No new monkeypox cases here, but doctors must be vigilant: MOH
Sign up now: Get ST's newsletters delivered to your inbox
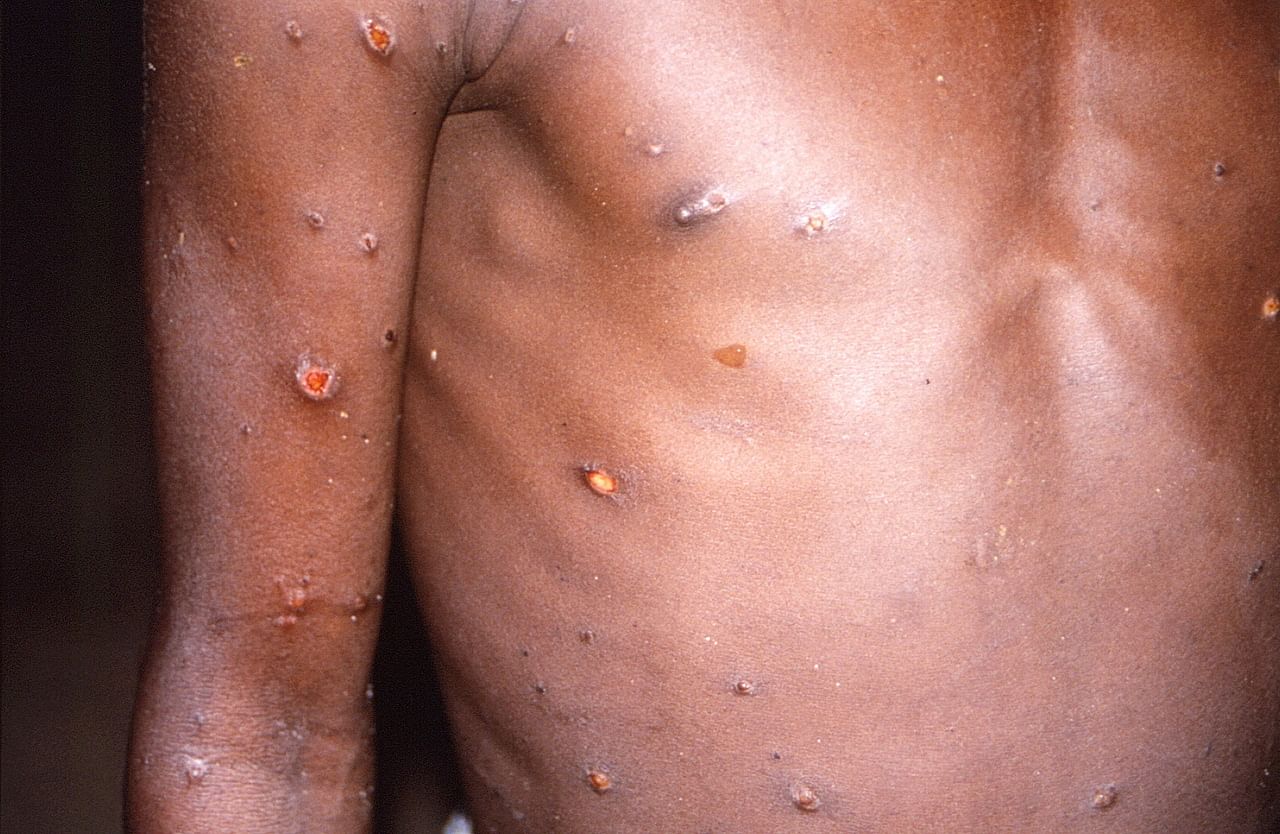
Human-to-human transmission of monkeypox, while possible, is limited, said MOH.
PHOTO: REUTERS
SINGAPORE - While there are no new monkeypox cases in Singapore, the Ministry of Health (MOH) has alerted all medical practitioners here to be vigilant in detecting and reporting cases of the disease.
The ministry said that it will continue to monitor the situation closely.
Responding to queries from The Straits Times, MOH added on Saturday (May 21) that as at Friday, no monkeypox cases have been detected here, apart from the imported case from Nigeria which was detected here on May 8, 2019.
The virus is endemic in parts of central and west Africa, but over recent weeks, cases have been detected in nine European countries, as well as the United States, Canada and Australia.
MOH said monkeypox is a rare disease caused by a virus that is primarily transmitted to humans from animals.
