Cases of public healthcare workers being abused doubled between 2022 and 2024: MOH
Sign up now: Get ST's newsletters delivered to your inbox

Between 2022 and 2024, the number of abuse and harassment incidents reported by public healthcare institutions increased from about 1,500 cases to 3,000 cases annually.
PHOTO: ST FILE
- The Tripartite Framework, launched in December 2023, defines what constitutes abuse and harassment.
- The framework provides standard protocols for healthcare workers to address abuse, leading to fines, and imprisonment for some offenders.
- Hospitals offer support for abused staff, including counselling, and empowerment to intervene, recognising lasting emotional impact.
AI generated
SINGAPORE – When nurse manager Siti Yusirah A. Majid told a patient he could not change his dressing without supervision, the angry man threatened to throw a pair of scissors at her.
Her colleagues at Ng Teng Fong General Hospital (NTFGH) alerted security and called the police, who arrested the man.
The hospital had also forcefully discharged two abusive patients – once they were medically stable – with the help of security.
The number of abuse and harassment incidents reported by public healthcare institutions increased from about 1,500 cases to 3,000 cases annually between 2022 and 2024, a Ministry of Health (MOH) spokesperson said.
This comes after the implementation of the Tripartite Framework for the Prevention of Abuse and Harassment in Healthcare that was launched by Health Minister Ong Ye Kung in December 2023.
It includes a common definition of abuse and harassment, and standardised protocols for response and measures that can be taken against abusers.
Ms Siti has been a nurse for 15 years and has on many occasions faced verbal abuse from patients when their demands were not met. In the past, she accepted such behaviour as part of the job – but not any more. Reflecting on her experience, she said: “Back then, we didn’t know what was considered abuse, because shouting happens a lot, so we used to just take it. But now we know it is abuse, and we know (we should report it).”
Under the framework, abuse and harassment are defined as words, communications, actions or behaviours that are inappropriate, threatening and insulting, and cause a healthcare worker to feel intimidated, alarmed or distressed.
Dr Lim Jia Hao, senior consultant at the Singapore General Hospital’s (SGH) emergency department, said the most common form of abuse is verbal, followed by physical. He said: “Harassment is also a form of abuse which is increasingly being reported. Some cases arise from reasons we can empathise with – frustration from waiting, physical or emotional discomfort during treatment, or patients lacking mental capacity or under the influence of intoxicants.
“However, many other cases stem from unacceptable reasons such as racial or gender discrimination, unreasonable demands and unprovoked aggression.”
Abusive patients forcefully discharged
The framework also details standard protocols for dealing with such incidents, such as firmly telling the perpetrators to stop, activating security personnel or administering restraints on the abuser as a last resort.
Dr Lim said SGH staff are empowered to intervene whenever instances of abuse occur, usually by warning perpetrators, and to call for help during high-risk situations.
He said complex cases involving repetitive or recalcitrant behaviour are reviewed before formal warnings are issued. Clearly severe or criminal offences – such as physical assault, sexual harassment and outrage of modesty – are referred to the police.
Dr Lim added: “Some abusive patients have been discharged with the assistance of security, but only after medical treatment has been completed and they are deemed clinically fit for discharge, and their continued presence is preventing care from being delivered to other patients due to their disruptive behaviour.”
Ms Ng Sow Chun, who is the chief nurse at NTFGH and Jurong Community Hospital, said NTFGH has forcefully discharged abusive patients since the framework was implemented.
Ms Ng is also the tripartite representative for the National University Health System (NUHS), which comprises the National University Hospital, NTFGH, Alexandra Hospital and Jurong Community Hospital. She said: “For such patients, if they require (outpatient) follow-ups, we make arrangements for them to return, but make it very clear that we do not allow abusive behaviour.”
When it comes to abusive behaviour, a spokesperson for NUHS said it adopts a zero-tolerance stance and has taken steps over the past years to protect its employees.
For instance, NUHS’ internal framework has identified ward-based activities that may carry a higher risk of incidents involving outrage of modesty and other forms of abuse. These include adult diaper changing, assisted showers, bathroom visits, transferring patients during therapy, responding to patient calls in the early hours of the morning, and calming agitated patients. It also highlights the corresponding safety measures to mitigate these risks for its staff.
