ScienceTalk
Cancer patients' Covid-19 dilemma: To jab or not to jab
Sign up now: Get ST's newsletters delivered to your inbox
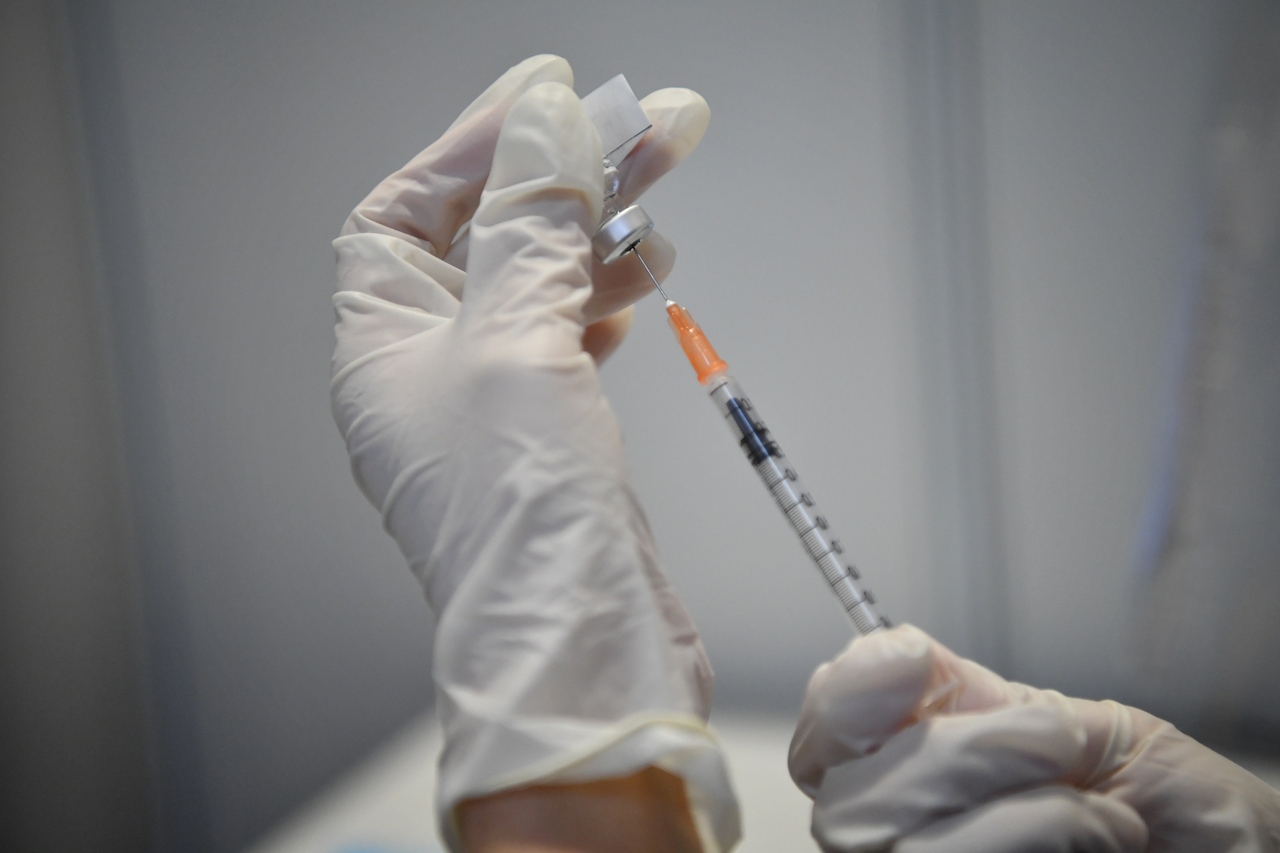
Concerns over a vaccination strategy for cancer patients arise from the fact that they are in a potentially immunocompromised state.
ST PHOTO: CHONG JUN LIANG
These days, many of my cancer patients are engaged in a soliloquy much like Shakespeare's Hamlet: To be, or not to be.
In their case, they ask:
To jab, or not to jab?
Cancer patients are agonising over whether or not to receive the Covid-19 vaccine.
Cancer patients are especially vulnerable to the deadly virus.
Multiple reports in medical literature have documented a higher infection risk as well as probability of developing complications and of mortality in such patients.
Depending on which specific report one is looking at, the mortality rate of cancer patients down with Covid-19 ranges from 5 per cent to 60 per cent, with the median hovering at about 25 per cent.
In comparison, the mortality rate of the general population who contract Covid-19 is 2 per cent to 3 per cent.
Not only are they especially vulnerable to the virus, but coming down with Covid-19 would likely lead to cancer patients pausing, permanently stopping or never starting anti-cancer treatment, inevitably leading to a higher cancer mortality rate down the road.
The motivation to protect cancer patients by vaccination is therefore strong.
The concerns over such a vaccination strategy, however, arise from cancer patients being in a potentially immunocompromised state.
