Women welcome MOH move to screen for family cancer history, have insurance cover preventive surgery
Sign up now: Get ST's newsletters delivered to your inbox

Breast cancer is the most common cancer among women in Singapore, with more than 2,000 women diagnosed and more than 400 dying from the disease a year.
PHOTO ILLUSTRATION: UNSPLASH
- Singapore will subsidise genetic testing for hereditary breast and ovarian cancer (HBOC) from December, addressing a high mutation rate (1 in 150 individuals).
- MediShield Life and MediSave will cover risk-reducing surgeries for eligible women with HBOC from late 2026, enhancing financial support for preventive measures.
- Women like Ann and Alice highlight the need for affordable preventive care, as current insurance often denies coverage for risk-reducing surgeries, causing financial and emotional strain.
AI generated
SINGAPORE - Business executive Ann, 51, had been diagnosed with Stage 1 breast cancer in her right breast.
But when she opted for a double mastectomy in 2021 at age 47 and had both breasts removed at the same time, her insurers refused to cover the preventive surgery to remove and reconstruct her non-cancerous left breast.
It paid for only one.
Meanwhile, Alice, at 61, found out she carried a gene mutation associated with hereditary breast and ovarian cancer after her sister in the US was diagnosed with breast cancer.
Although she was able to take preventive steps that included surgery later, she felt that she might have made different life choices if she had known earlier.
Both women, who declined to give their full names for privacy reasons, welcomed the Health Ministry’s recent move to not only subsidise genetic testing for hereditary breast and ovarian cancer (HBOC), but also allow MediShield Life and MediSave to be used to pay for risk-reducing surgery.
They hope that women from now on will not only know their risk early, but also be spared the back and forth with insurance companies to have preventive treatments covered, as Ann experienced.
Speaking at the debate in Parliament on his ministry’s budget on March 5, Health Minister Ong Ye Kung announced that subsidised genetic testing for HBOC would start in December, and MediShield Life and MediSave would cover risk-reducing surgery for eligible women from late 2026.
Breast cancer is the most common cancer among women in Singapore, with more than 2,000 women diagnosed and more than 400 dying from the disease a year.
A 2024 study of 572 Asian families in Singapore and Malaysia with the gene mutations estimated that one in 150 individuals carries a mutation such as BRCA1 or 2, which are associated with HBOC, substantially increasing a woman’s lifetime risk of developing breast and ovarian cancer.
The study, conducted by researchers from institutions such as NTU’s Lee Kong Chian School of Medicine, the National Cancer Centre Singapore, A*STAR, Cancer Research Malaysia and the University of Malaya, provides an important framework for estimating cancer risks in Asian carriers to allow a more tailored approach to managing the disease in Singapore.
Currently, subsidies are available to support family planning, specifically for individuals with a family history of high cholesterol or severe genetic conditions. There are about 20,000 people in Singapore with hereditary high cholesterol, which can increase their risk of getting a heart attack at a younger age by up to 20 times.
Up to 70 per cent of the costs of specific, approved genetic tests will be subsidised for eligible Singapore citizens and permanent residents, who can also tap their MediSave to offset the remainder.
For HBOC testing, it is also offered to family members of women with breast or ovarian cancer who carry the faulty BRCA gene.
While regular mammograms are effective for detecting breast cancer early in women aged 50 and above, there is no similar recommendation for younger age groups. As a result, cancer may be missed in younger women who have HBOC gene mutations.
These women face a lifetime risk of up to about 60 per cent for breast cancer and up to about 50 per cent for ovarian cancer, compared with up to 13 per cent and up to 2 per cent, respectively, in the general female population.
In his March 5 speech, Mr Ong told the House that if these women test positive, their immediate family members will also be assessed.
A woman identified to have hereditary mutations in HBOC-associated genes will be recommended for more frequent mammograms or other risk-reducing measures such as surgery.
Such surgery can be paid for or defrayed through MediShield Life and MediSave from later in 2026, which was an option that Ann never had.
Integrated healthcare plan did not agree to pay for her double mastectomy
When Ann was in her mid-30s, she felt lumps in her breasts, and a mammogram at her doctor’s office found several of them.
“I did a biopsy on one of the lumps, and it was found to be benign,” she told The Straits Times. With her doctor, she decided to keep monitoring the growths.
For over a decade, Ann maintained a rigorous schedule of scans and mammograms, sometimes every three months, other times every six months. This prolonged period of surveillance was “expensive, time-consuming and emotionally tiring”.
During that time, her family faced significant challenges. Both of her sisters and her mother were diagnosed with breast cancer. While her sisters survived the illness, her mother suffered a relapse and died in November 2025.
Ann said she became the last woman in her immediate family to be diagnosed with breast cancer.
Her breast surgeon categorised her as high-risk due to her family history and the presence of multiple lumps in both breasts. Additionally, one of the lumps had changed shape during routine scans, raising further concerns.
Ann underwent a biopsy for the lump and also genetic testing, and though she tested negative for the BRCA mutation, her oncologist said a negative result did not rule out the possibility of developing breast cancer, given the strong link to family history.
The biopsy confirmed that Ann had Stage 1 breast cancer in her right breast.
