NHG programme for diabetic foot disease reduces major amputations by 40 per cent
Sign up now: Get ST's newsletters delivered to your inbox
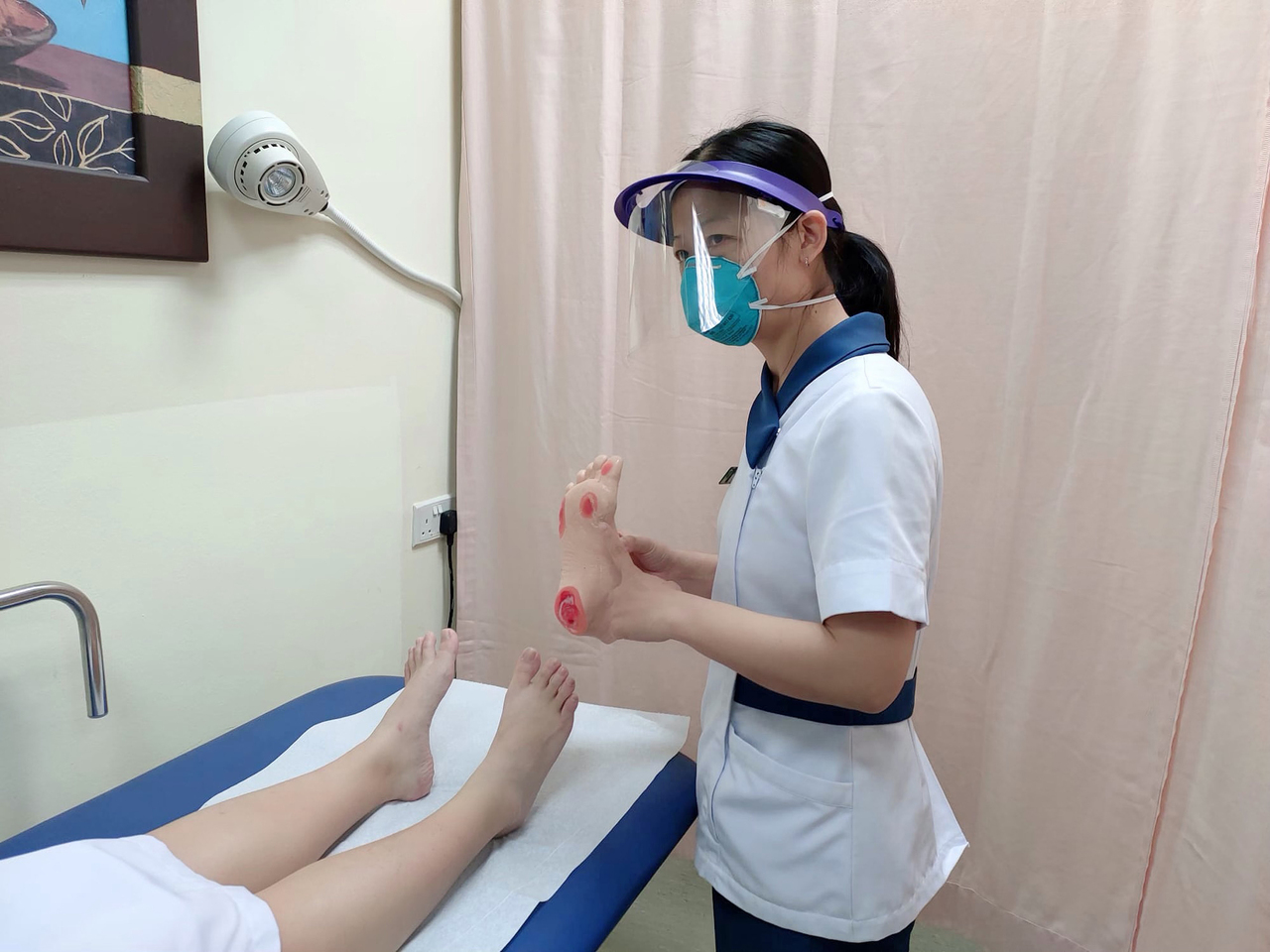
A wound care nurse educating a patient on preventing new and recurrent diabetic foot ulcers.
PHOTO: NATIONAL HEALTHCARE GROUP
SINGAPORE - An innocuous injury to his left little toe in late 2019 led to an infection that resulted in nine foot-related operations and five lower limb angioplasties in just over a year for Mr Toh Eng Cheng.
