New centre aims to lift standard of palliative care in Singapore
Sign up now: Get ST's newsletters delivered to your inbox
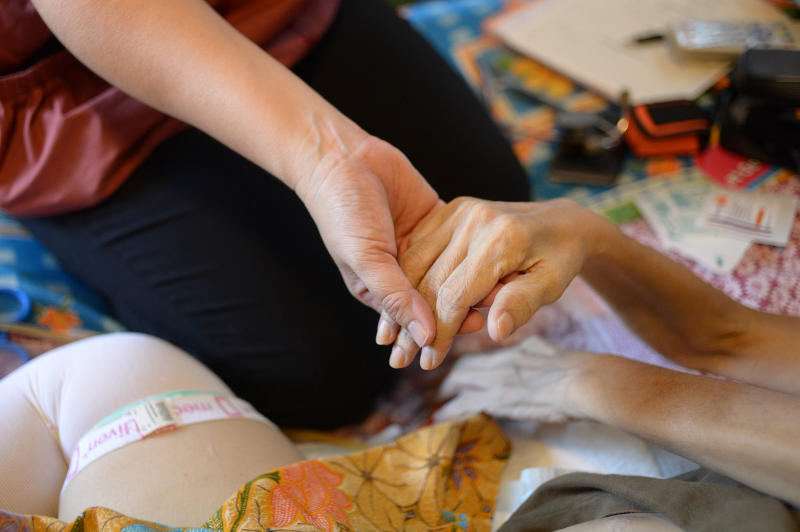
As Singapore's population ages and awareness of palliative care grows, demand for such care will undoubtedly rise.
PHOTO: MY PAPER
SINGAPORE - Mr Mah Yook Loong, 74, put off seeing a doctor for two months in 2019, preferring instead to endure excruciating pain down his spine.
He slept while seated as the pain prevented him from lying down.
"My father said if his time was up, he did not want to go for any treatment, and wanted to pass on in the comfort of home," said his daughter, Ms Mah Siew Heng, 41, a financial consultant.
When Mr Mah finally went to see a doctor, he was diagnosed with end-stage prostate cancer. "The doctor told us that if (the cancer is) untreated, he was probably left with just three weeks," said Ms Mah.
Mr Mah subsequently went for treatment, and was put under palliative care to help him manage his pain, condition and mood.
Palliative care is aimed at helping someone live with a serious, complex illness in the best way possible, improving the quality of life for the patient as well as his loved ones.
As Singapore's population ages and awareness of palliative care grows, demand for such care will undoubtedly rise. In line with this, the newly-launched SingHealth Duke-NUS Supportive and Palliative Care Centre (SDSPCC) and the Singapore Hospice Council held a virtual forum on Tuesday (March 23).
"We're not just looking at life prolongation of curative means, but giving patients what matters to them during their final days, and giving them a good closure," said SingHealth's group chief executive, Professor Ivy Ng, in her speech at the forum.
"It takes time, effort and commitment to hear each patient out to know what matters to them... and what will help them have closure. And then to try and meet those as part of a holistic care that must include compassion, pain-free comfort, dignity and peace."
The new head of SDSPCC, Clinical Assistant Professor Patricia Neo, said it wanted to raise the standard and capacity of palliative care, train more professionals in it and, in the process, help to normalise death and dying.
SDSPCC will integrate all supportive and palliative care services within the SingHealth cluster. Among other things, it has targeted to build general palliative care capacity and capability as well as specialist palliative care expertise.
Professor Neo, who is head and senior consultant at the Division of Supportive and Palliative Care at the National Cancer Centre Singapore (NCCS), said there was a need to change the culture of death and dying in Singapore.
"There's still in this old generation a kind of cultural belief that death should not be spoken about, and that it's just something that you hide away and not engage until it's in your face," said Prof Neo.
Up till some 60 years ago, people were sent to death houses in Sago Lane to await their death. Palliative care began in the country in 1985 with the 16-bed St Joseph's Hospice. providing end-of life care, and the care has considerably evolved.
More hospices were built and home hospice services were offered.
Today, there is also a focus on early palliative care, which is called supportive care, and this can be offered concurrently to say a person who is undergoing active aggressive treatment for a newly-diagnosed cancer with large tumours and may be suffering pain, she said.
This is somewhat different from late-stage palliative care for a patient who is no longer on chemotherapy, and may be in the last stages, perhaps up to one to two years, of their lives.
The palliative care team also helps the patient's family to cope, not just during the illness but also after the death.
"If we notice that some of these families need further bereavement support, that is when the hospice team comes in," said Prof Neo.
"At the moment, it is not ideal because bereavement care is something we are trying to develop and do better, but hopefully things things will improve," she added.
At the virtual forum, guest speaker Fliss Murtagh, a palliative care expert from the Hull York Medical School in the United Kingdom, said that a positive difference may well take the form of preventing deterioration, maintaining mobility or lessening the impact of symptoms, rather than an improvement in a patient's condition,
Research done over the past 30 years showed that what mattered most to patients in advanced stages of an illness include good pain and symptom control, support for the family and a reduction in the caring burden, she said at the lunchtime forum.
"The patient wants to achieve a sense of resolution and peace, and want the time and support to prepare for death," said Professor Murtagh.
Prof Neo, who's also the chairman of the Singapore Hospice Council, said that by educating the public and healthcare workers on palliative care, setting standards for it and talking about it, people will start to think of palliative care as a good option.
It is, she said, not to think about palliative care as giving up but to focus on the "dignity, personhood and maximising of the quality of life."
Mr Mah in the meantime is continuing to undergo treatment aimed at prolonging his life.

When he was hospitalised for two months after spinal surgery, he became depressed as he was going through a lot of pain. The palliative team helped and were there for her father when he could not sleep. said Ms Mah.
"They spoke to him, they called him shuai ge ('handsome man' in Mandarin)," she said.
"We felt they were not giving up on us just because it's the end-stage... It gave us hope that my dad can have quality of life. He does not need to suffer till the end."
Mr Mah not only regained his appetite but went on to have physiotherapy, and was able to return home to enjoy his daily activities such as practising qi gong and reading, said Ms Mah. The family are also going on outings more often now.


