Fear and shame surrounding sexual health means many suffer in silence, say experts
Sign up now: Get ST's newsletters delivered to your inbox

Experts say many misconceptions about sexual health arise due to social conservatism and discomfort with discussing such deeply personal issues.
PHOTO: ADOBE STOCK
- Sexual health in Singapore is hampered by shame and taboo, leading to patient embarrassment and reluctance to seek help, despite privacy concerns.
- Services like anonymous testing and telemedicine are increasingly popular, addressing privacy concerns and lowering barriers for patients seeking help.
- Significant knowledge gaps persist in female and male sexual health, with many unaware of symptoms or risk, often viewing issues as personal failings.
AI generated
SINGAPORE – Shame and taboo revolving around sex undermines public awareness and open conversation about a variety of sexual health issues, from sexually transmitted diseases (STDs) to reproductive health, experts tell The Straits Times.
“Patients are understandably embarrassed,” says Dr Tan Kok Kuan. “I have had many patients begin their consult by saying, ‘I don’t know where to start.’”
He adds, referring to patients who seek assistance with sexual dysfunction: “And this is them having already overcome their fear of setting up the appointment and turning up at my clinic.”
The clinician, who operates out of Dr Tan Medical Centre in Novena, has spent more than 15 years treating men’s health and STD issues.
He is one of eight experts speaking to ST on what to know about sexual health and testing, and the common misconceptions surrounding it.
Patients’ feelings of shame and fear, as well as concerns over privacy, have fuelled demand for anonymous testing provided by charities in Singapore such as Action for Aids, and private operators like DTAP Clinics Singapore.
Dr Jonathan Ti, DTAP’s chief medical officer, says it performs 200 to 250 rapid HIV (human immunodeficiency virus) tests each month across its seven branches, as well as 150 to 200 rapid chlamydia and gonorrhoea tests monthly.
DTAP was among the first here to offer rapid point-of-care STD testing, says Dr Ti. When it began offering HIV and syphilis tests in 2005 at a now-defunct clinic in Robertson Walk, it was one of the first anonymous testing sites designated by the Ministry of Health (MOH).
The rise of more clinics offering such services over the years means that DTAP’s figures only scratch the surface of the increased demand for testing, he adds.
DTAP grew from just three clinics in 2017 to five clinics with doctors as well as two express self-testing branches.
For thorny issues surrounding sexual health, telemedicine providers like Noah and &Sons have emerged.
Noah says it has served more than 75,000 customers in Singapore since it launched in 2020. Many of these customers seek prescription medications for erectile dysfunction or premature ejaculation.
How often should I get tested?
Testing for STDs is as easy as a needle prick to draw blood (if testing for HIV or syphilis) and swabs at the relevant sites, such as the mouth (if testing for chlamydia or gonorrhoea).
Self-testing kits for HIV are now also available at authorised pharmacies at $28.50.
At the Department of Sexually Transmitted Infections Control (DSC) Clinic, where the cost of testing is subsidised, a chlamydia and gonorrhoea polymerase chain reaction test costs $61.55 for each site tested, excluding the cost of a doctor’s consultation, if necessary.
At private clinics, the cost can be more than $400 for a full panel of HIV, syphilis, gonorrhoea and chlamydia tests, especially for those seeking next-day results.
While the testing process typically takes less than 30 minutes – with many HIV tests now offering same-day results – misconceptions around sexual health and the cost of treatment mean that many do not get tested.
Such misconceptions include patients underestimating their level of risk, believing that a lack of symptoms means they are safe, or that oral sex does not spread STDs.
Dr Benson Yeo, head of DSC Clinic, says: “Many individuals are unaware that the pharynx is an important site for gonorrhoea infection and a recognised reservoir for the development of antimicrobial resistance.”
Says Dr Tham Sai Meng, a consultant at the National University Hospital’s (NUH) division of infectious diseases: “Many STDs, including HIV, syphilis and chlamydia, can be asymptomatic for long periods. Some infections may persist or remain dormant for many years without obvious signs.”
Another misconception is the belief that HIV can be transmitted outside of sexual contact and by exchanging needles, which contributes to the persistent stigma faced by those living with the condition.
