Covid-19 booster jabs: Some may not get same vaccine from earlier shots
Sign up now: Get ST's newsletters delivered to your inbox
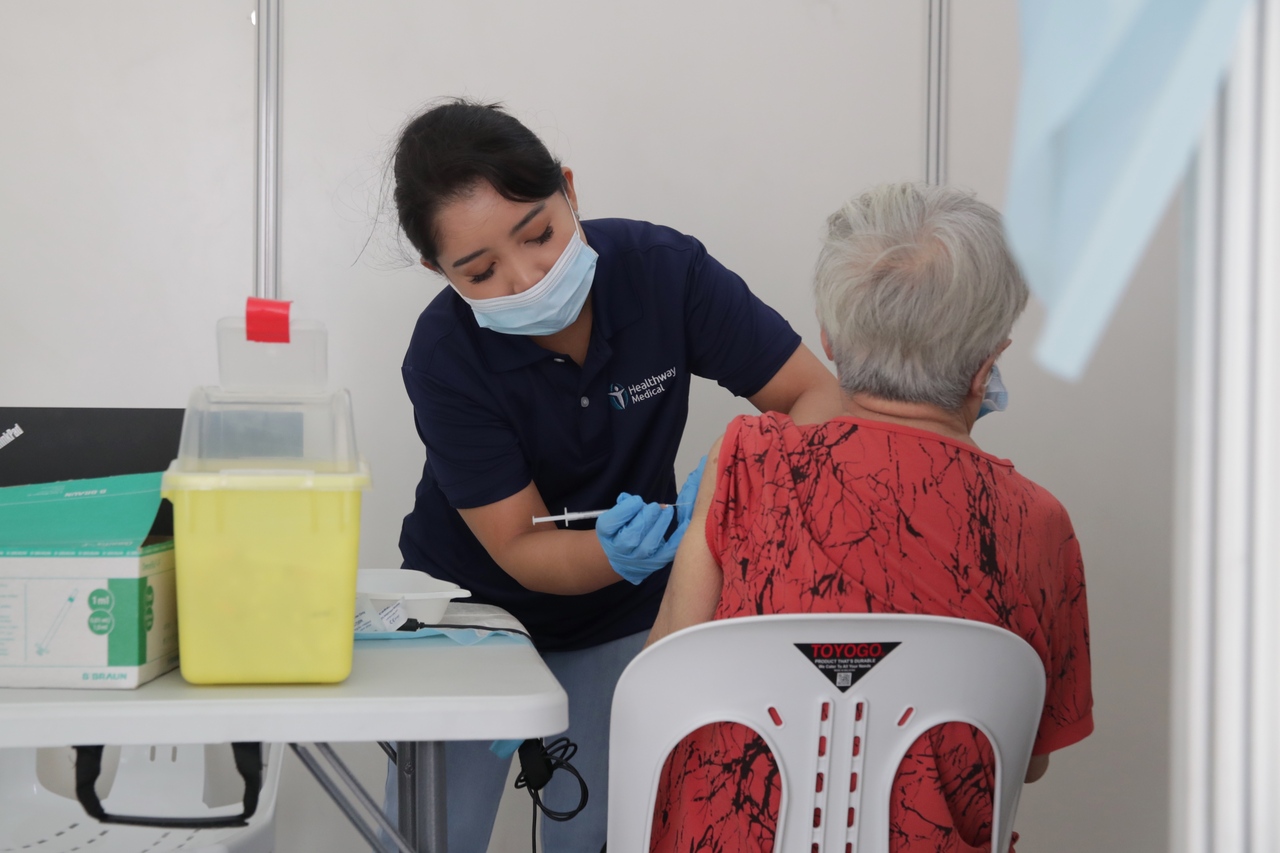
A vaccine booster is an extra dose of a vaccine given to maintain or augment the protection provided by the original dose or doses.
ST PHOTO: GIN TAY
SINGAPORE - When Covid-19 booster shots are rolled out in Singapore, some may be given the same vaccine they took earlier while others may be administered a different one.
"Both approaches are being considered, with pros and cons to both strategies," Associate Professor Lim Poh Lian, director of the High Level Isolation Unit at the National Centre for Infectious Diseases, told The Straits Times.
"We have to look at which is more effective in protecting against the current and future virus strains circulating. We have to look at safety issues and different segments of the population.
"What might be good for older adults might have more side-effects in younger persons, so it may not be a one-size-fits-all recommendation. Those kinds of data just take time to be collected, analysed and reported," said Prof Lim, who is also a member of the Expert Committee on Covid-19 vaccination.
Those who got inactivated Covid-19 vaccines such as Sinovac may benefit from receiving an mRNA booster jab, some experts said.
mRNA vaccines include the Pfizer and Moderna vaccines, which are part of Singapore's national vaccination drive.
Professor Ooi Eng Eong from Duke-NUS Medical School's Programme in Emerging Infectious Diseases explained: "Inactivated vaccines do not generate appreciable levels of killer T-cells. Such individuals thus rely mainly on a single line of defence - their antibodies."
