Cutting-edge technology sharpens treatment
Sign up now: Get ST's newsletters delivered to your inbox
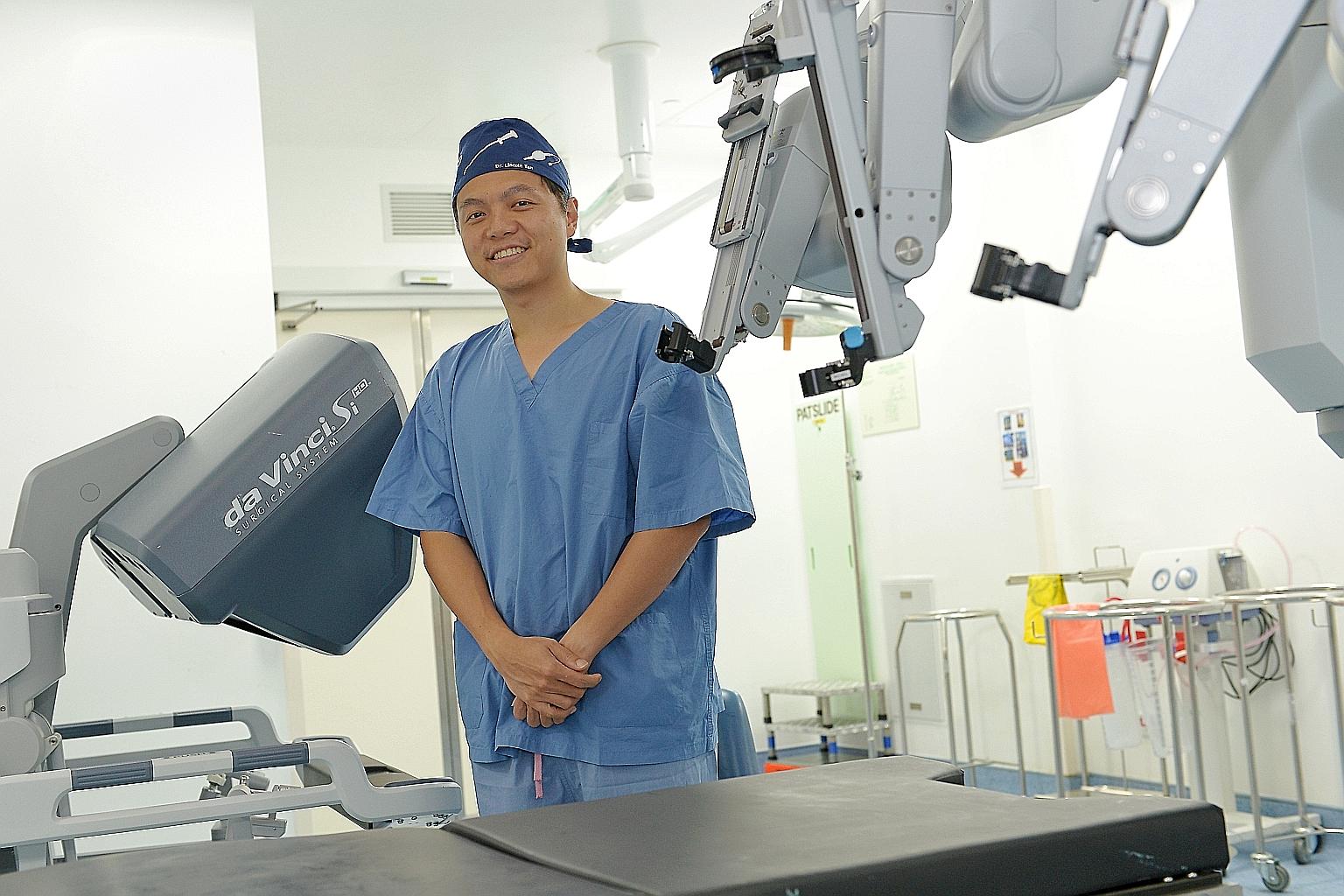
The "da Vinci Surgical System" is more precise at microscopic procedures than human hands.
ST PHOTO: DON CHI
Cutting-edge developments, from genetic profiling to automated decision-making by computers, are bringing benefits to men with prostate cancer.
Dr Lincoln Tan, consultant at the National University Cancer Institute, Singapore (NCIS), said researchers are developing molecular markers to identify different types of prostate cancer in order to ascertain the most appropriate treatment, including which drugs to use.
He added that as these medications are expensive, knowing this beforehand would prevent patients from "wasting time and money on a drug that won't work for them".
Another treatment is simply to remove the prostate gland, which is now a less messy procedure than in the past, thanks to a robot named after one of the world's greatest inventors.
The "da Vinci Surgical System", approved by the United States Food and Drug Administration in 2000, executes microscopic surgical manoeuvres more precisely than human hands can, and is controlled by the surgeon using joysticks at a remote console.
This minimises blood loss, lowers the risk of nerve damage and shortens the hospital stay.
Headway is also being made in radiotherapy, which often uses highly penetrating gamma radiation to kill cancer cells.
Radiotherapy sessions for prostate cancer used to last eight weeks, a relatively long period compared to cancers like lymphoma, for which treatment takes about three weeks, said Dr Keith Lim, senior consultant at NCIS.
"The cell turnover rate is a bit slower, so you need to give more radiation over a longer period of time in order to kill more cells."
But now, for patients in which the prostate cancer has not spread to the surrounding tissues, doctors can "nuke it" in three days with the latest technology, said Dr Lim.
The strong radiation, however, has to be administered in a very precise manner, or it will kill too much healthy tissue.
This is accomplished using brachytherapy, in which radioactive "seeds" are implanted directly into or adjacent to the tumour through hollow plastic needles inserted into the prostate gland.
This technique is also used for breast, cervical and oesophagus cancers, among others.
Dr Lim said researchers have worked out the optimal strength and frequency of radiation through clinical trials.
The doctor decides on the strength of radiation required for a particular patient depending on the severity of the cancer.
This information is passed on to the computer, which then works out where to position the radioactive seeds for durations as short as half a second.
The doctor can also manually tweak the settings while therapy is in progress, said Dr Lim.
Subsequently, data on the outcome of the treatment can be fed back into the computer to continually improve its decision-making algorithm.
Dr Lim said this is part of a wider array of computerised decision-making tools in healthcare that is not yet commercially available in Singapore, but will be introduced at the National University Hospital within the next five to six years.
These tools account for various patient-specific factors to help doctors and patients decide on the best treatment.
Find out more about cancer and how to fight it on ST's Fighting Cancer microsite.


