MOH releases two new daily charts to better reflect Covid-19 situation in S'pore
Sign up now: Get ST's newsletters delivered to your inbox

The chart will provide a clearer representation of the situation in the hospitals, especially the ICUs.
PHOTO: ST FILE
DeeperDive is a beta AI feature. Refer to full articles for the facts.
SINGAPORE - Two new charts have been added to the daily Covid-19 updates that the Ministry of Health (MOH) issues every night.
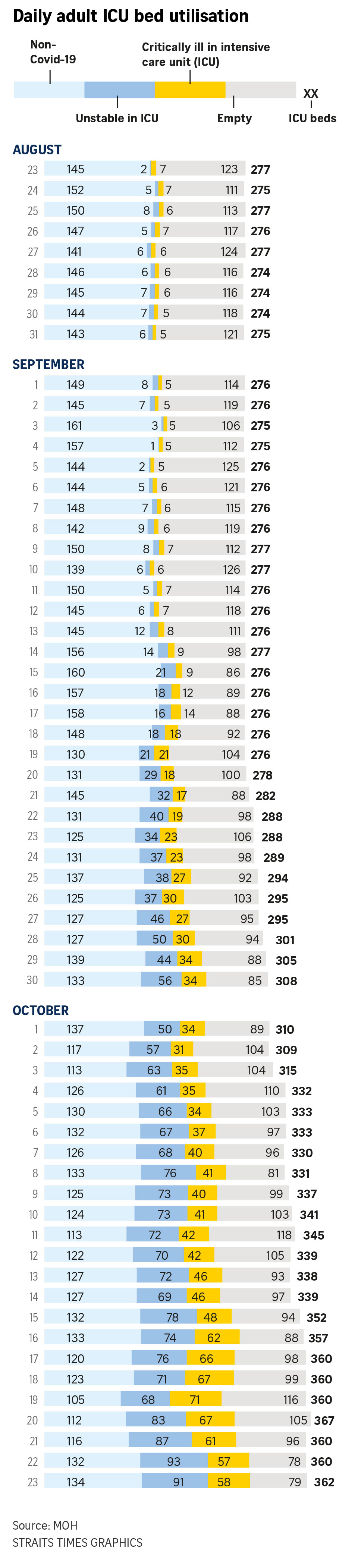
They are a chart of Singapore's daily adult intensive care unit (ICU) bed utilisation, and another showing the ratio of community cases in the past week compared with the week before.
The ICU chart details, over time, the number of empty ICU beds, patients critically ill in the ICU (such as those requiring ventilators), those unstable in the ICU (who require monitoring or are on oxygen support) and non-Covid-19 ICU cases.
The chart will provide a clearer representation of the situation in the hospitals, especially the ICUs, said Professor Teo Yik Ying, dean of the Saw Swee Hock School of Public Health at the National University of Singapore.
Looking at the bigger picture of ICU utilisation as a whole instead of just focusing on those who are critically ill and in the ICU also provides a better reflection of the situation in the hospitals as doctors are working equally hard to provide a high quality of care even for those who are just being monitored in the ICU, he added.
There is also a lag time in ICU utilisation and infection numbers as a person who is infected today may only progress to a critical stage requiring ICU care in seven to 10 days, Prof Teo noted.
"Given that every patient in the ICU has a real risk of experiencing severe symptoms that may result in death, we want to prevent as many cases in the ICU as possible... However, if we have already utilised in excess of two-thirds of the ICU beds, it is already pointing to a trajectory that our healthcare system is under pressure."
Health Minister Ong Ye Kung said on Oct 20 that the surge in Covid-19 cases here has placed significant pressure and strain on public hospitals, with 89 per cent of the 1,650 isolation beds and 67 per cent of the ICU beds occupied.
There are currently about 200 ICU beds for Covid-19 patients, who stay an average 15 days in the ICU. But the longest stay can be up to a month, Mr Ong said.
The chart also shows explicitly who is in the ICU with Covid-19 and who is desperately ill in the ICU with Covid-19, said Associate Professor Alex Cook, vice-dean of research at the NUS Saw Swee Hock School of Public Health.
