10 suspected cases of blood clot in brain among those who received mRNA Covid-19 vaccines in S'pore
Sign up now: Get ST's newsletters delivered to your inbox
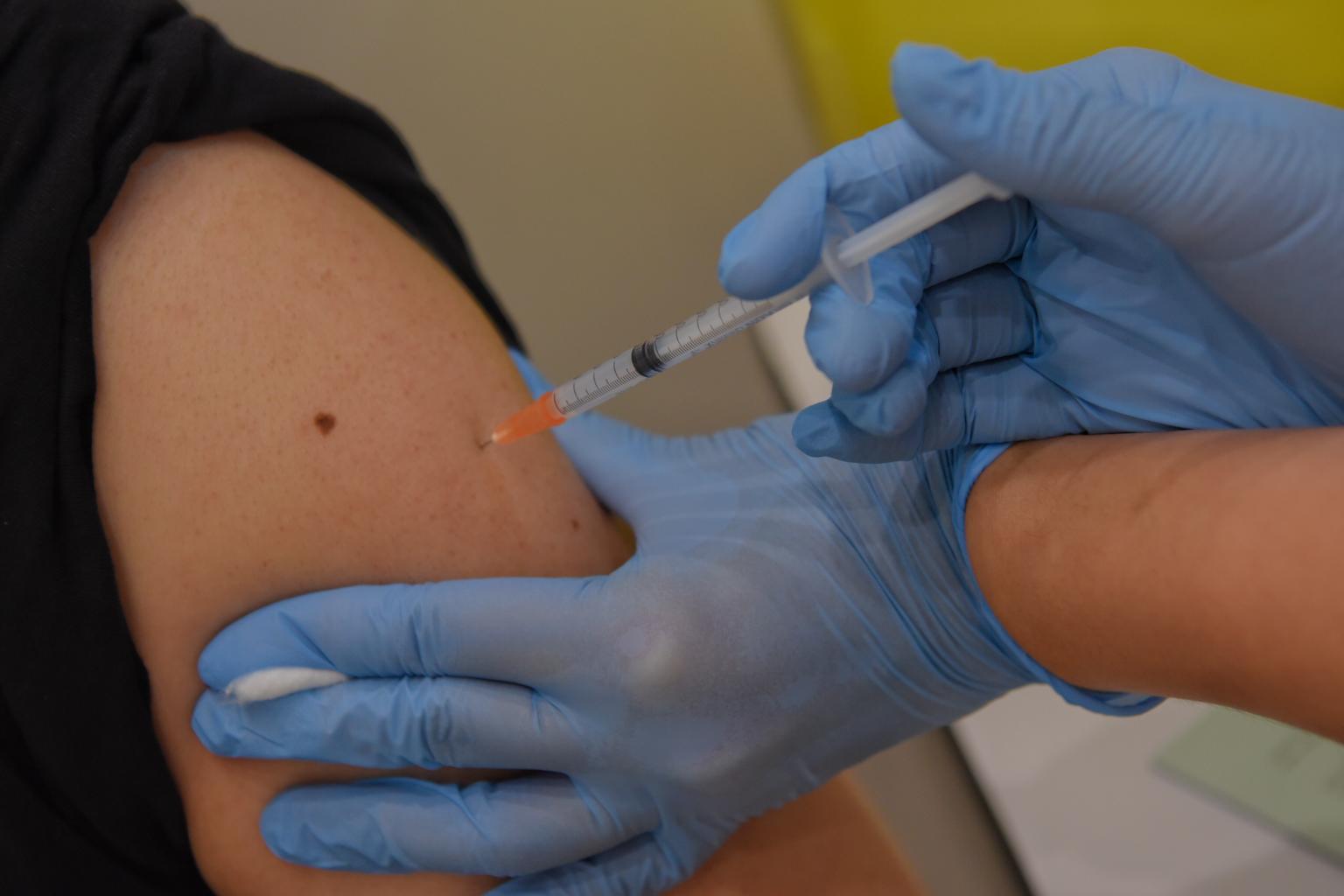
Among the suspected cases of vaccine-related blood clots, HSA noted that none was fatal.
