All healthcare practices roped into plan to put patients' medical history in electronic database
Sign up now: Get ST's newsletters delivered to your inbox

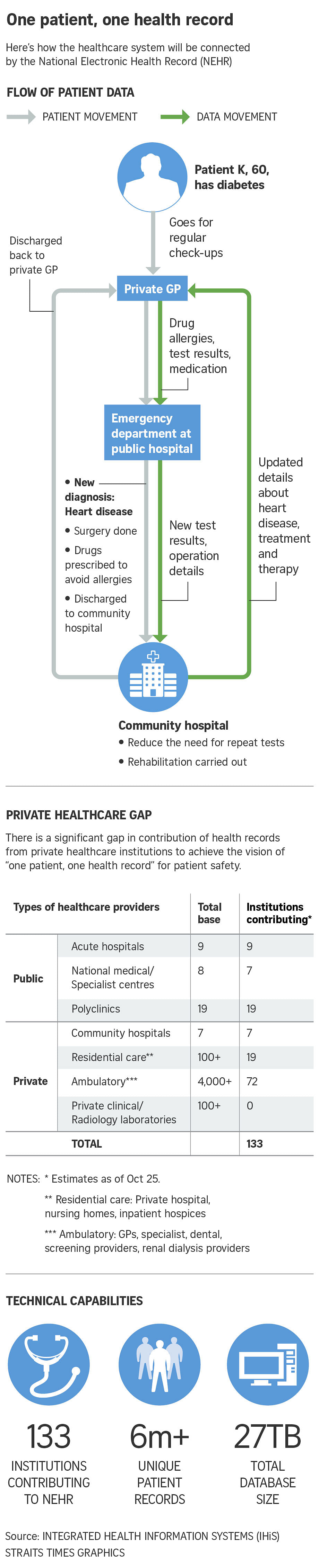
Singapore is one of the first countries to make it compulsory for all healthcare providers to upload data to the National Electronic Health Record (NEHR).
ST PHOTO: ARIFFIN JAMAR
DeeperDive is a beta AI feature. Refer to full articles for the facts.
SINGAPORE - The Ministry of Health (MOH) wants to make it compulsory for all healthcare providers to upload data to the National Electronic Health Record (NEHR) - from large hospitals all the way down to the neighbourhood GP clinic.
This means that every aspect of a person's medical history, including visits to doctors in the private sector, chronic medication, allergies and vaccination records, will be reflected in these records.
These plans come on the back of a slow take-up rate from private healthcare providers in the six years since the NEHR was launched in 2011.
Singapore is one of the first countries to have established such a comprehensive system.
The sharing of medical information in a national electronic repository will make for more seamless treatment and save money for patients, said the Government.
The proposed changes will likely be tabled in Parliament next year. If approved, healthcare groups will be given a grace period of two to three years to make the necessary preparations.
A $20 million kitty has also been set aside to help medical practices offset the costs of updating their systems.
Health Minister Gan Kim Yong made these announcements on Wednesday morning (Nov 8), at the start of the three-day FutureHealth Conference.
He said that the sharing of medical information was getting increasingly important, with more patients visiting various healthcare professionals for multiple conditions.
Currently, most NEHR data comes from public sector institutions, such as public hospitals and polyclinics.
-
Measures to protect confidentiality
Cyber-security measures to protect patients' data in the National Electronic Health Record will be similar to those used by other government agencies which deal with confidential information, said Mr Bruce Liang, who is chief executive of the Integrated Health Information Systems, which is the national technology agency for healthcare.
"The methods we use are very similar to how the Inland Revenue Authority of Singapore, for example, protects its tax database when it collects information from thousands of companies," he said.
Those who wish to access a person's health records for reasons other than their medical care - for example, a pre-employment check or for insurance purposes - must get that person's consent.
Associate Professor Low Cheng Ooi, who is chief clinical informatics officer at the Integrated Health Information Systems, said: "As long as it's not for patient care, you would need to have explicit consent from the patient."
Only 3 per cent of the more than 4,000 private healthcare providers - including specialist clinics, nursing homes and hospices - contribute to the scheme. This is despite the fact that a quarter of them have access to it and can view patient records.
A recent study of 1,500 private healthcare institutions done by the Integrated Health Information Systems - the national technology agency for healthcare - found that two in 10 private GPs and specialist clinics still use written medical records, rather than an electronic system.
"Patients can only realise the full potential of the NEHR if the data is comprehensive," said Mr Gan at the conference, which is being held at the Nanyang Technological University's Lee Kong Chian School of Medicine.
"And for NEHR data to be comprehensive, every provider and healthcare professional needs to contribute relevant data to it," he added.
Early adopters who start contributing data by June 2019 will be able to claim a one-off amount from MOH to offset the costs of upgrading their systems. The $20 million will go towards this, said Mr Gan.
The minister added that MOH will be organising workshops for doctors to help them understand the new requirements. Workshops will also be conducted for IT vendors who help doctors provide such electronic clinical management services.
Associate Professor Low Cheng Ooi, who is chief medical informatics officer at MOH, said many people move between the public and private healthcare sectors throughout their lifetimes. If private sector data is not reflected in the NEHR, this could lead to gaps in a person's medical history, he added.
The Health Ministry's chief information officer Bruce Liang said having such information on hand is especially critical in emergencies, when patients may not be in a position to recount their medical history to doctors.
Mr Liang is also the Integrated Health Information Systems' chief executive and Prof Low is its chief clinical informatics officer.
The Health Ministry plans to introduce the changes under the Healthcare Services Act so that all healthcare providers will be legally obliged to follow through with its plans. If the changes go through, those who do not comply will likely face penalties.
"This will not be an easy journey," he added. "The state of IT adoption is uneven across the 4,000-over healthcare institutions in Singapore, and there are a large number of IT solutions providers with a wide variation of offerings... However, it is a journey we must make, as a strong digital backbone is essential in meeting our patients' and healthcare system's needs in the future."
At the conference, Mr Gan also launched the Healthcare Industry Transformation Map, which will help chart the path for Singapore's healthcare system.
He said that the ministry will build a strong local core in the healthcare workforce, help people "work smarter" to enhance productivity, and push innovation across the sector.
For more info about the NEHR, click here.