Associate Professor Hsu Li Yang, vice-dean of global health and Infectious Diseases Programme leader at Saw Swee Hock School of Public Health, pointed out that China is reportedly considering the use of an mRNA vaccine as a booster following the primary vaccination with the Sinovac or Sinopharm vaccine - the reason being to broaden coverage against other Covid-19 variants, including the Delta variant.
"Neutralising antibody levels appear to drop rapidly six months post-Sinovac vaccination, which is the other reason for considering a booster dose with either an mRNA or the same vaccine," he added.
The experts agreed, though, that with different countries taking different approaches, there is a need for more data before a decision is made.
Britain, for example, is looking into mixing its vaccines for booster doses, after results from its Com-Cov study launched in February showed that administering one dose of the Pfizer vaccine after a dose of the AstraZeneca jab could help to boost the immune response.
But Israel - the first country to administer booster shots of the mRNA vaccines to those aged 60 and older and recently extended the booster shots to those above 30 - has decided not to do this.
Prof Lim said that the vaccine committee is also studying several other things, including the incidence rate of adverse reactions from a booster shot in other countries and the steps that can be taken to remove or mitigate the risk.
She acknowledged that there are theoretical concerns about the side-effects of a third dose of vaccine, though countries such as Israel and the United States which are already implementing boosters can soon provide real world data on the effectiveness and safety of these approaches.
She noted that Moderna has tested different doses for its booster, and the US Food and Drug Administration (FDA) has held discussions with the company on which dose provides the best combination of effectiveness and safety.
The Moderna vaccine contains 100 micrograms of vaccine a dose, while the Pfizer has 30 micrograms a dose.
Asked if a booster shot at a lower dose was more favourable in preventing adverse side-effects, Prof Lim said that dosages are not directly comparable between vaccines, or other medications.
"Even in the same class of high blood pressure medicines, 5mg of one medicine may have the same therapeutic effect as 50mg of another medicine," she added.
On who should get the boosters first, Associate Professor David Allen, an infectious diseases clinician at the National University of Singapore's Yong Loo Lin School of Medicine, said: "If the goal is to decrease hospitalisation, severe disease and death, then give the booster to those people it has been shown to be efficacious for - such as the immunocompromised...and probably the elderly."
How do booster jabs work and when should they be given?
Prof Hsu said that a vaccine booster is an extra dose of a vaccine that is given to maintain or augment the protection provided by the original dose or doses.
"It will augment (or boost) whatever part of the immune system that the original vaccine targets, so in the case of Covid-19 vaccines, it will probably increase the number of memory B- and T-cells in addition to the level of circulating antibodies targeting the Sars-CoV-2 virus," he said.
Memory B-cells help to produce antibodies on demand which target the virus and its variants, thus preventing severe lung disease, while T-cells are able to detect and kill infected cells to prevent the Sars-CoV-2 virus from spreading.
Prof Ooi noted that some have suggested monitoring antibody levels and giving boosters to those with waning levels of antibodies against the Sars-CoV-2 virus.
"However, antibody measurements alone are insufficient to guide such decision-making on booster shots, and doing so would miss out on all the different ways in which the immune system is able to protect us from Covid-19," he said.
Prof Hsu pointed out that the experiences of Israel and Britain show that the protection from asymptomatic and mild infection decreases within six months post-vaccination, particularly with the Pfizer vaccine.
"However, these same experiences also show that protection against severe Covid-19 disease (cases requiring hospital care, oxygen support) remains excellent, with more than 85 per cent effectiveness when compared with unvaccinated people, even for the elderly," he said.
"Will protection against severe disease wane over time? We do not know for sure at this point if and when this will happen, but it will certainly take a far longer period of time compared with protection against infection," Prof Hsu added.
He pointed out that different vaccines affect the immune system differently, so current results cannot be extrapolated to other vaccines, such as the Moderna shot.
As to how often the Covid-19 jab should be administered, Prof Paul Tambyah, president of the Asia Pacific Society of Clinical Microbiology and Infection, said that it is still too early to tell - though it might be the case that Covid-19 is like hepatitis B or measles, each of which needs three jabs.
"It is highly unlikely that we will need annual jabs as the mutation rate is much lower than influenza," he said.
Likewise, Prof Ooi added that there is no fixed formula for when booster shots should be administered.
"The immune response does not wane at a fixed rate but varies from vaccine to vaccine and infection to infection. Moreover, how much immune response is needed to prevent infection and disease varies from virus to virus. There is thus no theoretical way to estimate when booster shots are needed," he said.
He suggested that a more accurate way of determining when to administer booster shots would be to conduct active surveillance of Covid-19 cases in hospitals to guide decision-making.
Once a trend towards an increase in severe Covid-19 cases among the vaccinated is observed, then perhaps there will be sound evidence for the need of booster shots.
This approach should also apply to special groups of the population, including people with compromised immune systems, he added.
Prof Lim also said that waning immunity may be more of a problem in such people, as well as older adults.


