Singapore began preparing early in 2020 for surge in Covid-19 cases in ICU
Sign up now: Get ST's newsletters delivered to your inbox
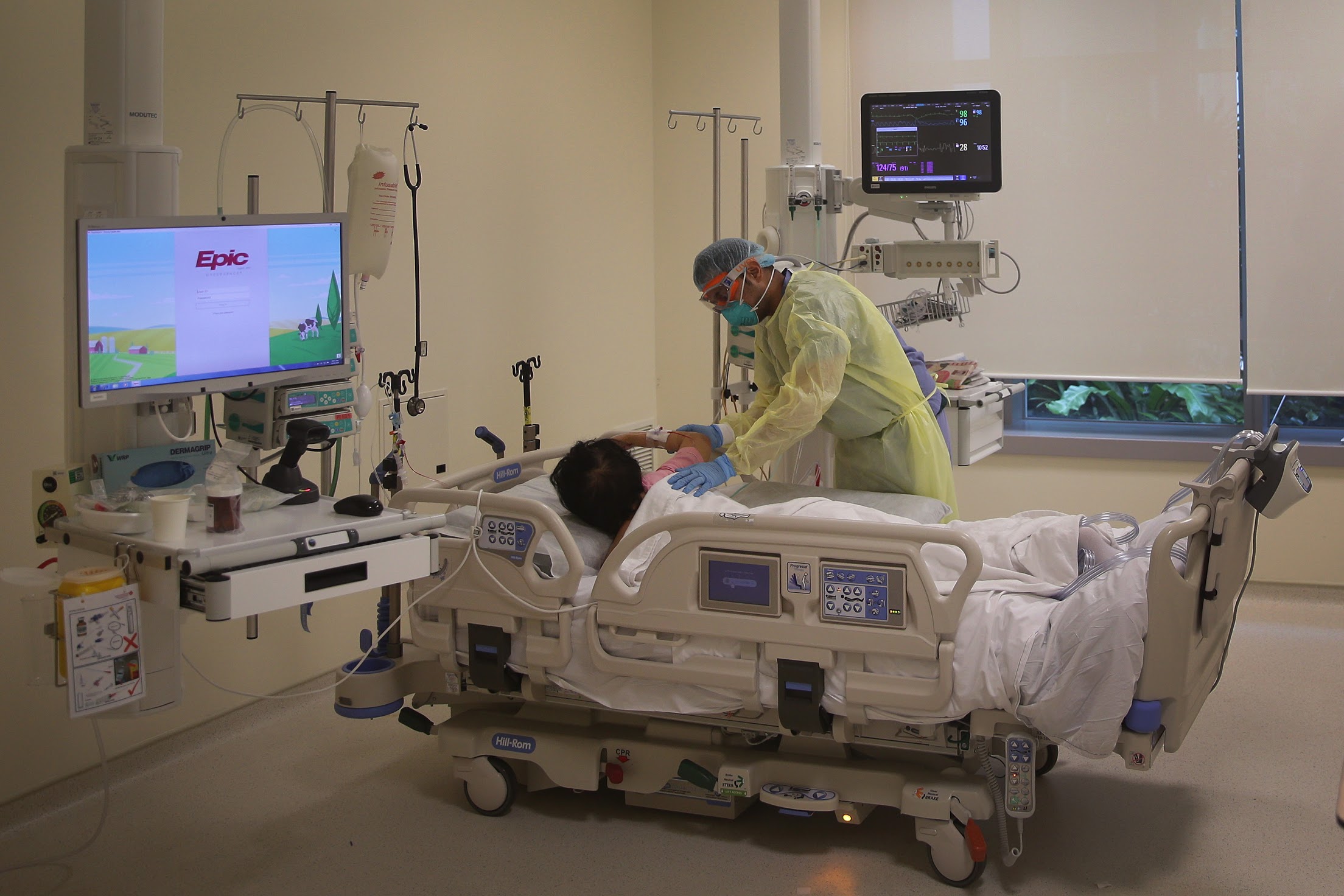
Turning ward beds into ICU beds takes time and effort.
PHOTO: ST FILE
SINGAPORE - Public hospitals in Singapore began preparing for a surge in seriously ill Covid-19 patients requiring intensive care early in 2020, about the time when the first Covid-19 patient was identified here.
Professor Philip Choo, group chief executive officer of the National Healthcare Group, told The Sunday Times: "In anticipation of Covid-19 becoming a pandemic, intensive care unit (ICU) bed planning at the national level had begun as early as January 2020.
"The National ICU Committee prepares and organises ICU care, which ranges from facilities to manpower, equipment and drugs."
The National Centre for Infectious Diseases (NCID), which has 38 ICU beds, recently turned 16 of its isolation ward beds into ICU beds. More can be added if needed.
Its isolation wards, with about 500 beds, were built to deal with infectious diseases, so all have negative pressure where air from the rooms is sucked out and cleaned by high-efficiency particulate air filters, and not allowed to flow into the corridor outside. This is needed for Covid-19 patients.
Turning ward beds into ICU beds takes time and effort. There are two parts to ramping up capacity.
One is the hardware needed for critically ill patients, such as ventilators to help them breathe, and machines to monitor a range of functions - all must go through biomedical engineering tests to ensure they are working properly.
The other is the need for trained and experienced doctors and nurses, as quick reactions and split-second decisions can mean the difference between life and death for a patient. And training is not something that can happen in days.
In February 2020, Tan Tock Seng Hospital (TTSH) identified and trained 500 experienced nurses to prepare them in case there was a need for more ICU nurses.
Over five days, they were taught not just how to care for someone who is critically ill and to use the many equipment needed in ICU, but also how to protect themselves when caring for someone with an infectious disease.
This includes donning full personal protective equipment (PPE) in just over a minute before going into the patient's room.
This was followed by four weeks working in the ICU to gain experience, before going back to their normal work.
Before being deployed to the ICU, they undergo a further seven-to-10-day refresher in an ICU where they work with highly experienced staff.
Prof Choo said: "Business-as-usual wards will be closed to shift these trained manpower to the outbreak ICU wards."
This is why the Government asked for electives, or non-urgent treatments, to be postponed several times, to free up staff so they can be trained to care for seriously ill Covid-19 patients.
Dr Hoi Shu Yin, TTSH's chief nurse, who has a staff of 3,500 nurses, said about 100 had to be deployed for the additional ICU beds, since they need to work round the clock with three nurses caring for four patients at any one time.
She said ramping up this year was more difficult than last year: "It's harder to prioritise for electives. Patients who could have their electives deferred last year cannot be deferred this year."
Dr Hoi said many who had their treatment - usually surgery - deferred "might come in more sick and so may stay longer". This adds stress to the general wards.
She also needed to move out some of the more capable and experienced nurses to the ICU, as they would be more able to deal with the very sick. Yet, she has to ensure there is sufficient nursing leadership in the wards and clinics to maintain high standards of care.
Appealing to seniors to get vaccinated to reduce the strain on limited hospital resources, Prof Choo said: "Unvaccinated elderly represent 1 to 2 per cent of our population, but account for two-thirds of our ICU beds."
Every additional 3,000 seniors getting vaccinated could translate to 300 ICU-bed days saved or more, he said. "Elderly patients with Covid-19 do not just suffer from respiratory illness. They may decondition after an acute bout of illness. Some may require a long period of rehabilitation."
This means they need to stay in hospital or step-down care facilities for longer, depriving other patients of a bed.
But with Singapore's forward planning, Prof Choo said: "We have not reached the point of rationing ICU beds."



