SINGAPORE - The Singapore Medical Council (SMC) has sent a circular to doctors reminding them of their role in helping keep healthcare costs down.
The reminder, it said, comes in the wake of recent scrutiny of healthcare insurance and unreasonable practices and fees. The SMC also alluded to media coverage of "hefty and questionable insurance claims".
It said that patients fully or largely covered by insurance may be less likely to contest the fees charged by the doctor. "However, patients' acquiescence to a doctor's fees does not absolve the doctor of the responsibility of charging reasonable fees," it said.
The SMC also reminded doctors not to subject a patient to unnecessary test or procedures just because of the fees the doctor can charge, as this may be a breach of his ethical obligations.
Similarly, doctors should not provide tests or treatments that are not clinically required, just because the patient wants them. It said: "Acting in a patient's best interests does not mean doing everything a patient wants."
The SMC acknowledged that there is no prohibition against hospitalising a patient for what is normally a day surgery. But it also sent out a warning: "Doctors must not recommend hospitalisation where there is no clinical justification to do so and for the primary purpose of charging higher fees. Such conduct may constitute overservicing and/or overcharging."
It said that even in cases where a doctor does not set the fees, so long as he has a material financial interest "he must satisfy himself that the fees abide by SMC's ethical standards".
The subject of doctors and patients, especially those who are fully covered by insurance, submitting large and questionable claims was raised in Parliament earlier this month.
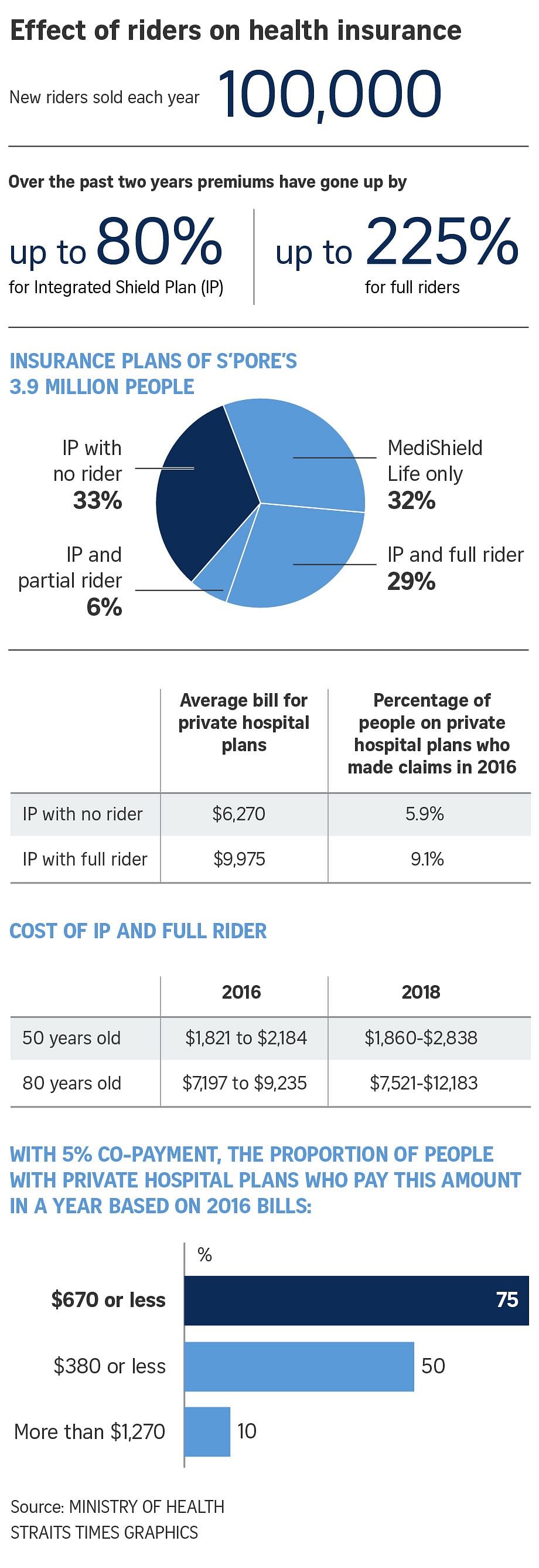
It was because of such claims that the Ministry of Health (MOH) will no longer allow full riders to be sold. All riders sold since March 8 have to include at least a 5 per cent co-payment by the patient.
Discussing the issue, Senior Minister of State for Health Chee Hong Tat had told Parliament: "Some of the examples of overconsumption and overservicing are - to put it plainly - disturbing."
He cited one case where a patient fully covered by his health insurance, "made claims for 12 nose scopes in a year, without clear medical need".
There were also cases where a patient was admitted for one problem, but was then seen by a host of other, unrelated specialists for scans and tests, chalking up bills "up to $25,000 for a hospital stay that was less than 24 hours!"
In yet another example, Mr Chee said one woman had run up a bill of more than $70,000 to remove a small breast lump. The procedure generally costs $5,000 in the private sector.
These were among the many cases that the six insurers providing coverage for Integrated Shield Plans (IPs) that incorporate MediShield Life, had submitted to the MOH.
When asked if the SMC plans to follow up on any of these examples, its spokesman said: "The SMC investigates complaints of alleged overservicing and overcharging by doctors. It can take disciplinary actions against errant doctors who do not meet the ethical code and ethical guidelines requirements, and has done so before."