Cancer patients have immune systems that are potentially affected by the condition of cancer or by cancer-related treatment. Hence, cancer patients are often considered a "different breed" when it comes to consideration of the balance between risks and benefits associated with vaccination.
A well-functioning immune system is a sine qua non for vaccination success. The immune cells, in response to stimulation by a vaccine, must respond appropriately by producing the necessary antibodies to neutralise the offending viruses that enter the body.
Cancer, being a rapidly growing group of cells, imposes a huge drain on the nutrients and energy reserves of the body. Normal cells, immune cells included, are therefore relatively deprived of nutrition and often fail to thrive. Cancers that arise from the malignant transformation of white blood cells, these being the immune cells of the system, deal a particularly heavy bodily blow to normal immune response as the immune cells themselves have gone rogue. Leukaemias and lymphomas are such cancers.
Many cancer-related therapies, such as radiotherapy and conventional cytotoxic chemotherapy, while suppressing the growth of cancer cells, inadvertently inhibit the normal multiplication of white blood cells and put the immune system on its back foot.
Cancer patients are therefore counting on doctors and scientists to help them answer three critical questions unique to cancer patients receiving Covid-19 vaccinations: Does it work? Is it safe? Are all cancer patients the same?
In trying to definitively answer the question of whether cancer patients, both on and off treatment, benefit from Covid-19 vaccination, doctors struggle with the problem of paucity of scientific data as these patients did not, by and large, participate in the clinical trials leading to the approval of these vaccines.
Indirect evidence, however, can be gleaned from the decades of experience with flu (influenza) vaccination in cancer patients.
Cancer patients do mount an immune response and produce protective antibodies (a process known as seroconversion) in response to flu vaccination. Ample clinical evidence indicates that the mortality from influenza amongst cancer patients can be decreased substantially with the help of the flu vaccine.
Since direct clinical trial experience of Covid-19 vaccination in cancer patients does not look to be rapidly forthcoming, and faced with the elevated threat that cancer patients have against the coronavirus, it is not beyond the pale to extrapolate from the flu vaccination data and conclude that Covid-19 vaccination is likely to confer protection on cancer patients.
Chemotherapy, in causing a less-than-perfect immune response, will probably lead to some degree of attenuation in the seroconversion and, hence, the protection rate. Cancer immunotherapy and hormonal therapy (also known as endocrine therapy) will likely not have such an effect.
Conceivably, severely immunosuppressive treatments such as stem cell transplant (bone marrow transplant) or treatment directed against antibody-producing immune cells (known as B-cells) will have the most profound impact and substantially water down the vaccine protection rate.
With the exception of patients receiving such treatments, other cancer patients should probably mount a fairly efficient immune response to vaccination.
Given a choice, is there an optimal timing that cancer patients should pick to undergo vaccination? It is probably best to get it done before the commencement of anti-cancer treatment, while the immune system is fairly robust.
The next question is - is it safe?
Currently-developed Covid-19 vaccines are, thankfully from the point of view of cancer patients, not live vaccines.
In general, the use of live vaccines in cancer patients with an impaired immune system is ill advised. Pretty severe infective complications have occurred in the past with the use of BCG (Bacillus Calmette-Guerin) vaccines against tuberculosis in this vulnerable group. Current Covid-19 vaccines in use in the world are either mRNA-based or non-replicating vaccines which are unable to make new viral particles.
Cancer doctors have been experimenting with anti-cancer vaccines that are mRNA-based for over a decade.
While therapeutic success against cancers has yet to be achieved, oncologists at least have gathered from such experiments that mRNA-based vaccines can be safely administered to cancer patients.
Is there a particular vaccine that will suit cancer patients better? From a safety perspective, no. Both mRNA-based and non-replicating vaccines using inactivated viral particles or vectors should be fairly safe.
Finally, we come to the question of whether all cancer patients should be treated the same, or if they should be stratified.
Broadly, we can group cancer patients into an active group still on treatment, a chronic group in remission on a treatment holiday and a survivorship group who are potentially cured of their cancers.
Singapore has adopted an approach of vaccinating the chronic group (with the proviso that they are off treatment for at least 3 months with no plans to start further treatment in another 2 months) and the survivorship group (who are either not on treatment or on only hormonal treatment).
The active group is currently excluded from Singapore's vaccination programme.
This decision is likely made with abundant caution out of concerns over the ability of these patients to mount an immune response to the vaccine and safety issues.
International trends are moving towards vaccination of most, if not all, cancer patients.
The European Society for Medical Oncology gave a call to action to vaccinate all cancer patients. The American Cancer Society wrote an open letter to appeal to the governors of all states in the United States to prioritise the vaccination of cancer patients.
Once our local medical community has gained a sufficient level of comfort over the likelihood of the benefits substantially outweighing the risks of vaccination, Singapore should move quickly towards not only including, but prioritising, all cancer patients in our vaccination program.
• Dr Wong Seng Weng is the medical director and consultant medical oncologist at The Cancer Centre of the Singapore Medical Group. His sub-specialties include breast cancer, lung cancer and gastrointestinal cancers.


