Low-oxygen environment can worsen TB damage to lungs
Sign up now: Get ST's newsletters delivered to your inbox
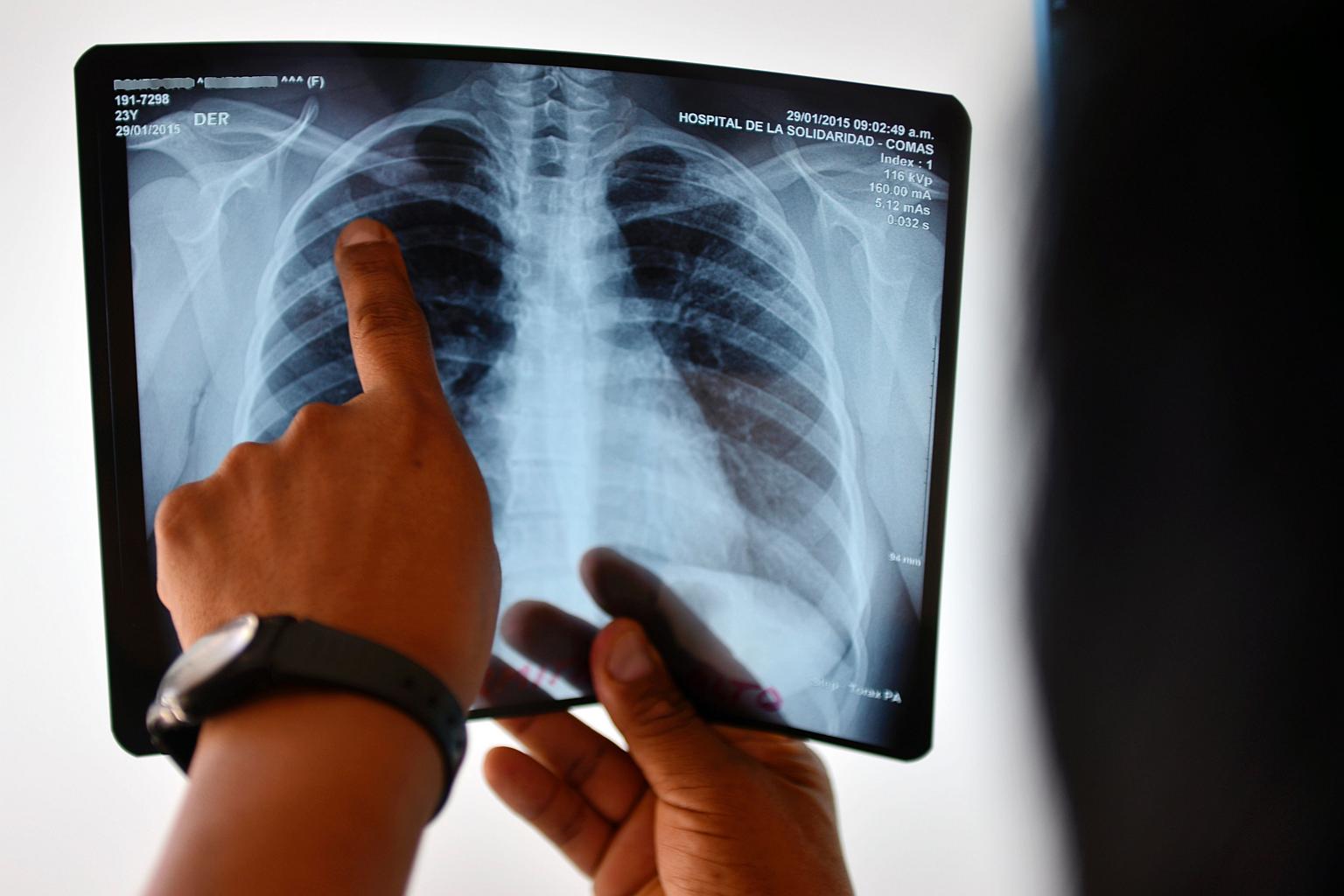
Now, scientists have learnt that a low-oxygen environment - which is often found in the lungs of TB patients - can make this damage even worse.
PHOTO: AFP
When a person contracts tuberculosis, his body dispatches white blood cells to fight off the disease.
But, these cells can also cause collateral damage to the lungs.
Now, scientists have learnt that a low-oxygen environment - which is often found in the lungs of TB patients - can make this damage even worse.
"It's a vicious circle," said Dr Catherine Ong, who was part of the team studying the phenomenon. Their findings were published in international journal Scientific Reports earlier this year.
Dr Ong said these white blood cells, known as neutrophils, secrete enzymes that destroy both TB bacteria and lung tissue. This includes lung collagen, which helps the organ keep its structure and elasticity.
When the lung is damaged, oxygen levels can drop further, and this triggers the production of more destructive enzymes.
Tuberculosis is endemic in Singapore, with 1,536 new cases reported among Singapore residents last year. Latent TB infections, where people unknowingly carry an inactive form of the disease in their bodies, are not uncommon.
Dr Ong, a consultant with the National University Hospital's infectious diseases division, added that if left untreated, the consequences of active TB infections can be dire.
"For example, a patient could have holes in their lung or even have the whole lung destroyed as a result of the disease," she said.
For the study, Dr Ong and her team put neutrophils in a low-oxygen laboratory environment and tracked their behaviour.
They found that these neutrophils not only produced more destructive enzymes, but also tended to live longer.
Now that scientists know what triggers the destruction of lung tissue, they can start looking at ways to stop this from happening, Dr Ong said.
One solution could be as simple as providing patients with extra oxygen, which is already being used to treat other medical conditions. Another could be to find a drug that would help to limit the amount of damage done.
"We want to find out if there are biological pathways we can use to target this reaction, and allow the enzyme to perform its function without the damage," Dr Ong said.
She added that the findings could be useful for other diseases that also cause low oxygen levels in the lungs, such as chronic obstructive pulmonary disease and lung fibrosis.


