Risk of monkeypox spreading in S'pore is low, say experts
Human-to-human transmission risk low, and likelihood of outbreak is remote: Specialists
Sign up now: Get ST's newsletters delivered to your inbox
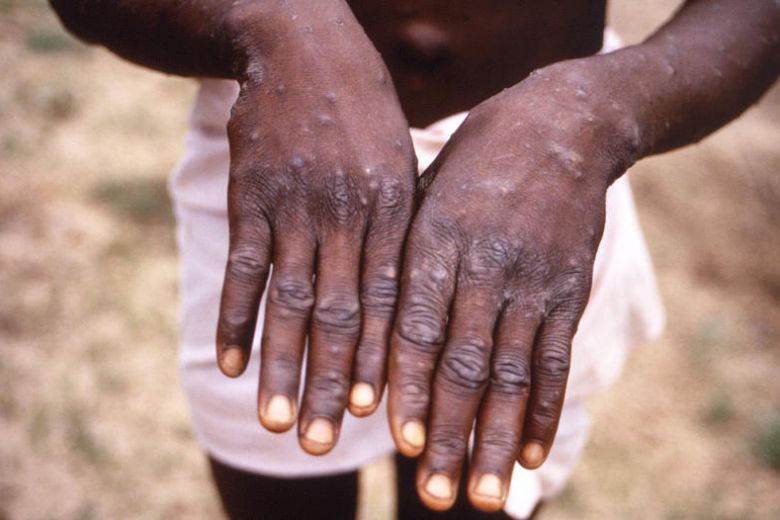
The Ministry of Health has confirmed one imported case of monkeypox infection in Singapore, involving a Nigerian national who arrived last month for a workshop.
PHOTO: CDC/BRIAN W.J. MAHY
Singaporeans need not worry too much about monkeypox spreading among the population here, as the risk of human-to-human transmission is low, say infectious disease specialists.
"I'm not worried about it," said Dr Leong Hoe Nam, an infectious disease specialist at Mount Elizabeth Novena Hospital.
"Monkeypox has been in other countries like the United Kingdom, and there were no local transmissions subsequently. It didn't happen there, and the chance of it happening in Singapore is low."
On Thursday, the Ministry of Health (MOH) confirmed one imported case of monkeypox - the first case reported here - involving a Nigerian national who arrived in Singapore on April 28. The 38-year-old man is in an isolation ward at the National Centre for Infectious Diseases and is in stable condition, MOH said.
Meanwhile, 22 of the 23 people identified as close contacts of the man are also under quarantine as a precautionary measure. The remaining contact, who left Singapore before the patient was diagnosed, has reported to MOH that he is well and has no symptoms. They came into contact with the man at Hotel 81 Orchid, where he stayed from April 28 to May 7, and at the Samsung Hub, where he attended a conference on April 29 and 30.
Employees at the hotel declined to comment when approached by The Straits Times. A response from the hotel's management was not available by press time.
Singapore is the fourth country outside the African continent - and the first in Asia - to report a monkeypox case, according to the United States' Centres for Disease Control and Prevention.
Last year, Britain saw three reported cases, two of which were unrelated imported cases among travellers who had visited Nigeria. Similarly, Israel reported one case last year, an imported case involving a traveller who had been to Nigeria.
In 2003, the US saw 47 reported cases of monkeypox, attributed to a shipment of animals from Ghana.
Noting that these cases did not cause secondary transmission, infectious disease specialist Nicholas Chew from Farrer Park Hospital said the risk of a monkeypox outbreak here is "very remote".
Dr Leong said it is not difficult to differentiate between monkeypox and the common chickenpox, as the former would result in swollen lymph nodes in the neck. The rashes from monkeypox are also "much bigger, more obvious", he added.
Dr Paul Tambyah, president of the Asia Pacific Society of Clinical Microbiology and Infection, said monkeypox rash tends to start on the limbs and the palms and soles, while chickenpox rash is usually seen on the body before it spreads to the limbs.
Three other rare infectious diseases spotted here recently
Monkeypox is not the first rare infectious disease here in recent years. Here are three more.
Candida auris infection
Candida auris is a drug-resistant invasive fungus that kills nearly half of its victims in 90 days. It is not a threat to healthy individuals and has so far been seen mostly in patients with weakened immune systems. At least three cases have been seen in a Singapore hospital since 2012, said a New Paper report.
Zika virus infection
The mosquito-borne Zika virus made headlines in 2015 when thousands of people in Brazil were affected and babies were born with Zika-related birth defects.
The first locally transmitted case here was seen in August 2016, involving a woman who had no history of travel to countries affected by Zika then. About 450 people here were infected by the end of that year. As of last month, there were four Zika cases this year.
Group B Streptococcus (GBS) infection
GBS is a bacterium commonly found in the gut and urinary tract of about 15 per cent to 30 per cent of adults without causing any disease. But it may occasionally cause infections of the skin, joints, heart and brain.
A mass outbreak of 360 cases occurred in Singapore in 2015, with two fatalities. About 150 of the more serious cases were linked to the consumption of raw freshwater fish.
Lester Wong
What precautions to take when travelling in Africa
The precautionary steps to be taken when travelling to areas affected by monkeypox in Central and Western Africa:
• Maintain a high standard of personal hygiene, including frequent hand washing after going to the toilet, or when hands are soiled.
• Avoid direct contact with skin lesions of infected living or dead persons or animals, as well as objects that may have become contaminated with infectious fluids, such as soiled clothing or linen used by an infected person.
• Avoid contact with wild animals, and consumption of bush meat.
• Returning travellers from areas affected by monkeypox should seek immediate medical attention if they develop any symptoms (for example, sudden onset of high fever, swollen lymph nodes and rash) within three weeks of their return. They should inform their doctor of their recent travel history.
SOURCE: MOH


