Crowded emergency depts: Experts look at UK’s pilot model
Sign up now: Get ST's newsletters delivered to your inbox
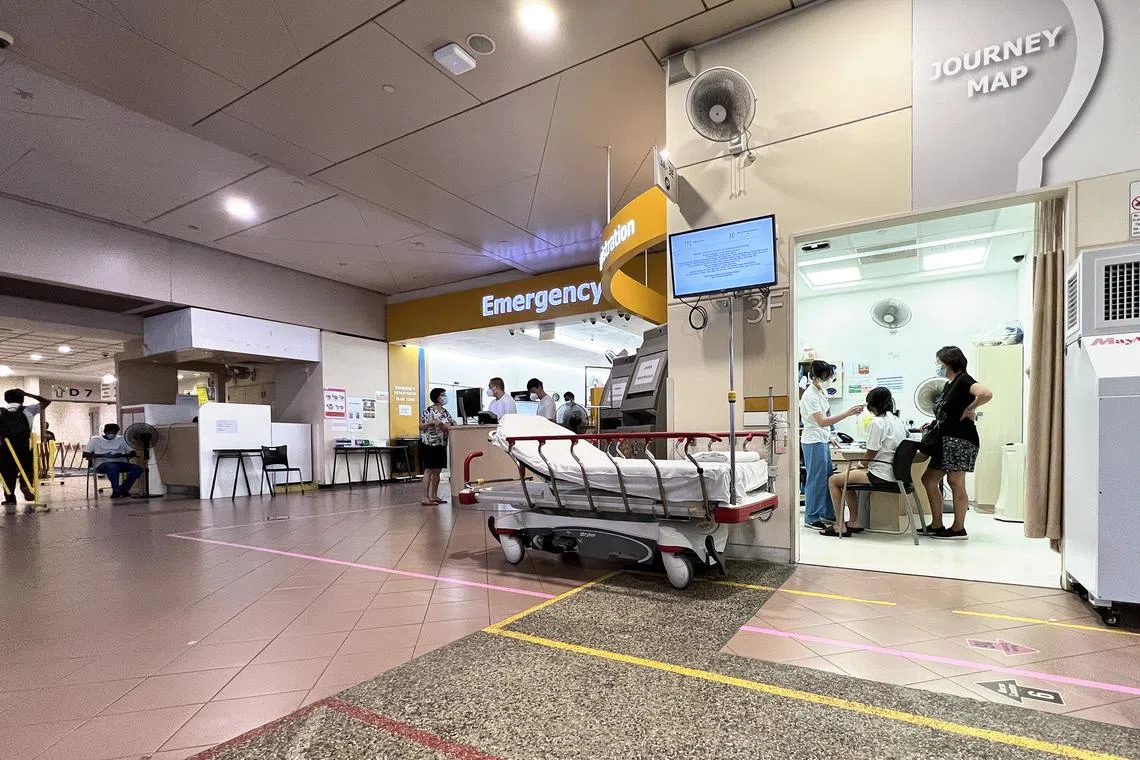
In Singapore, the problem of overcrowding at EDs has been around for years, but has become worse with the Covid-19 pandemic.
ST PHOTO: ALPHONSUS CHERN
SINGAPORE - Like the emergency departments (EDs) in Singapore, those in England’s hospitals are overcrowded, and its National Health Service (NHS) is looking at moving patients out of the ED to a ward to ease the load.
This “continuous flow model”, already piloted in some places in England, involves ED patients being moved out even when no beds are available in the wards.
This means they may have to share a bay or side room with another patient in the ward, said an article in the Oct 25 issue of the British Medical Journal (BMJ).
“The scheme aims to reduce numbers of ambulances queueing outside emergency departments and to encourage wards to discharge and so reduce blockages in patient flow,” the article explained.
NHS England’s interest in such a scheme comes amid record delays in hospital and ambulance response times in September.
“More than 30,000 patients were delayed for 12 hours or more from the decision to admit to actual admission, the highest on record,” said the article. It quoted data from NHS England, which oversees 875 hospitals.
In Singapore, the problem of overcrowding at EDs has been around for years, but has become worse with the Covid-19 pandemic.
Compared with what is happening in Singapore’s public hospitals, a 12-hour delay does not seem like a very long wait.
The latest statistics from the Ministry of Health showed that half the patients at Khoo Teck Puat Hospital’s ED who needed to be admitted on Oct 17 had to wait for more than 39.2 hours.
The same day, half the patients at Ng Teng Fong General Hospital waited in the ED for more than 34.4 hours to get a bed in a ward, after a doctor had determined that the patient needed to be hospitalised.
The data does not show what the longest wait was.
However, although not always achieved, NHS England has a target for 95 per cent of patients in the ED to be discharged or warded within four hours.
Hospitals that fail to do so can be fined. So a wait of 12 hours or more is a major breach of this goal.
Dr Adrian Boyle, president of the Royal College of Emergency Medicine (RCEM), strongly supported the model to move patients out of EDs regardless of the hospital bed situation.
He told BMJ: “The RCEM has always argued that if you spread the risk across the whole patient pathway, you dilute the risk. It’s important to realise that this may not work in every setting, as hospitals vary enormously in their estate and how their flow models work.
“However, the risks in emergency departments are so significant at the moment – and that has knock-on effects in the ambulance service – that I think it is beholden on people to at least consider an attempt and try this.”
But not all doctors agree with him. Dr Nick Scriven, past president of the Society for Acute Medicine, was quoted as saying: “Simply offloading patients does not ‘share the pressure’. It merely changes its point of focus from relatively well-staffed emergency departments to much less staffed other areas.”
Dr Boyle said in response: “We understand that inpatient wards and teams are under enormous pressure. We don’t want this to be seen as a ‘them and us’ issue. We are trying to spread the risk across the system.”
He added that it all comes down to clinical leadership. If it is prepared to take a system-wide view, this can be made to work.
Professor Philip Choo, group chief executive of the National Healthcare Group which runs Khoo Teck Puat Hospital and Tan Tock Seng Hospital, thinks such a move provides a good interim measure to ease the crowded EDs here. “It’s safer to spread the load and have more eyes, hands and feet sharing the load than have EDs bear the burden alone.”
Associate Professor Jeremy Lim of the National University of Singapore’s Saw Swee Hock School of Public Health said this is a reasonable approach. Hospitals here should start developing guidelines and clarity on how applicable this model will be and for which patients.
He added: “There is no one-size-fits-all and the decision for ‘corridor beds’ has to be based on the patient and the hospital.
“Is the patient better off in the ED waiting or in a ward, albeit in a ‘corridor bed’? What’s the impact on the other patients, whether in the ED or in the ward?”



