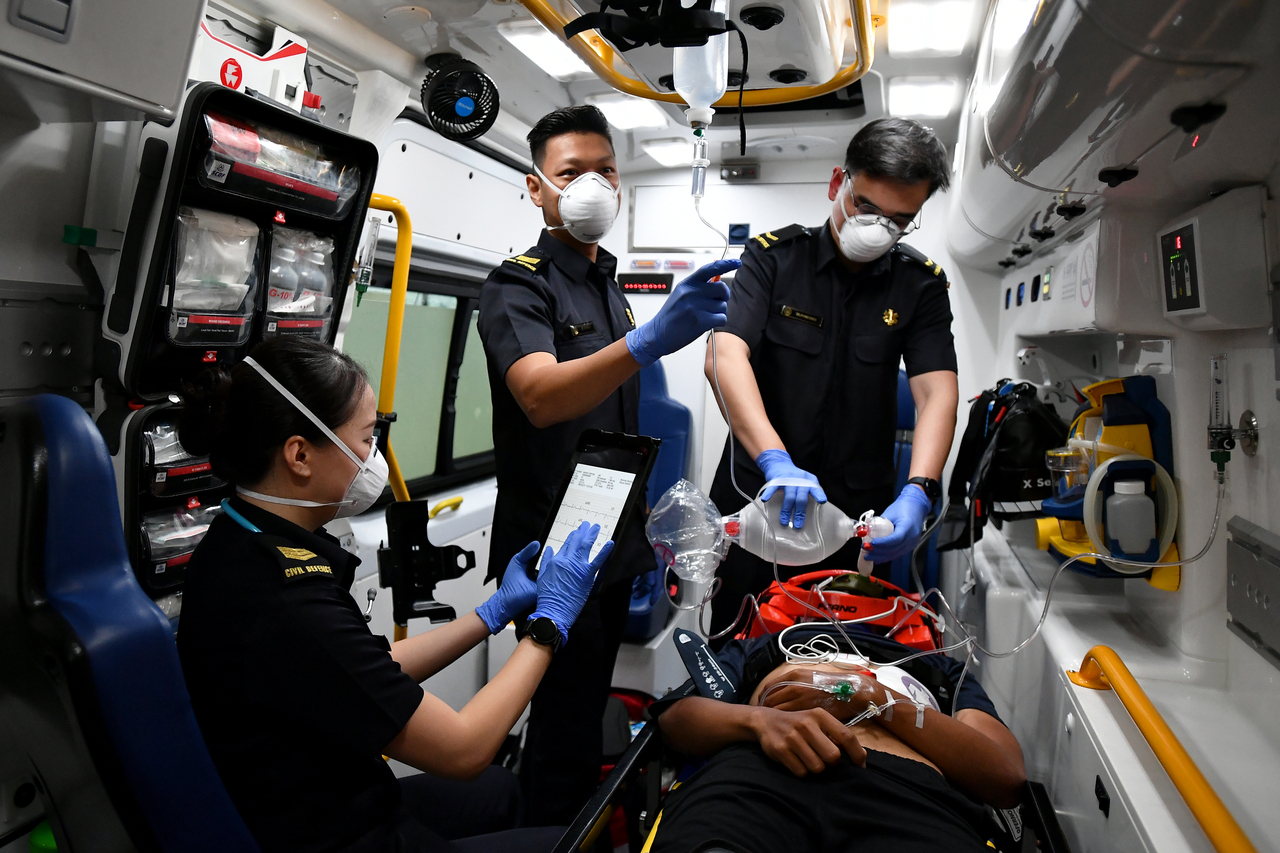
Pre-hospital emergency care systems provide a sequence of rapid responses before a patient gets to a hospital.
ST PHOTO: LIM YAOHUI
Follow topic:
SINGAPORE - Every minute counts and a programme to improve the standard of emergency care a person receives before reaching a hospital has been launched.
Pre-hospital emergency care (PEC) systems are critical as they provide a sequence of rapid responses during events, such as a stroke or cardiac arrest, before the patient arrives at the hospital.
This can make a big difference to saving lives and ensuring better patient outcomes, especially since many medical emergencies occur outside of the hospital, such as at home or the workplace.
A first in South-east Asia, the three-year programme was jointly launched on Saturday (May 21) by SingHealth and Temasek Foundation, in partnership with the Asian Association for Emergency Medical Services and Pan-Asian Resuscitation Outcomes Study network (Paros).
