BRANDED CONTENT
What oncologists want women in their 30s and 40s to know about triple-negative breast cancer
Learn more about this aggressive form which occurs at a younger age, its symptoms and the latest treatments

Triple-negative breast cancer (TNBC) is a more aggressive form of cancer that appears more frequently among younger women in their 30s and 40s. PHOTO: GETTY IMAGES
Breast cancer is the most common cancer among women in Singapore, occurring in nearly 30 per cent women in Singapore who are diagnosed with cancer. This year, it has overtaken lung cancer to become the most common cancer worldwide and leading cause of death among women, according to the World Health Organisation.
About 70 per cent of all breast cancers are hormone positive breast cancer, meaning that the cancer cells contain either oestrogen receptor or progesterone receptor or both. They are commonly diagnosed among women in their 60s.
There is another type known as triple-negative breast cancer (TNBC), a more aggressive form of cancer that appears more frequently among women in their 30s and 40s, says Dr Khoo Kei Siong, deputy medical director and senior consultant at Parkway Cancer Centre.
Other risk factors of breast cancer include:
- Race: African-American women are at greater risk
- Family history: A family history of breast cancer increases your risk of developing breast cancer
- Weight: Those who are obese have a higher risk of of developing breast cancer
- Pregnancy: Women who are pregnant for the first time after the age of 30
- Personal history: Women with cancer in one breast have a three- to four-fold increased risk of developing cancer in the other breast or in another part of the same breast
Among those diagnosed with TNBC, about 10 to 15 per cent carry the BReast CAncer 1 (BRCA 1) gene mutation, which increases the risk of developing breast cancer.
Doctors may also measure the levels of a protein (called PD-L1) on cancer cells and the immune cells around it after biopsy. PD-L1 is made by the cancer cells. When it binds to the PD-1 receptor on the immune cells, the immune cell loses the ability to recognise the bad nature of cancer cell and fail to attack it. Presence of PD-L1 may help in selecting the appropriate therapy for patients.
Here are three things you need to know about TNBC:
1. TNBC is a more aggressive form of breast cancer
"Aggressive means that the cancer has a higher growth rate and grows quicker. If a surgery was done, there is a higher chance of recurrence. Patients also have a shorter survival period," says Dr Khoo.
In general, five-year relative survival rate is reduced significantly with more advanced stages.
In comparison, hormone positive breast cancers can be kept under control and their recurrence rate reduced at all stages with hormone therapy. HER2, which is another type of aggressive breast cancer, can be managed with targeted drugs too.
TNBC cells do not have oestrogen and progesterone receptors (ER and PR), and also lack the human epidermal growth factor receptor 2 (HER2). The absence of these receptors means that, unlike their hormone-receptor positive and HER2 positive counterpart, it is more difficult to cure TNBC than other breast cancer subtypes as it lacks the targets (such as ER, PR and HER2). Hence, chemotherapy remains the mainstay of treatment.
Symptoms for TNBC are similar to other types of breast cancers. Common symptoms include a lump in the breast, swelling, breast or nipple pain or nipple discharge.
2. There are treatment options for TNBC
Women now being diagnosed with TNBC may have a better outlook than before.
Surgery is an important and essential part of the treatment as long as the cancer is confined to breast and the lymph nodes in the arm pit (from stage 0 up to some of the Stage 3). It involves removing the tumour from the breast and the lymph nodes from the armpit if they are affected. Stage 0 breast cancer refers to a non-invasive form of breast cancer.
Chemotherapy may be given first to shrink a large tumour before surgery or given after surgery to reduce the chances of cancer returning. Radiation might also be an option depending on the characteristic of the tumour.
"Once the cancer has spread beyond these areas, surgery to the primary tumour may not make a lot of difference in the long term," says Dr Khoo. "When a patient is discovered to have stage 4 breast cancer, what is known as metastatic cancer where it has spread beyond the breast, we are no longer in a hurry to do surgery." This is known as Stage 4 TNBC, where there is a higher tendency to spread to visceral organs such as the lungs, liver and kidneys.
"Even though TNBC is an aggressive disease, we now have better treatments that can offer patients a higher chance of getting the cancer under control."
Chemotherapy has been the conventional way to treat TNBC, especially in metastatic cases. TNBC tumours have responded to chemotherapy, although the cancer may return.
In the last 5-8 years, immunotherapy, in the form of PD-1 and PD-L1 inhibitors, has been found to be an effective treatment for many cancers including lung cancer, kidney cancer and melanoma. Amongst the different types of breast cancer, however, immunotherapy is only shown to be effective in TNBC, to date. Immunotherapy used in combination with chemotherapy may help improve response to treatment. The combination may help keep the cancer at bay for nearly 10 months; while with chemotherapy alone, regrowth may occur after six months.
Patients whose tumours express PD-L1 are eligible for this option. The higher the percentage of immune and cancer cells found to have PD-L1, the better the chance of response and a better outcome for the patient. Hence, if there are higher levels of PD-L1, it indicates to the doctor that the patient has a better chance of responding well to immunotherapy, and there is a better outcome for the patient.
In addition, patients who carries a mutated BRCA1 or BRCA2 gene also respond well to a class of drugs known as PARP inhibitors. In some selected cases, this means a longer chance of survival with a very good quality of life," says Dr Khoo. Other options to consider are antibody-drug conjugates (ADC).
