Covid-19: The first 100 days in S'pore
A dinner where death lurked: Couple who became part of Safra Jurong Covid-19 cluster landed in hospital, and survived
Couple who attended became part of Safra Jurong cluster, landed in hospital, but survived
Sign up now: Get ST's newsletters delivered to your inbox

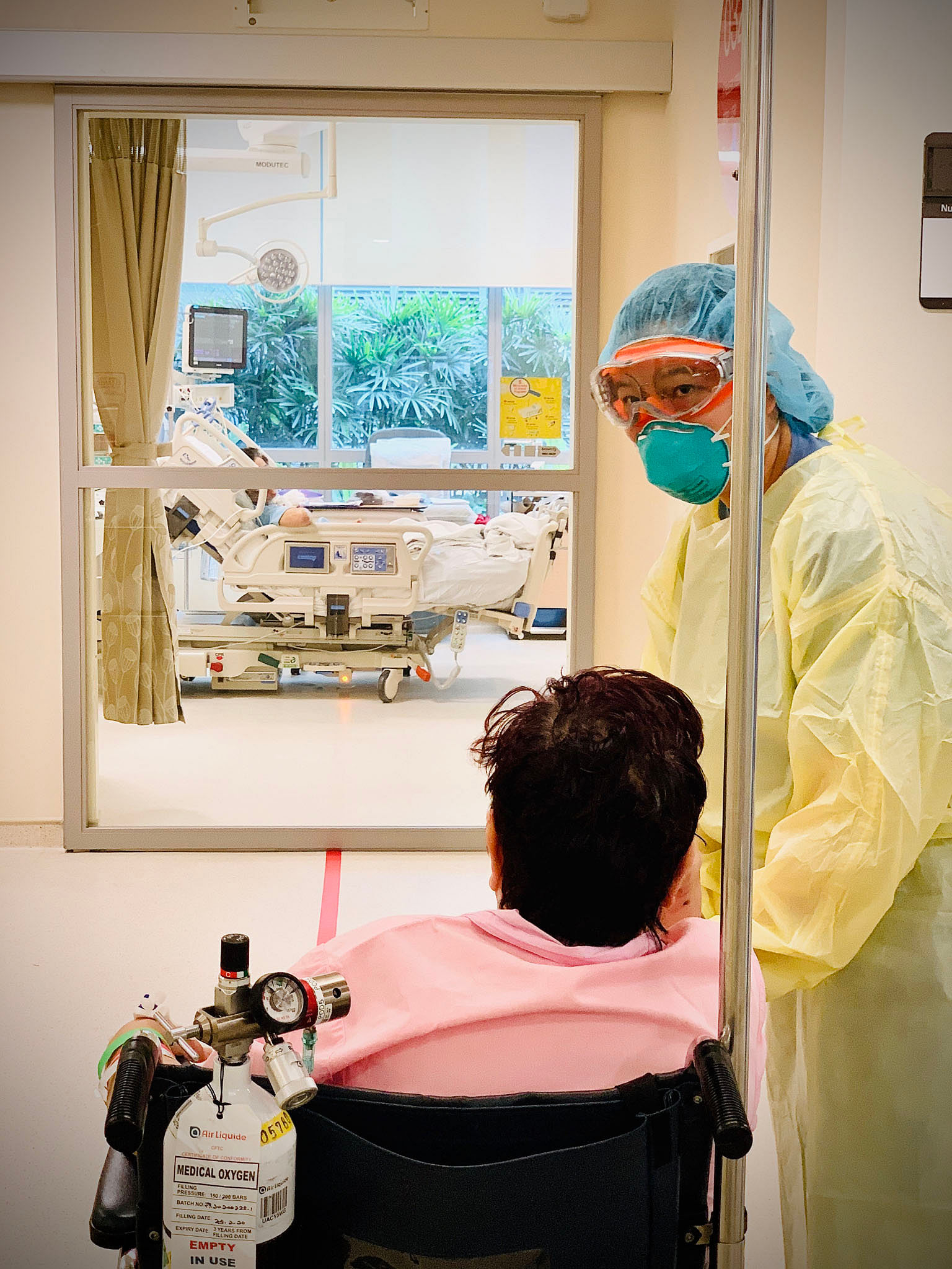
Senior staff nurse Wee Zhen Chian monitoring Mr Tan's condition at Ng Teng Fong General Hospital.
PHOTO: NG TENG FONG GENERAL HOSPITAL
It was a boisterous and lively Chinese New Year dinner that dragged on for five hours, with guests shuttling between tables to chit-chat and pose for wefies with one another, recalls case 130 of a celebration he and his wife attended at Safra Jurong on Feb 15.
"The atmosphere was upbeat and people were happy," the 66-year-old, who would give his name only as Mr Tan, tells The Sunday Times.
