Covid-19 antibody cocktail treatment to arrive in Singapore in October
Sign up now: Get ST's newsletters delivered to your inbox
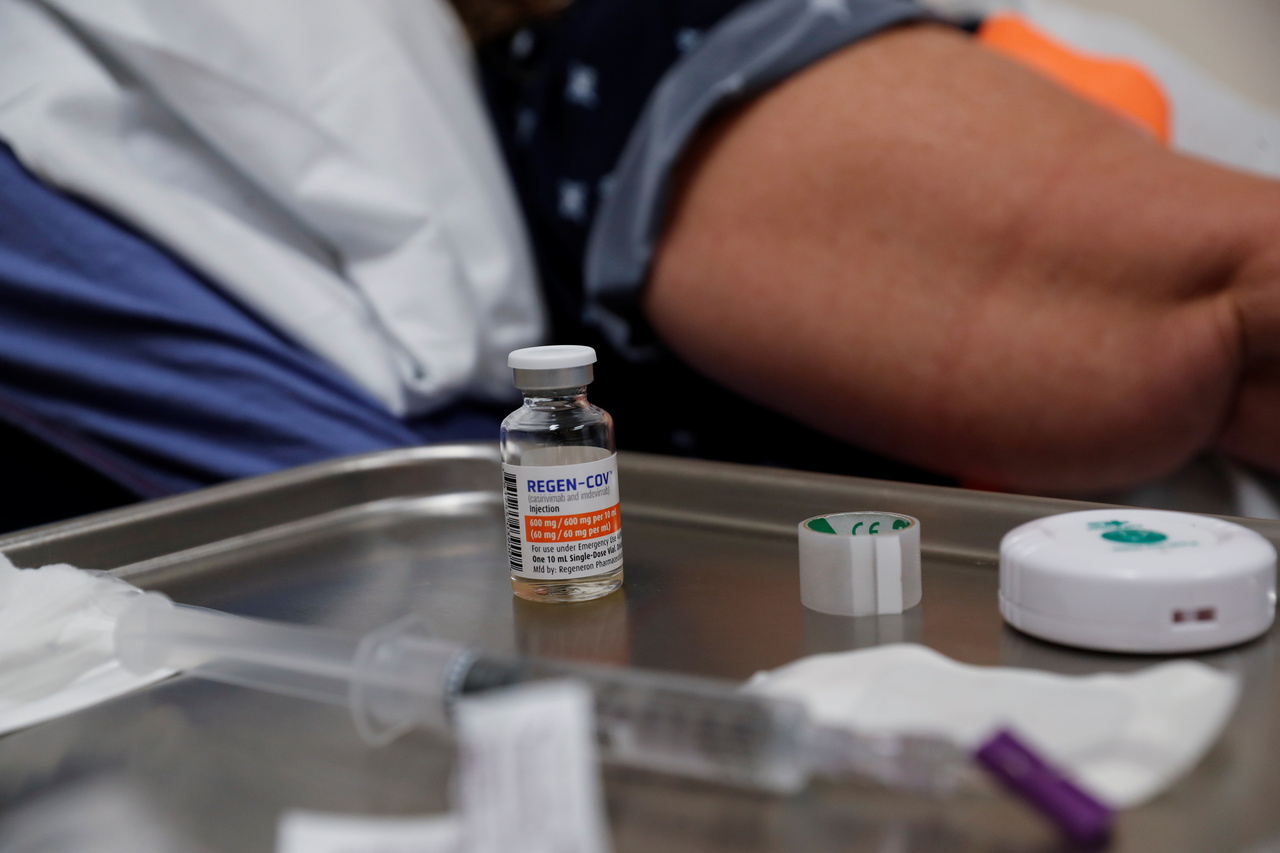
A vial of Regeneron monoclonal antibody. Monoclonal antibodies are laboratory-made proteins that act like antibodies in helping the body to fight off infection.
PHOTO: REUTERS
SINGAPORE - More treatments are now available here for Covid-19 patients, as Singapore continues to battle against a rising number of coronavirus infections.
The latest addition to this arsenal of treatment options is a Covid-19 antibody cocktail, which was developed by Regeneron and Roche. It is expected to arrive here next month or so, the National Centre for Infectious Diseases (NCID) said on Tuesday evening (Sept 28) in response to queries from The Straits Times.