“Since I was high-risk given my history of having multiple lumps in both breasts, we both agreed that it would be safer for me to do a double mastectomy, despite my left breast not being affected,” she said.
Ann even consulted a psychiatrist before the surgery to ensure her decision was a rational one, yet her insurance company declined to pay for the double mastectomy, agreeing only to one – the mastectomy and reconstruction of the cancerous breast.
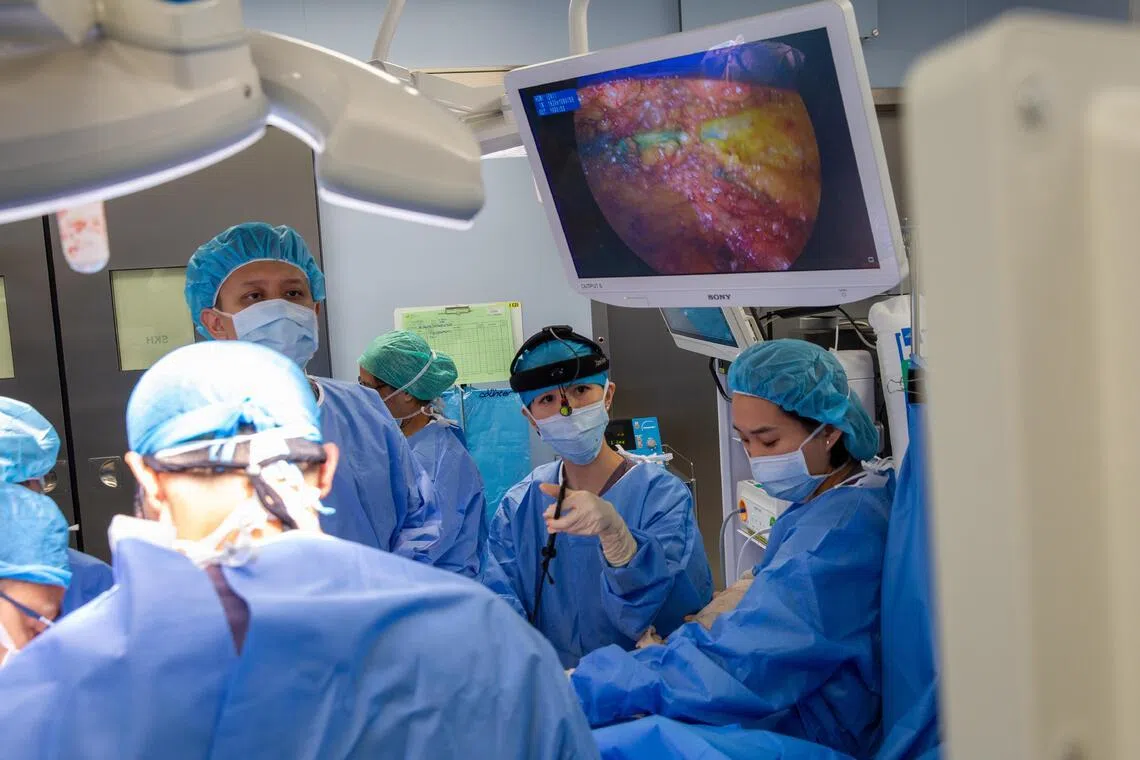
Currently, insurers will pay for surgery to remove a cancerous breast, but not preventative surgery. This will soon change when MediShield Life and MediSave are available for such procedures for HBOC.
PHOTO: SENGKANG GENERAL HOSPITAL
“It stated that removal of the (healthy) breast was ‘an elective decision for cosmetic reasons’. That was insensitive and cruel, and also completely disregarded the medical opinion of my doctor,” Ann said.
After months of failed appeals, she was mentally and emotionally drained.
“No woman takes a mastectomy decision lightly. To be made to justify my painful decision is making me relive everything over and over again. I just wanted to move on and get on with my life,” she said.
Ann told ST she was glad to see that the health system now officially recognises preventive surgery as medically necessary.
Subsidised genetic testing cuts costs, helps manage cancer early
As for Alice, it was only after her sister in the US was diagnosed first with breast cancer and two years later, with ovarian cancer, that she, now 73, and her immediate family consented to genetic screening in 2014. Alice is believed to have paid between $1,000 and $2,500 per test.
“I was already 61 when I found out I had the familial BRCA1 faulty gene, which meant that the chance of my getting breast and ovarian cancer is higher than others’. That was when it was mandated that I go for a six-monthly surveillance screening to catch any cancer signs,” she said.
She recalled vividly that she became anxious about breaking the news to her three daughters.
“I was worried as they could have inherited the faulty gene as well,” Alice added.
Following her news, her daughters got tested and are monitoring closely.
In December 2018, a lump was discovered in her right breast, and Alice had a double mastectomy carried out in February 2019.
“With the knowledge of my having the inherited gene, it definitely helped to direct my management of my cancer risk,” she said.
Doctors told ST that each child of a parent who carries a BRCA mutation has a 50 per cent chance of inheriting the mutation.
Alice also had her ovaries removed at a later stage to reduce her risk of ovarian cancer.
“With subsidised genetic screening for HBOC, it will definitely help younger women, especially those who are at high risk but who cannot afford the tests, make informed decisions when it comes to preventive surgery,” she said.