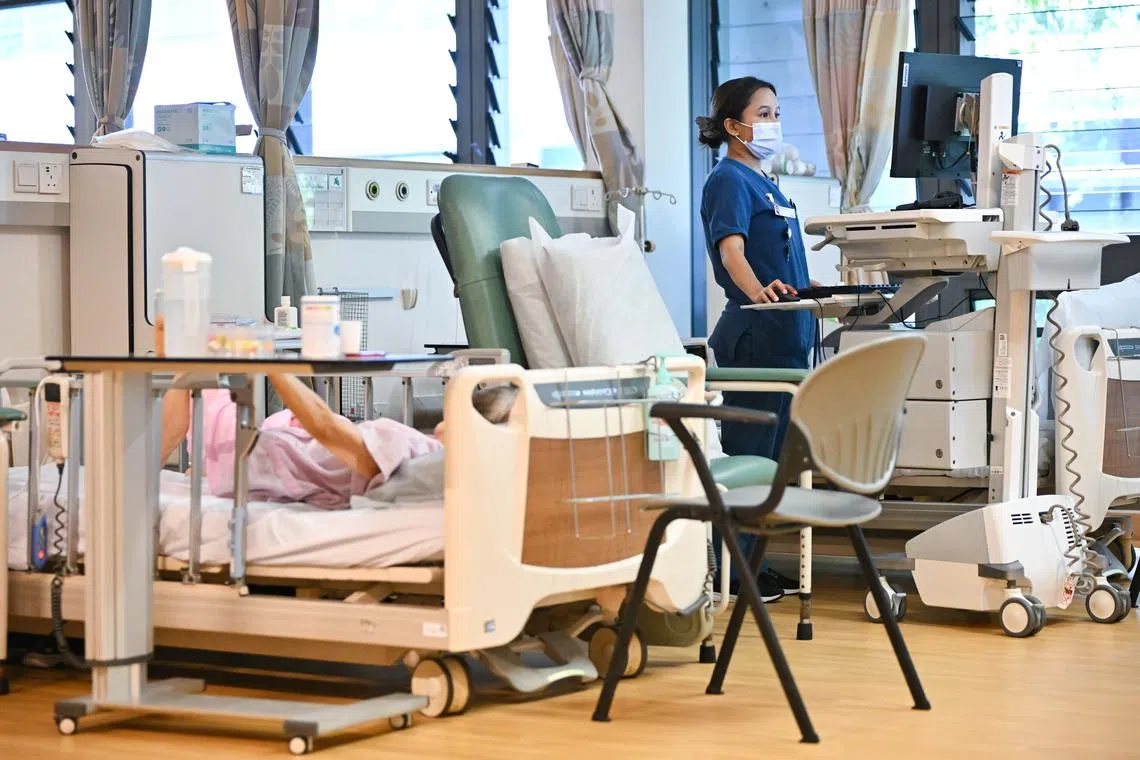
The National University Health System’s internal framework has identified ward-based activities that may carry a higher risk of incidents.
ST PHOTO: LIM YAOHUI
NUHS staff are encouraged to speak up and seek help from their peers and supervisors if they face abusive behaviours.
They are also taught self-protection techniques, and are trained to support one another through peer support courses that teach them how to intervene and assist their colleagues during incidents.
In the event of abuse, or if there is a threat of physical harm, NUHS activates its security staff or calls the police. A warning in the form of a code of conduct agreement will be issued to abusive patients, in which the hospital reserves its right to refuse non-emergency medical treatment to these patients, or revoke visitation rights to abusive visitors or next of kin.
Said the NUHS spokesperson: “Abusive next of kin and visitors may also be escorted out of the hospital by our security team if their behaviour persists despite attempts at verbal management. Legal recourse will be taken against egregious perpetrators who continue to behave in an unacceptable manner.”
Culprits can be charged under the Protection from Harassment Act. If convicted, they can be fined up to $5,000, jailed for up to 12 months, or both.
In the past three years, some abusive patients have found out that their behaviour would not be tolerated. On Jan 13, a 42-year-old man was sentenced to 10 months’ jail for molesting a nurse during a medical check-up.
And in October 2023, a woman who verbally abused an SGH employee was sentenced to five weeks and five days’ jail, and fined $600.
Months of trauma
Ms Ng said hospital staff who experience abuse can be left in shock, even months after the incident.
She said a nurse once politely advised a patient’s son to not use a folding chair in the ward during the day, as it obstructed movement and could affect safe care delivery. Such chairs are offered to registered caregivers for use after visiting hours.
The family member reacted by throwing the chair at the nurse.
“Although she was not injured, she was shocked and shaken. She was still affected by it when I followed up with her six months later,” Ms Ng said.
The hospital understood that the patient’s son was fined in court.
Ms Ng added that NTFGH staff who have been abused can turn to their seniors and in-house counsellors for support, or approach the care and protection team and senior management.
To prioritise staff well-being, Tan Tock Seng Hospital (TTSH) formalised the Office for the Protection of Employees in 2024, addressing staff abuse cases post-pandemic.
Dr Pauline Yong, TTSH’s director of workplace health and safety, said: “We have clinical protocols to ensure that staff are taken care of (physically), and in terms of emotional support, we have programmes and helplines for our staff’s mental health and in-house counsellors or appointed peers if they need someone to talk to.”
SGH’s Dr Lim said other patients have spoken up for healthcare workers when they see them being abused. He said: “This is tremendously reassuring and empowering for junior staff, particularly before additional help arrives. Written compliments are also incredibly validating for our teams. Where staff do experience significant incidents of abuse, SGH has support structures in place to help them through it, because we recognise that even a single serious experience can have a lasting impact on a healthcare worker’s well-being.”