This monoclonal antibody treatment can be used to treat patients who are mildly sick but at risk of severe illness.
It was granted interim authorisation to be used for the treatment of patients with mild to moderate Covid-19 under the Pandemic Special Access Route (PSAR) by Singapore's Health Sciences Authority (HSA) on Sept 21.
HSA said on its website that infectious diseases specialists will be able to use this therapy for those aged 18 and older, who do not require oxygen supplementation and are at risk for progression to severe Covid-19.
An ongoing phase three study that HSA reviewed has found that this antibody treatment cut the relative risk of Covid-19 disease progression to requiring acute treatment in hospital or death by 70 per cent, compared with the placebo group.
Symptoms also cleared up an average of four days earlier compared with the placebo group.
On Sept 24, a World Health Organisation panel also recommended the use of this antibody cocktail for patients at high risk of hospitalisation and those severely ill who had no natural antibodies.
The treatment was granted US emergency use authorisation in November last year, having gained attention when used to treat former president Donald Trump's Covid-19 illness last year. Europe is reviewing the therapy, while Britain approved it last month.
Apart from this antibody cocktail treatment, there are four other drugs in use to treat Covid-19 here.
Antibody drug sotrovimab
As at Sept 22, 64 NCID patients here have been on sotrovimab. The drug was made available to healthcare institutions from this month.
Sotrovimab is a single-dose monoclonal antibody drug administered through intravenous infusion.
Monoclonal antibodies are laboratory-made proteins that act like antibodies in helping the body to fight off infection.
It can be used to treat patients who do not require oxygen supplementation and have mild to moderate Covid-19 disease but are at risk of progressing to more serious illness.
The drug, developed by GlaxoSmithKline and Vir Biotechnology, was granted interim authorisation under the PSAR by HSA on June 30.
Arthritis drug tocilizumab and steroid dexamethasone
As at Sept 22, 60 NCID patients have been on tocilizumab and approximately another 290 on dexamethasone.
Manufactured by Swiss drugmaker Roche, tocilizumab is an intravenous anti-inflammatory monoclonal antibody used to treat rheumatoid arthritis.
It has been reported to reduce the risk of death in hospitalised patients with severe Covid-19, especially when combined with the steroid dexamethasone, a cheap and widely used steroid used to reduce inflammation in other diseases.
These drugs are given to patients in intensive care with hyper-inflammation and have been shown to decrease mortality, Dr Shawn Vasoo, clinical director of NCID, said.
Researchers in Britain have also found that the drug also shortened patients' length of stay in hospitals and reduced the need for a ventilator.