PHOTO: ST FILE
SINGAPORE - There are 10 suspected cases of cerebral venous thrombosis (CVT), or blood clot in the brain, among those who have received the Pfizer and Moderna vaccines for Covid-19 in Singapore.
CVT is a very rare type of blood clot occurring in the veins of the brain, which can happen naturally regardless of vaccination. There are risk factors and these include a medical history of blood clotting disorder, head trauma and the use of medications such as oral contraceptives and drugs for hormonal replacement therapy.
The yearly background incidence rate of CVT in the general population is 1.3 to 2 in 100,000 people, said the Health Sciences Authority (HSA) in its fifth safety update of Covid-19 vaccines.
Among the suspected cases of vaccine-related CVT, HSA noted that none was fatal. It also cannot be determined if there is an increased rate of CVT associated with the use of mRNA vaccines, said HSA.
The authority is monitoring such occurrences closely and reviewing the reported cases with local expert panels, though it noted that no overseas regulators have identified CVT as a safety signal of mRNA vaccines.
According to a recent large cohort study conducted in the United States and published in the medical journal The Lancet, it was found that the incidence rate of CVT in people who received an mRNA vaccine is comparable with the baseline rate of CVT among its population. This means that both the Pfizer and Moderna vaccines are not associated with an increased rate of CVT.
Meanwhile, in another large cohort study in the UK, it was concluded that the risk of most blood clotting events was substantially higher after a Covid-19 infection compared with after vaccination.
The HSA update reported that CVT has been associated with Covid-19 infection at an incidence rate of 8.4 cases per 100,000 infections in a local study. This is higher than the rate among those who have been vaccinated.
Assistant Professor Christine Cheung from the Nanyang Technological University's Lee Kong Chian School of Medicine told The Straits Times that aside from blood clots occurring in the brain post-vaccination, rare clots have also been found in other areas, such as large veins in the abdomen, as well as in some arteries carrying oxygenated blood from the heart to various organs.
Among those who had blood clots post-vaccination, most had a low number of platelets.
"This is ironic, as these are blood cells that normally prevent bleeding by forming clots," said Dr Cheung.
"What was found instead was that patients had a particular antibody that can activate platelets and cause them to mistakenly clump together, in turn clogging up important blood vessels. The actual trigger for the production of such antibodies is still uncertain," she said.
HSA data has also shown that the CVT cases reported locally are not associated with thrombocytopenia, or low platelet levels, and are different compared with the overseas cases of CVT with thrombocytopenia occurring in people who received the AstraZeneca and Janssen (Johnson & Johnson) vaccines.
Dr Cheung pointed out that there were fewer reports of CVT arising from the mRNA vaccines compared with the AstraZeneca and Janssen vaccines.
Both a Covid-19 infection and immunisation with mRNA vaccines can induce certain levels of virus-specific T-cell responses, said Dr Cheung.
T-cells are responsible for killing virus-infected cells.
In healthy individuals, the blood vessel lining is made of healthy endothelial cells that are more resistant to inflammatory insults and are better at escaping the destructive action of T-cells.
However, a Covid-19 infection is thought to inflict damage on blood vessels, resulting in greater susceptibility to blood clotting issues, said Dr Cheung.
A local peer-reviewed study, conducted by researchers from Tan Tock Seng Hospital, the National Neuroscience Institute and Khoo Teck Puat Hospital, found that three people had suffered from CVT after receiving the second dose of the Pfizer-BioNTech vaccine.
It was published in the American Journal Of Hematology on June 16.
They were aged between 54 and 62 years old, with symptoms including headache, vomiting and stroke-like traits such as numbness on one side of the body.
Two of the patients experienced haemorrhage, or bleeding, in the brain.
All three were treated with anticoagulant medications and blood thinners to reduce clotting.


