Republic is 12th best on palliative care index
National strategy pushes it up from 18th place in 2010 in global ranking on quality of death
Sign up now: Get ST's newsletters delivered to your inbox
Singapore has been ranked the 12th best place in the world to die, up from 18th in 2010, in a global index on palliative care. It is also the second best in Asia, behind Taiwan.
ST PHOTO: JAMIE KOH
Singapore has been ranked the 12th best place in the world to die, up from 18th in 2010, in a global index on palliative care. It is also the second best in Asia, behind Taiwan.
This is according to the Quality of Death Index released yesterday by Economist Intelligence Unit (EIU).
The improvement was due largely to the drafting and implementation of a national strategy on palliative care in recent years and making such care more affordable.
Palliative care seeks to improve the quality of life of patients who have life-threatening illnesses.
As in the first ranking five years ago, Britain topped the index, followed by Australia and New Zealand.
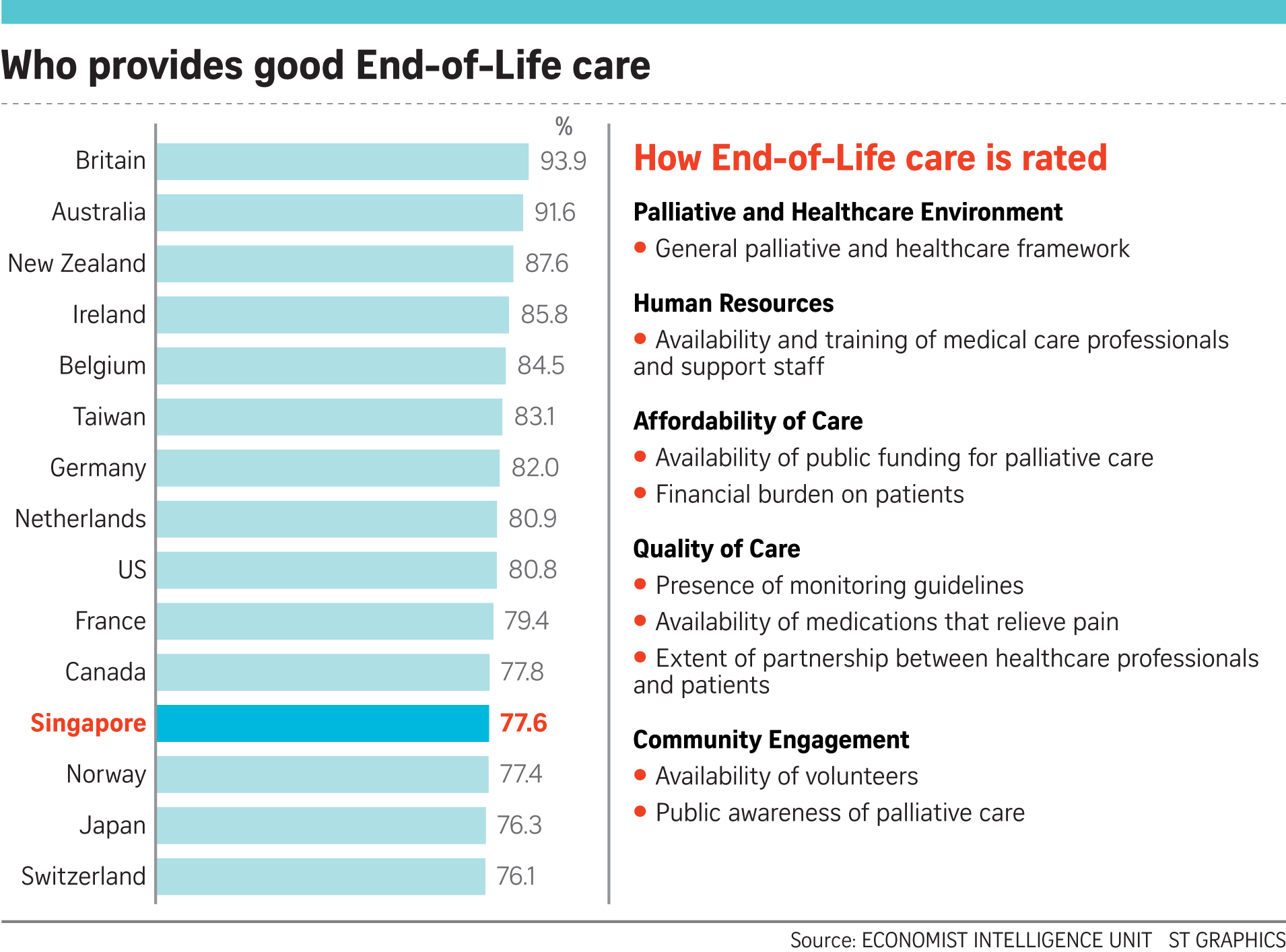
The index, which was commissioned by local philanthropic organisation Lien Foundation, ranked 80 places on end-of-life care. It is scored on 20 indicators across five categories: Palliative and healthcare environment, human resources, affordability of care, quality of care and community engagement.
In 2010, when the index was developed, Singapore was ranked 18th out of 40. The index has since been tweaked to make it more rigorous and to include more entries.
Mr David Line, managing editor of industry and management research at the EIU, said at the press conference: "The new index is structured differently from the previous one, so we can't make direct comparisons. But it is clear that Singapore has since made improvements in its palliative care definitively and relatively to others."
Singapore was strongest in affordability of care (sixth place), quality of care (eighth) and human resources (eighth), according to the index. It was the weakest in community engagement (22nd).
The EIU's 2010 index sparked a series of policy debates over the provision of palliative care around the world.
In Singapore, the first index led to the Government tasking the Lien Centre for Palliative Care to develop a coordinated national strategy for palliative care, which was released in 2012. The strategy includes coordination of care and recruitment of workers to improve palliative care. New national guidelines on end-of-life care were also unveiled last year.
Singapore's strengths in the field, according to the EIU report, include funding that lowers financial barriers, such as increasing the Medisave withdrawal limits for palliative care from January this year.
Dr Angel Lee, chairman of the Singapore Hospice Council, said: "There have been positive changes in funding, new services and in-patient facilities, guidelines and new training programmes - all in a short span of time since the implementation of the national strategy."
A new area that the report assesses is the demand for palliative care. Singapore was placed 23rd, partly because of its greying population.
Demand is rising as the population ages and the incidence of cancer and chronic diseases also increases. By 2020, more than 10,000 people a year are expected to need palliative care, up from the 6,000 patients in 2013.
Places with a high quality of death share several characteristics, said the report. These include generous subsidies for patients and strong public awareness of palliative care.
Associate Professor Cynthia Goh, chair of the Asia Pacific Hospice and Palliative Care Network, said: "Public awareness of palliative care in Singapore needs to be strengthened by getting people to talk about dying or planning for advance care as early as when they hit their 40s when they are still well."
Lien Foundation chief executive Lee Poh Wah said: "It is incumbent upon each of us to remove the barriers buried in our healthcare systems and cultural practices as well as to demand greater accountability from our governments to improve care for the dying."