Many are also unaware of when or how often they should be tested.
This is a question without an exact and uniform answer because the level of risk varies by individual. This issue is compounded by many patients’ reluctance to be open and honest with their physicians about their concerns, say experts.
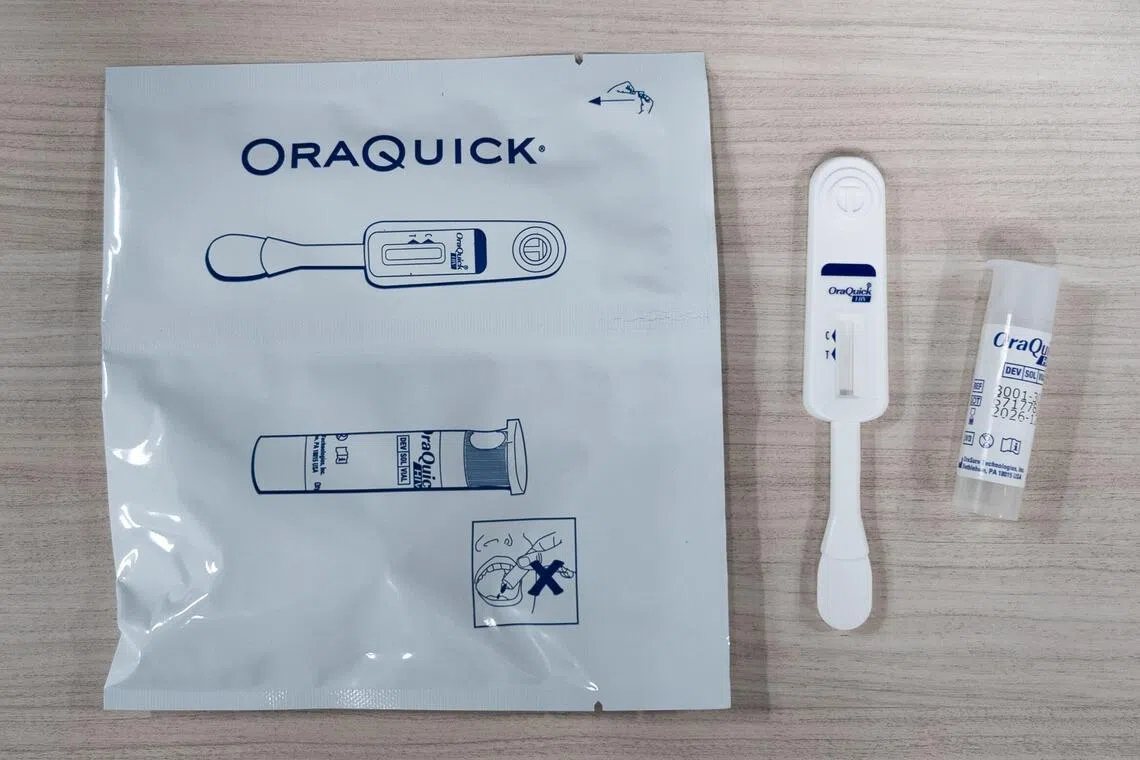
HIV self-testing kits are available at authorised pharmacies.
PHOTO: MINISTRY OF HEALTH
The National HIV Programme recommends that all sexually active adults aged 21 and above get tested at least once in their lifetime, except for females over the age of 65. It also recommends that high-risk individuals get tested every three to 12 months.
Says Dr Tan: “A general recommendation would be to screen annually for sexually active adults and to screen more frequently for people in high-risk groups.”
Dr Yeo says sexual health knowledge varies greatly across communities. Some, such as segments of the LGBTQ community, have longstanding peer-led education and outreach.
“Other populations are harder to reach due to the absence of consistent communication channels or organised community networks,” he adds. With limited open discussion, this can lead to individuals relying on assumptions rather than evidence when assessing their own risk.
How private is treatment?
Part of the demand for anonymised testing is fuelled by concerns over staining one’s medical records. Singapore’s National Electronic Health Record (NEHR) shares some patient information across participating healthcare institutions.
