Coronavirus pandemic
My body was a wreck, says Covid-19 patient
Couple who contracted disease recount ordeal, thank healthcare workers who cared for them
Sign up now: Get ST's newsletters delivered to your inbox

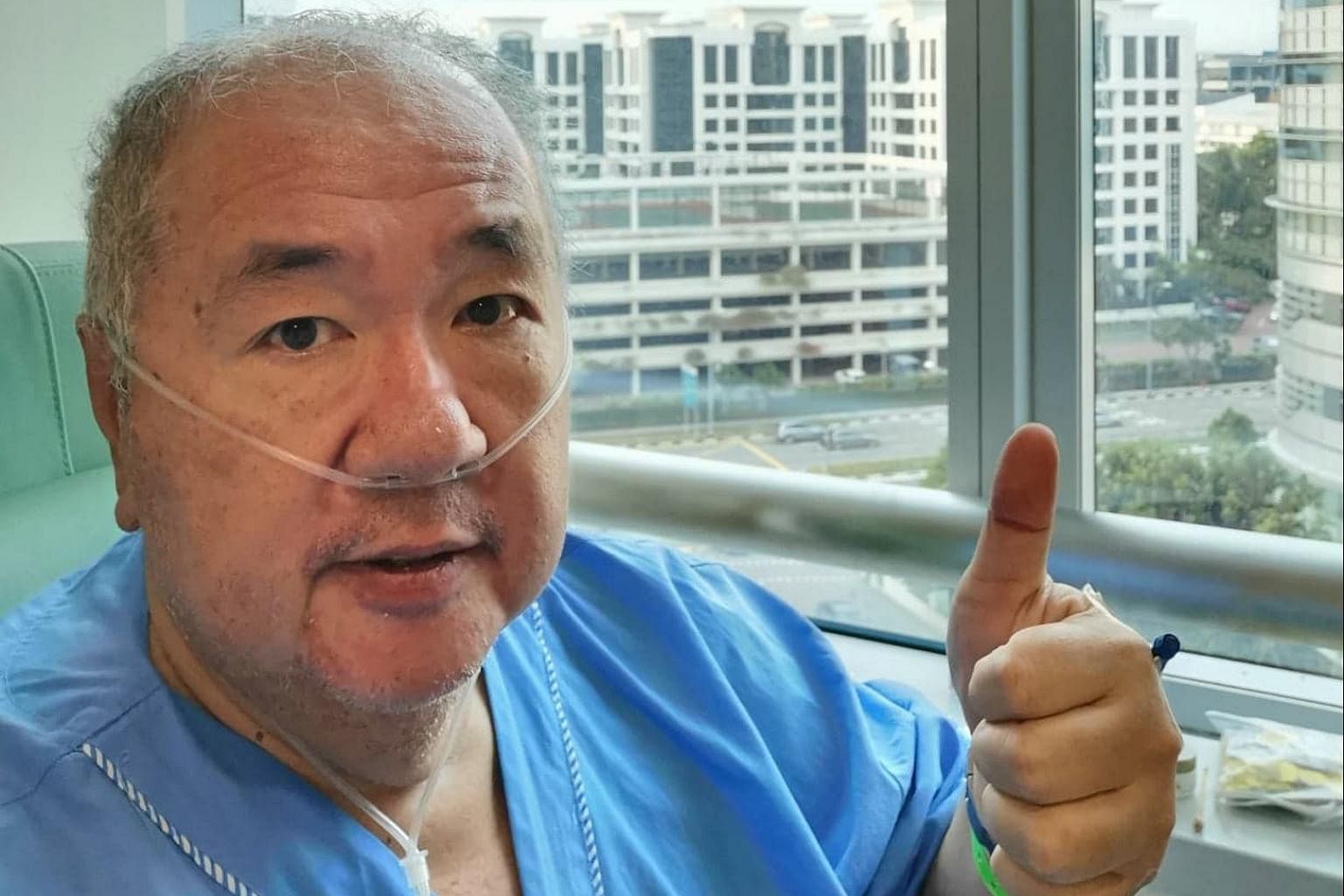
Mr Andrew Phay and his wife Anna Yeo tested positive for Covid-19 in March after a 25-day trip to the United States and Mexico.