The study was part of the Recovery trial, an international clinical trial that has been testing a range of potential treatments for Covid-19 since March last year.
Antiviral drug remdesivir
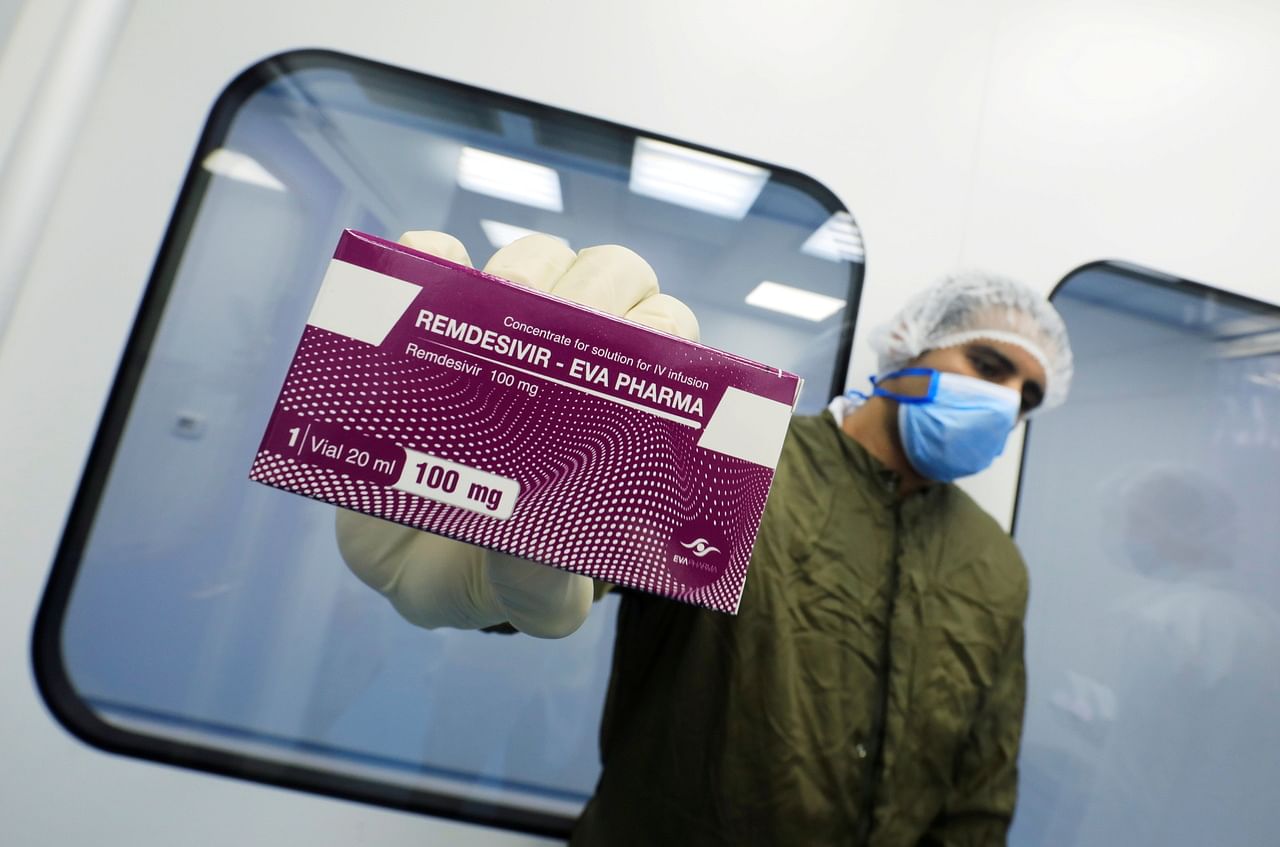
<p>FILE PHOTO: A lab technicians shows the coronavirus disease (COVID-19) treatment drug "remdesivir" at Eva Pharma Facility in Cairo, Egypt June 25, 2020. REUTERS/Amr Abdallah Dalsh/File Photo</p>
PHOTO: X90179
As at Sept 22, 580 NCID patients have been treated with remdesivir.
Administered in the early stage of Covid-19 illness, it hastens time to recovery.
Remdesivir, developed by United States drugmaker Gilead Sciences, received conditional approval from HSA to be used outside of clinical trials in June last year.
There are also some repurposed drugs that have not proven useful for Covid-19 treatment.
Dr Vasoo said that while some of these drugs may have demonstrated activity against the virus in a lab setting, their results in real-life clinical studies still remain to be seen.
The definitive way to assess a drug's efficacy is through a double-blind randomised controlled trial in which at least two groups of patients get the drug or placebo or receive standard care, and neither the investigators nor the patients are aware of what treatment was given.
Some of these drugs include:
Ivermectin, a medication used to treat parasitic infections
While many have called for ivermectin to be used as part of an outpatient treatment plan for Covid-19, data regarding it has been fraught with inconsistencies, Dr Vasoo said.
At least two trials claiming its use showed serious flaws, with one being retracted for possible plagiarism and data flaws.
Other more robust randomised controlled trials have not shown ivermectin to have any effect in preventing hospitalisation or an earlier resolution of symptoms.
"Ivermectin cannot be recommended at this point as part of the standard therapy of Covid-19, outside of well-designed clinical trials," Dr Vasoo said.
Anti-malaria drug hydroxychloroquine and antiretroviral drugs
Hydroxychloroquine and antiretroviral drugs commonly used to treat the human immunodeficiency virus (HIV) - such as lopinavir-ritonavir - have not shown efficacy in randomised controlled trials to date, Dr Vasoo said.
"The major definitive trials which have informed practice have been completed. It is unlikely that any further new, ground-breaking trials will be attempted," he said.
Gout medication probenecid
Probenecid, a medication that is primarily used to treat gout and has broad antiviral properties, was studied in the lab and showed activity in blocking replication of Sars-CoV-2, the virus that causes Covid-19.
However, there is no current robust human trial data yet, Dr Vasoo said.
At present, Singapore is not looking into this drug in relation to Covid-19 treatment.