He noted that even though the utilisation has gone up, temporary ICU facilities have been created to ensure that those who need it can access it, as seen from the overall increase in ICU capacity.
"I understand that we can continue to create more temporary ICU beds until about 1,000, but as the numbers go up, the quality of care will start to be sacrificed," Prof Cook added.
On the other new graph, looking at the ratio of two sets of case numbers is better than purely looking at daily case numbers as daily numbers will fluctuate, said the two experts.
"If you look at the daily case numbers, there's a weekly pattern. It's especially obvious on Tuesdays, which will see a higher case number as the results come in for people who went to a clinic on a Monday," Prof Cook said.
"The number of people going to a clinic on Monday is probably higher because clinics are usually shut over the weekend, so people delay the visit to a doctor till Monday," Prof Cook added.
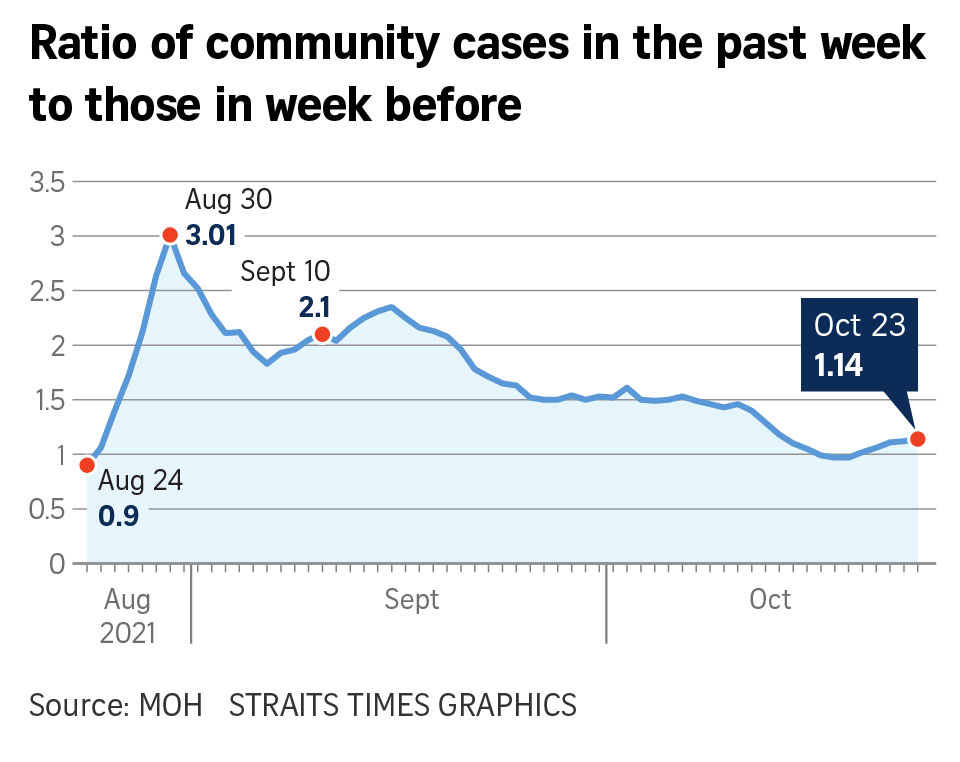
This is a similar trend with influenza, and can be overcome by taking the ratio of today to one week ago, Prof Cook noted.
A consistent series of days or even weeks where the ratios fall below one will reflect the epidemic to be under control, and that there are few new cases being reported each week, Prof Teo said.
"However, this number does not necessarily reflect the strain on the healthcare system. If we have fewer cases being reported each week but many of these cases are unvaccinated people who are old or with underlying medical conditions, then the strain on the healthcare system will remain or even worsen," Prof Teo added.
"Right now, if we truly want the strain on the healthcare system to be alleviated, we need to get the remaining unvaccinated people to be vaccinated, as they are disproportionately taxing the healthcare system."