The dinner would later be identified as a coronavirus cluster, and was once the nation's largest one with 47 cases linked to it.
Never did the Tans - seated at table 28 - expect it to turn into a nightmare that saw them struggling to survive in the intensive care unit (ICU) and having multiple therapy sessions to relearn how to walk and talk.
But the couple count themselves lucky, as someone at the same function also contracted the coronavirus but never recovered. The 70-year-old man - case 128 - tested positive for the virus on March 6 and died of complications on April 14.
The Tans, who work as food handlers, tested positive for Covid-19 three weeks after the party.
Within days, their lungs became severely inflamed, they were gasping for air and on the verge of dying.
For 31 days, Mr Tan fought for his life in the ICU at Ng Teng Fong General Hospital (NTFGH). He was in hospital for a total of 49 days.
His 68-year-old wife, who is case 129, was at the same hospital for 40 days - 15 in the ICU.
Strangely, no one else in their circle of friends that night was infected, Mr Tan says in Mandarin.
"We were just unlucky. We didn't know there were people who were sick at the dinner."
'WE DIDN'T MINGLE MUCH'
Three years ago, Mr Tan and his wife decided to join a Hokkien singing group led by a music teacher, Ms Liang Fengyi.
Being members of that group, the couple decided to attend the event organised by Ms Liang at Safra Jurong's Joy Garden restaurant, despite being aware of the coronavirus situation.
By then, Singapore had over 70 Covid-19 cases, and had raised its Disease Outbreak Response System Condition (Dorscon) level to orange - the second-highest alert level - for more than a week.
Some 200 guests had to undergo temperature checks before attending the dinner, which featured song-and-dance performances and a traditional lohei tossing. There were an estimated 30 tables.
"We didn't know everyone seated at our table that night," says Mr Tan, adding that he did not notice anyone who was particularly sick.
At their table of 10, the Tans believe they were the only ones who caught the virus. But Mr Tan points out: "We didn't mingle with friends much and didn't move from table to table... but some people did come over to take photos.
"We were also careful not to shake hands, opting to wave instead."
That night, the couple made sure to wash their hands thoroughly when they went to the toilet at the dinner. When they returned home to their Jurong West flat, they headed straight for the shower.
Their music teacher, Ms Liang, was seated at another table and also tested positive for the virus.
Ms Liang tells The Sunday Times that she just wants to move on from the episode. The 56-year-old recovered after 12 days at the National Centre for Infectious Diseases.
The couple do not know the 70-year-old man who died, but Mr Tan says the episode has prompted them to think twice before committing to future social gatherings.
'SMELL OF FOOD MADE ME NAUSEOUS'
Mr Tan was the first to report the onset of symptoms.
It started innocuously enough with a cold on Feb 24. He visited a general practitioner on the same day. On Feb 29 and March 1, he visited the same doctor again after his symptoms did not let up.
Over the next few days, he felt lethargic and did not eat or drink much. His bones and back ached, and he spent most of his time in bed.
"The smell of food made me nauseous," he recollects.
On March 4, a relative took him to the emergency department at NTFGH, where he was admitted.
"When I got there, the staff told me that they would safekeep my bag, wallet and cellphone for me," says Mr Tan, who was drifting in and out of consciousness and could not recall what happened after that.
That evening, a doctor phoned Mrs Tan after suspecting that her husband had the coronavirus and told her to come by for a swab test.
Mrs Tan was later advised to admit herself into the hospital, and she immediately packed her cellphone, charger and a water bottle before an ambulance arrived to pick her up. "I had only one set of clothes - the set I was wearing. It happened quite suddenly," says Mrs Tan, who had earlier gone out to dye her hair and visit the market.
On March 6, both their test results for the virus returned positive.
Their two daughters - who are in their 40s - four grandchildren and a maid who live with them were quarantined. Thankfully, none contracted the virus. Looking back, Mr Tan says: "We were worried that we might have unknowingly passed the virus to those whom we came into contact with."
'I THOUGHT I WOULD DIE'
Mr Tan, who had a fever, was sent to the ICU on March 5 - not long after arriving at the emergency department of NTFGH.
His wife, who was initially asymptomatic, started running a fever two days into admission. She was later transferred to the ICU on March 14, after her condition deteriorated with worsening breathlessness.
Both were in a bad shape when they arrived at the ICU, said members of the critical care team. What they had was acute respiratory distress syndrome, a severe lung condition and a common cause of death in seriously ill Covid-19 cases.
The Tans had entered with alarmingly low oxygen levels in their blood, says Dr Damian Bruce-Hickman, a resident physician at NTFGH.
When they were transferred to the ICU, breathing tubes connected to ventilators were needed to pump enough oxygen into their fragile lungs.
For the next few days, both remained unconscious.
Doctors and nurses, in their cumbersome personal protective equipment, also had to flip the patients face down - in a fairly common intervention known as proning - to boost their oxygen levels.