With advancement in innovative therapies, many can live a relatively normal life and he has seen some patients able to return to work as well.
As treatment in TNBC progresses, Dr Khoo is "cautiously optimistic" that there may better treatment options for patients. However, he emphasises that finding the cancer at an early stage is still the best course of treatment.
3. The importance of healthy living and early detection
Although you cannot prevent cancer, some habits can help reduce the risk, including maintaining a healthy weight, staying physically active, eating fruits and vegetables and limiting alcohol consumption.
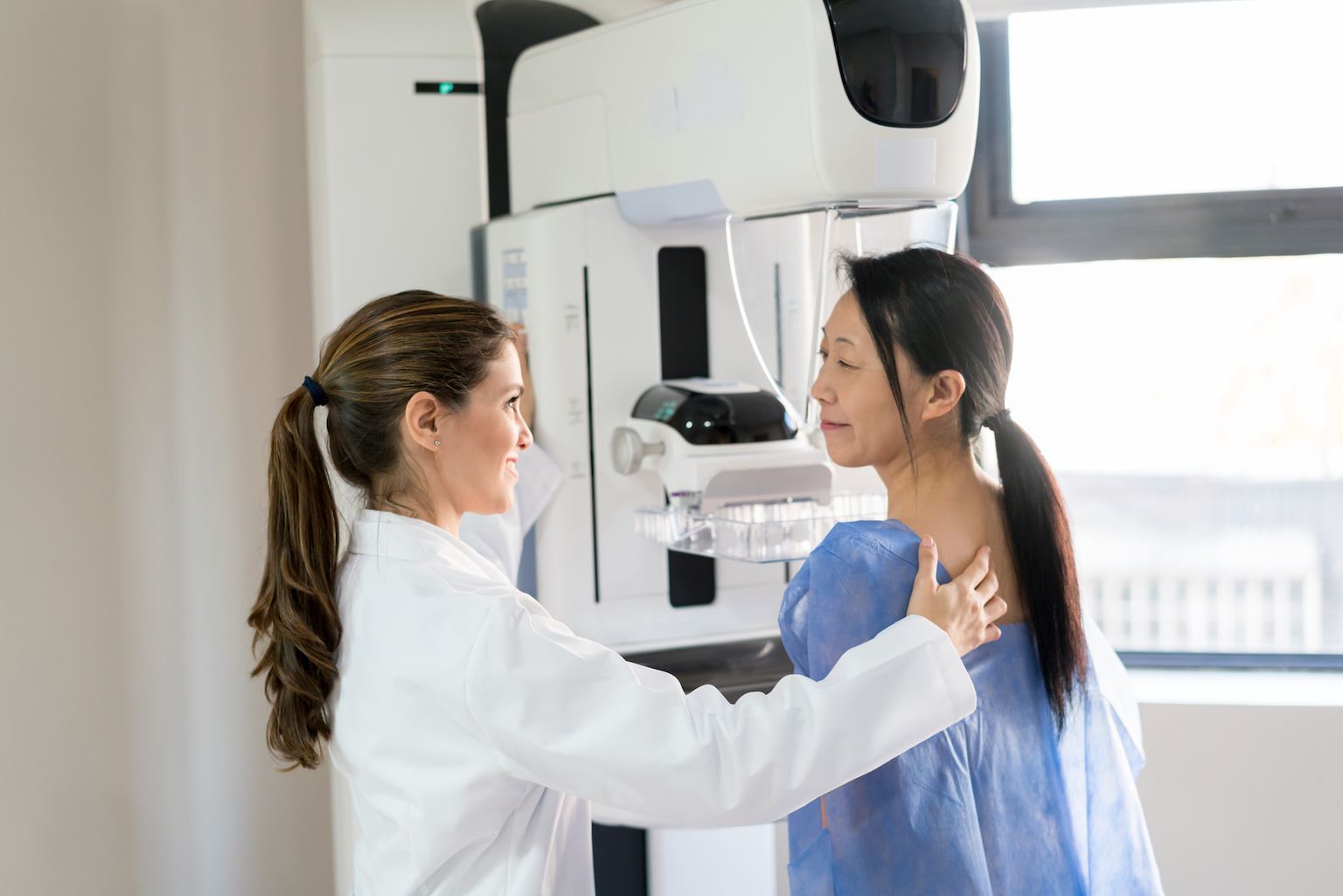
Many women with breast cancer also may not exhibit symptoms, even until the earliest part of stage 4. This is why Dr Khoo recommends women to go for regular mammograms every year when they reached 40, and every two years for women aged 50 and above, as per Health Promotion Board (HPB)'s recommendation. A mammogram is an x-ray that allows a qualified specialist to examine the breast tissue for any suspicious areas, and can detect tumours before they can be felt, so screening is key for early detection.
If you are below the age of 40, mammograms are not recommended for you. However, you are encouraged to perform breast self-exams at least once a month. Forty per cent of diagnosed breast cancers are detected by women who feel a lump, so establishing a regular breast self-exam is very important.
Early detection also helps discover the cancer earlier before it spread to other organs.
Dr Khoo advises: "No matter how effective the treatment is, the earlier you diagnose it, the higher the chance you can get rid of it. Be aware of the symptoms of breast cancer and seek treatment early. Go for screening and find it at stage 0."
Many women with breast cancer have no symptoms. This is why regular breast self-exam and breast cancer screening are important for early detection.
Speak to your healthcare provider to find out more.