The initiative will train 250 participants from Indonesia, Malaysia, the Philippines, Thailand and Vietnam in skills crucial for the recognition, intervention and treatment of emergency cases before they reach the hospital, Temasek Foundation and SingHealth said in a joint statement.
The programme, which starts on Saturday (May 21) and takes five days, is held online and in person at Singapore General Hospital (SGH). Another three days of training will be held in each partner country.
These participants include national disaster management officials, healthcare officials and workers, ambulance personnel, emergency first responders and leaders of community organisations.
Around 30 of them will be given further training to qualify as master trainers. They will be able to develop expertise in enhancing PEC systems in their countries or institutions at a system level, pegged to international benchmarks, and be equipped to train other professionals and community partners.
Speaking at the launch at SGH on Saturday, Senior Minister of State for Health and Manpower Koh Poh Koon, the guest of honour, said: “Beyond training, the programme will promote collaboration and sharing of international best practices among the partner countries.
“It also provides a platform for partner countries to develop joint initiatives to reduce morbidity and mortality, for research collaboration, and share ideas to strengthen their respective PEC systems.
“Ultimately, these efforts will enhance the PEC research and Emergency Medical Services (EMS) treatment capability in our region.”
For victims of medical emergencies to have the highest chance of survival, there needs to be an optimised system of care. This system is made up of the community, first responders, dispatchers, ambulance services and emergency departments working together to provide critical immediate response.
This is known as a chain of survival, and a strong PEC system is part of this chain.
In Singapore, the Ministry of Health (MOH) has been working to strengthen this chain and track improvements in overall survivor outcomes.
According to data from the unit for pre-hospital emergency care in MOH, more than 3,400 people suffered cardiac arrest outside the hospital - also known as out-of-hospital cardiac arrests (OHCA) - in 2020.
In 2011, there were about 1,300 cases.
OHCA cases in Singapore more than doubled in the last decade - from 27 cases per 100,000 people in 2011 to 60 cases every 100,00 people in 2020.
The rate where bystanders administered cardiopulmonary resuscitation to a cardiac arrest victim also more than doubled from 22 per cent to 56 per cent, while the rate where bystanders used an automated external defibrillator improved from 2 per cent to 9 per cent in the same time period.
However, these two rates saw a slight drop in 2020 during the pandemic compared with pre-pandemic year 2019.
Professor Marcus Ong, who is chairman of Paros and a senior consultant at the emergency medicine department in SGH, said: “This drop in rates could be because more cardiac arrests happened at home in the last two years.
“The rate at which bystanders respond to home incidents tend to be lower compared with if these incidents happen in the public space and not everyone in the household is aware of what to do. But more research needs to be done.”
“It could also be because people are concerned about catching Covid-19 if they perform CPR. We encourage people to perform hands-only CPR, and for those who are worried about getting infected with Covid-19, the chance of that happening is actually low,” Prof Ong added
Data also showed that 74 per cent of the cardiac arrest survivors had full brain recovery and could return to work or resume their normal life.
"Beyond training, the programme will promote collaboration and sharing of international best practices among the partner countries," Dr Koh said.
It also provides a platform for partner countries to develop joint initiatives to reduce morbidity and mortality, collaborate in research, and share ideas to strengthen their PEC systems.
The programme will also facilitate the development of research infrastructure for emergency medical services (EMS), and play a part in strengthening EMS treatment capabilities in the region, the statement said.
Professor Kenneth Kwek, deputy group chief executive (innovation and informatics) at SingHealth, said: "It takes a system to save a life, and strong pre-hospital emergency care systems are vital to any country's crisis response to medical emergencies."
The event also witnessed the launch of the Hero with a Heart: Push a Button, Save a Life! initiative, which emphasises the importance of community first responders.
Prof Ong said: “In Singapore, this can be as simple as downloading the myResponder app and participating as a community first responder, or calling 995 and following instructions from the SCDF dispatcher to resuscitate a cardiac arrest victim.
“The critical success of pre-hospital emergency care lies not only in the hands of ambulance personnel or healthcare professionals but also the public that rises to the occasion in each life-saving act.”
The myResponder app from the Singapore Civil Defence Force alerts users to nearby fires and medical cases.