His gangrenous toe had to be amputated, and another six later, to curb a recurrence of diabetic foot ulcers, but the 52-year-old counts himself lucky.
"I could have lost the lower part of my leg or maybe the whole leg," said the former security supervisor, who has three toes left on his right foot.
"Of course, I did not like the idea of amputating my toes at first," he told The Straits Times. "But if I didn't accept it, then who knows, I might not be talking to you now," he said. He added that he is glad he is still able to walk without the need for a walking frame or walking stick.
Mr Toh is one of more than 2,700 diabetic patients who have benefited from a programme launched by the National Healthcare Group (NHG) in June last year that aims to prevent diabetes-related amputations.
Major lower limb amputations, which involve removing the leg below or above the knee, have been reduced by 40 per cent as at June this year.
Minor amputations of the foot or toes are also down by 80 per cent, thanks to the Diabetic Foot in Primary and Tertiary (Definite) Care programme, in which regular foot screenings and early treatment are key approaches.
There was also a significant improvement in diabetes and hyperlipidaemia control among patients enrolled in the programme, NHG said.
Hyperlipidaemia refers to a high level of fats in the blood, which is a major risk factor for coronary heart disease and stroke.
These interim results will be presented during NHG's 19th Singapore Health and Biomedical Congress, which will be held virtually from Friday (Oct 7).
Other topics include lessons learnt from the Covid-19 pandemic as well as other innovations in clinical care, such as enhancements to palliative care and a pilot programme for diabetic patients to better monitor their blood glucose levels.
NHG said one in three Singaporeans is at risk of developing diabetes in their lifetimes, making the disease a major public health concern.
If poorly controlled, diabetes can lead to serious complications, such as foot ulcers, which, in turn, can lead to lower limb amputations.
Singapore has one of the highest diabetes-related lower limb amputation rates in the world, with an average of four such amputations conducted here daily.
The Definite Care programme has been rolled out across NHG's polyclinics, Tan Tock Seng Hospital (TTSH), Khoo Teck Puat Hospital (KTPH), and Woodlands Health to reduce the need for amputations.
It involves doctors, nurses and allied health professionals from multiple fields, including vascular surgery, orthopaedics surgery and podiatry.
Under the programme, diabetic patients undergo regular foot screenings, get educated on foot care, and receive early and preventive treatment for mild to moderate conditions such as calluses or blisters.
Patients with more severe foot wounds or ulcers are fast-tracked and referred to TTSH and KTPH for specialist care.
For Mr Toh, who was diagnosed with Type 1 diabetes when he was in Primary 5, this means that doctors and nurses at the polyclinic he frequents know he needs to get his wounds dressed and allow him to skip the queue where possible.
It also means that he knows who to turn to for help.
Mr Toh's surgeon, Dr Joseph Lo, is the project lead for the Definite Care programme. He said diabetic foot ulcers are a problem that often recurs - up to 40 cent of the time within the same year - and requires multiple procedures to address.

These ulcers are open sores or wounds that may result from poor blood circulation or a lack of sensation due to nerve damage caused by elevated blood glucose levels.
Diabetes makes it hard for the body to heal itself, increasing the risk of wounds becoming chronic and raising the risk of infection.
If the ulcer is a small one, the aim is to prevent any amputations at all, said Dr Lo, a consultant at Woodlands Health's surgery department.
"If you come in with an unsalvageable toe, the aim is to salvage the entire leg... This gives the patient the ability to continue to live an independent lifestyle," he added.
This was the case with Mr Toh, who had gone to the polyclinic after his injured little toe turned a dark colour, indicating gangrene. This condition occurs when body tissue dies due to a lack of blood flow or a serious bacterial infection.
Mr Toh was referred to TTSH, where Dr Lo previously worked, and was later enrolled in the Definite Care programme when it launched.
Since his last surgery in December last year, Mr Toh has been ulcer-free and wears special diabetic shoes and insoles when he is out and about.
He takes extra care to ensure his legs do not get injured - keeping walkways in his home clear, leaving a light on at night, and wearing socks - and he checks for wounds every night before bed.
A small scrape or sore, if left untreated, could fester into something worse.
"Prevention is better than cure," he said.
To help diabetic patients better monitor their own wounds, NHG is trialling a mobile app that guides patients to take clear photos of a wound or ulcer.
The app analyses the images in order to detect any deterioration in condition and alerts the relevant healthcare provider.
The trial currently involves 30 patients, and NHG aims to launch the app next year.
If needed, the app will be customised to address any challenges faced by patients, caregivers and healthcare providers.