Dr Bruce-Hickman says: "The second you need extra procedures to protect the lungs, you automatically have quite a high chance of mortality."
When they woke up, the Tans appeared confused and disorientated. At times, they were agitated and did not know where they were.
Because of their weak lungs, it took several phases to slowly reduce the amount of oxygen support and doses of sedative drugs they were on.
Mr Tan ended up with a tracheostomy - an incision made in the windpipe to help him breathe - on March 19.
"I thought I would die," he admits. "I couldn't talk due to the tracheostomy. I wasn't allowed to drink and was fed through a tube."
For days, he hallucinated and saw images that looked like viruses on the ceiling of his room. "I felt like I was in a dream," he adds.
All he could recall then were brief and hazy encounters of nurses asking him how he was feeling.

It was also those nurses who helped him put together what had happened. One piece of news, though, was especially heartrending - his wife was also battling Covid-19 in the next ICU room.
The days after felt like the longest for the couple, who temporarily lost some of their body functions.
Even standing up from their beds felt like an uphill task.
"My head would spin and I felt dizzy. The first time the therapist asked me to try, I struggled," says Mr Tan, adding that he managed to do so the next day with much effort.
The Tans were classified as having "fall risk", and had to get help for simple things such as going to the toilet.
Ms Alaine Teu, a senior staff nurse at the hospital, says with prolonged bed rest, the Tans' muscles got weaker. "So it is more difficult to get out of bed by themselves, to stand up and to walk," she adds.
After the tracheostomy, Mr Tan could not speak much as air would bypass his vocal cords, and he had to rely on a writing board to express himself.
"They made me write English letters and I got the capital and small letters mixed up. I couldn't quite hold the pen steady," he adds.
A simple task like drinking water was also not possible, as it could go down his lungs.
Throughout their ordeal, the love the couple shared was strong.
Ms Teu recounts an occasion when the couple finally got to see each other through their mobile screens, she says.
"Mrs Tan was very cheerful when she saw her husband."
Mr Tan, on the other hand, appeared emotional. "When they did the video call, though he wasn't able to talk much, he kept telling Mrs Tan to jia you," recalls Ms Teu, referring to the Mandarin term to not give up.
When Mrs Tan was well enough to be transferred out of the ICU on March 29, she was taken to see her husband - but from a distance, says Ms Teu. "They weren't able to meet each other physically, but they waved from outside the door."
RELEARNING HOW TO WALK, TALK
Such moments kept them going.
On April 4, Mr Tan had his tracheostomy tube removed. By then, he had not drunk any water for more than two weeks.
That day, he was given a cup with 10ml of water, after which he told the doctor "this is the best-tasting water in the world", shares Mr Tan, who left the ICU on April 5.
Gradually, he became more aware of his surroundings and received help from speech therapists to move air from the lungs past the vocal cords so he could phonate. One exercise he had to do was talk for an hour to boost his stamina.
The Tans were also put through physiotherapy sessions, which involved standing up from their beds and doing exercises in the garden.
"I wanted to get out of the hospital fast and made a point to work hard," reveals Mrs Tan, who returned to the general ward on March 29.
Both husband and wife were breathing on their own when they moved to the general ward, but still needed oxygen supplementation.
The ordeal has drawn the Tan family even closer, shared Mr Tan, who would check on his wife on WhatsApp when they were staying in separate isolation rooms.
The couple would chat with their daughters and grandchildren - aged between 11 and 20 - via a video call almost daily.
The Tans, who still have to go for follow-up appointments, thanked the medical team for risking their lives to care for them - even quashing doubts about themselves.
For instance, Mrs Tan's therapists would continually push her during their sessions together so she could see improvements, she shares. "They were tough on me, but they did so as they wanted me to recover quickly."
Mr Tan, too, recounts how a nurse came back on his day off with tau huay (soya beancurd) because he had mentioned that he missed the dessert. "We received thoughtful care from all those we met," he says.
Mr Tan spent a total of 49 days in NTFGH and was discharged on April 23. His wife left the hospital on April 14, after 40 days there.
But their ordeal is far from over. Both of them are still suffering from after-effects, including poor sleep.
Mrs Tan occasionally has headaches and gets only about five hours of sleep nightly. Her husband would still get breathless at times.
Since leaving NTFGH, they have been doing their prescribed exercises religiously. But they will not be leaving home any time soon.
Their children buy them groceries, which are left at the door, and their maid cooks the meals, says Mr Tan, whose gait is not as steady as before. "It is better this way."
If there is a silver lining, the Tans, who work at Jurong Port Road Food Centre, are thinking of retiring and enjoying their golden years.
Mr Tan admits that they had no idea that one dinner in February would change their lives.
But he adds: "We are very lucky to be alive and to have survived."