Human-to-human transmission, while possible, is limited.
An individual is infectious primarily during the period when they have symptoms, particularly skin rash.
"Transmission typically occurs from close contact with the respiratory tract secretions or skin lesions of an infected person, or objects recently contaminated by an infected person's fluids or lesions," the ministry said.
A spokesman for the National Centre for Infectious Diseases said the transmissibility rate will vary according to the outbreak and specific epidemiological settings.
“Generally, sustained human-to-human transmission has been rare thus far. But we will need to study this again for the current outbreak,” added the spokesman.
According to MOH, infected individuals would typically experience fever, headache, muscle ache, backache and swollen lymph nodes.
They may also get a skin rash that usually appears one to five days after the first symptoms, and which may resemble blisters caused by chickenpox.
Individuals will usually recover from their symptoms in two to four weeks.
"The disease is usually self-limiting, however severe illness and death can occur in some individuals," the ministry said.

Travellers are advised to take necessary precautions, including maintaining a high standard of personal hygiene, avoiding direct contact with skin lesions of infected living or dead persons or animals.
The ministry added that travellers should also avoid contact with wild animals and consumption of bush meat.
"Returning travellers, especially from areas affected by monkeypox, should seek immediate medical attention if they develop any disease symptoms within three weeks of their return. They should also inform their doctor of their recent travel history," said the ministry.
Infectious diseases experts said that while it will not be surprising for cases to appear in Singapore, that should not be a cause for concern as contact tracing, isolating the infected case and quarantine of contacts are likely to control the spread here, should there be any.
Dr Leong Hoe Nam, an infectious diseases specialist at the Rophi Clinic at Mount Elizabeth Novena Hospital, said: “It is a matter of time (before there are cases here). Singapore is a well-connected country. Many foreigners come in and out. A porous country like Singapore must expect cases like this.”
When asked if it could become the next pandemic, Associate Professor Alex Cook, vice-dean of research at National University of Singapore’s Saw Swee Hock School of Public Health, said: “At the early stage of any outbreak there is uncertainty on the nature of the epidemic, but so far, there is no cause for alarm.”
He added that prior to the rising cases overseas, the consensus was that monkeypox would not cause sustained outbreaks in a well-resourced country like Singapore, though importation and limited local spread may be probable.
“If sexual transmission is the main route of spread in the current outbreak, it should act as a ‘brake’ on the growth of any outbreak, because the number of contacts is much higher for respiratory pathogens than sexually transmitted ones, making contact tracing relatively easier,” he said.
He added that if any cases do appear in Singapore, the approach will be to isolate them, trace their contacts and quarantine them.
“It is hard to conceive how an epidemic of monkeypox in Singapore would get so out of hand that a community lockdown would be needed.”
Dr Leong added: “In many countries, the spread of monkeypox was stopped effectively with usual measures. It is a clear case of David versus Goliath when we compare monkeypox with Covid-19. Controlling the spread of monkeypox will be much easier.”
What happened when the first monkeypox case was confirmed in S'pore in 2019

The first imported case of monkeypox infection in Singapore, a Nigerian, was confirmed by the Ministry of Health (MOH) in May 2019.
The man, then 38, had arrived here for a workshop.
He was moved to an isolation ward at the National Centre for Infectious Diseases upon testing positive for the rare viral disease on May 8 that year.
Before arriving here on April 28, he had attended a wedding in Nigeria, where he may have consumed bush meat - a possible source of transmission of the virus.
Bush meat comes from wild animals, and is a popular source of protein in various parts of Africa, where meat from domesticated animals is scarce or expensive.
When he arrived in Singapore, he stayed at a hotel in Geylang. In the following two days, he attended a workshop in Church Street, in the Central Business District.
MOH had said then that 22 out of 23 individuals who had been identified as close contacts of the patient were placed under quarantine as a precautionary measure.
One of the close contacts, a workshop participant, had left Singapore before the patient was diagnosed.
The 22 individuals were monitored for the disease's maximum incubation period of 21 days from the last date of exposure to the patient.
They had remained symptom-free and were given the all-clear after completing their quarantine.
MOH had said on May 28 that year that the Nigerian had also recovered and had been assessed to be non-infectious.
Associate Professor Benjamin Ong, who was director of medical services at MOH at the time, said early detection, contact tracing and quarantine of close contacts enabled the ministry to tackle the case in a proactive and coordinated manner.