ST PHOTO: KEVIN LIM
On his 15th day at Changi General Hospital (CGH) battling the coronavirus, Mr Andrew Phay woke up to news that he had low oxygen levels in his blood.
All he could do was pray for a miracle.
X-ray checks showed his lungs were in bad shape and he needed breathing tubes to direct oxygen into them.
Mr Phay, 56, had tested positive for Covid-19 on March 17, after a 25-day trip to the United States and Mexico. His wife Anna Yeo, 57, and their two friends who were on that trip also contracted the virus.
"The fear of the unknown hit hard," said the retiree of the possibility that he would have to be moved to the intensive care unit.
"I prayed, I cried and despaired."
Doctors resorted to using hydroxychloroquine*, typically used to treat malaria, to improve his lung function after his body responded poorly to an earlier related drug.
Mr Phay, Singapore's case 277, was earlier given chloroquine, also used to treat malaria, for three days. But those were the "worst three days" of his hospital stay, he said, as his body "reacted very badly" to it.
"Every breath I took made me nauseated. I couldn't sit, couldn't sleep, couldn't stand," he said.
"I was taken off the medication but my body was a wreck."
His body accepted the second drug better than the first and, gradually, he felt less breathless.
Mr Phay has since recovered and was discharged on April 8. He said: "I believe I was given a second chance in life."
The former Asia-Pacific vice-president of an American information technology firm believes he and his travel companions had contracted the virus on their return to Singapore.
They had travelled overseas to attend his niece's wedding in Cancun, Mexico, and had taken a few connecting flights before arriving home on March 15.
"We were possibly infected during the time when we left the family," said Mr Phay, adding that the relatives and friends they had met there did not contract the disease.
On March 16, a day after arriving home in Singapore, he had throat irritation.
He woke up with a fever the next day and went to a general practitioner, where he was urged to go to the nearest hospital, CGH.
There, he had an X-ray and swab tests done and was told to go home and wait. That afternoon, the hospital staff rang to tell him he was down with Covid-19.
Mr Phay's first thoughts were "feelings of guilt and concern" for those he had come in contact with. He had met his parents and two relatives the day before.
His family, including his 28-year-old son and elderly parents, were issued quarantine orders. His wife and travel companions later tested positive for Covid-19 and were warded at the National Centre for Infectious Diseases (NCID).
Madam Yeo, who is case 422, had throat irritation on March 19. She developed a fever the next day and was taken to the NCID for X-ray checks and swab tests.
On March 21, her test results returned positive. "The first thought was whether our son was infected by us," said the housewife of their only child.
Thankfully, none of their family members was infected. During that period, relatives and friends spurred them on, while the neighbours helped by cooking meals for their son.
During his first few days at CGH, Mr Phay experienced mild symptoms. His fever was intermittent and his throat felt better on the third day.
On March 25, doctors started him on chloroquine.
"I couldn't rest at all. I tried throwing up but had only dry heaves," he said.
On March 31, the doctors used another drug, hydroxychloroquine*, after X-ray checks found his lungs to be in bad shape.
Mr Phay said: "I was told that if my lungs got worse, I might need to be on ventilator support."
Fortunately, his lungs recovered and the oxygen support was later removed.
Mr Phay was well enough on April 5 to be moved next door to St Andrew's Community Hospital, a step-down facility. He was discharged three days later.
"The wait for two negative swabs was excruciating," said Mr Phay, who was relieved when a doctor told him he could go home.
He said the healing of the lungs is a long process. "It gets better with each day but I still get a bit breathless when I try to exercise."
His wife spent 20 days at the NCID before she was moved to Concord International Hospital on April 9. She was discharged on April 14.
To celebrate their reunion, the couple and their son had an Italian meal at their condominium in Flora Drive the next day.
"I felt happy and blessed that we were able to have a meal together," said Madam Yeo, stressing that time spent with the family cannot be taken for granted.
The Phays are thankful to the front-line healthcare workers for risking their lives to care for them.
Mr Phay said: "It takes a lot from them to go to work in such uncertain times and put on a brave front for their patients.
"I am sure they experience more intensely the same emotions that we have, including the anxiety and fear of being exposed to the virus and whether they would infect their loved ones."
*Note: Malaria drugs chloroquine and hydroxychloroquine, which had shown some early promise against Covid-19, are no longer commonly used in Singapore, as some studies had found that, in addition to not working, they were also associated with side effects.