Responding to MPs who aired their concerns in Parliament over the confidentiality of sensitive health data stored in the NEHR, Senior Minister of State for Health Tan Kiat How said in January that there are additional safeguards in place for sensitive data relating to STD infection. These include restricting access to only the healthcare providers directly involved in caring for the patient with the condition.
Dr Tan Kok Kuan says: “The fact is, the patient’s information is protected and kept highly confidential, and this is not only protected by our laws, but also sacrosanct.”
He adds that for certain STDs – such as chlamydia, gonorrhoea and syphilis – doctors are not required to provide any identifying information when notifying the MOH of the case.
But for STDs like HIV, doctors provide identifying information like the patient’s name.
While, as at 2015, there is no ban on short-term visitors with HIV entering Singapore, people living with HIV are still prohibited from seeking an entry pass (such as an employment pass or a student pass), with testing typically required when applying for or renewing such passes.
Female sexual health a blind spot
Beyond STDs, one major blind spot comes in the form of female sexual health. About 30 to 50 per cent of women of all ages are estimated to suffer from female sexual dysfunction, such as those related to arousal or pain that causes distress.
A major misconception is that all women experience pain and bleeding when they first start having intercourse, and that this always goes away with time, says Ms Cheong Xinyi, head and principal psychologist of KK Women’s and Children’s Hospital’s (KKH) psychology service.
“While penetrative intercourse may stretch the hymen, this typically does not result in massive bleeding or pain,” she explains.
Rather, women often experience pain due to the anxiety or fear associated with a gap in sexual knowledge. Such pain could also be associated with medical reasons, past negative sexual experiences or relationship difficulties.
Another blind spot relates to the impact of menopause.
The reduction in oestrogen stemming from menopause means that women may require more foreplay and the use of lubrication for arousal and to prevent pain during intercourse, says Dr Tan Tse Yeun, senior consultant at the hospital’s department of reproductive medicine.
A 2024 study of more than 700 Singapore women aged 21 to 45 found that more than half (57 per cent) were not aware of the symptoms of female sexual health issues. A similar rate (54 per cent) reported poor sexual function.
At the same time, only 43 per cent said they would seek medical help if they experienced such issues, and 91 per cent believed that healthcare professionals should initiate discussions of sexual health issues when appropriate.
In the view of KKH specialists Ms Cheong and Dr Tan, this means persistent misconceptions surrounding the impact of menopause on sex and the idea that sexual difficulties always come down to skill or incompatibility, rather than a lack of open communication.
Such issues were what spurred the development of Singapore’s first guidelines on sexual health for women of reproductive age in 2025. The document is aimed at physicians and highlights the persistent under-recognition of female sexual health issues – an initiative that Ms Cheong and Dr Tan contributed to.
Even as many Asian women face knowledge gaps and are reluctant to seek assistance, many healthcare professionals also feel inadequately prepared to tackle these issues, says Dr Tan.
Do online supplements work?
Men, too, face a host of thorny issues, typically revolving around premature ejaculation (PE) and erectile dysfunction (ED). One in three men are estimated to face PE, while the prevalence of ED increases with age, affecting as many as 40 per cent of men in their 40s, says Dr Tan Kok Kuan.
These issues have fuelled a thriving industry of online businesses selling solutions directly to consumers.
Singapore’s largest men’s telehealth provider, Noah, has served more than 75,000 customers in Singapore through prescription medication for ED, alongside other products aimed at men’s health issues, such as hair growth shampoo and testosterone supplements.
“Men generally avoid seeking help – for anything,” says Noah co-founder Sean Low. “Sexual health is seen as a masculinity issue, not a health issue. Society frames ED and PE as personal failings in ‘not being man enough’ rather than as treatable medical conditions.”
Telemedicine providers fill a necessary service gap, says Dr Tan Kok Kuan, by lowering the barriers for patients to seek help and prescription medicines. Many often direct patients who need further assessment to in-person healthcare providers.
When it comes to supplements aimed at improving one’s sexual health, however, he notes: “Most supplements do not have large clinical studies proving their efficacy. However, most supplements are also relatively harmless.”
His approach with patients is to ask them about specific deficiencies they are using supplements for, and encourage them to continue as long as there is no potential for harm or interaction with prescription medicines.
Dr Chia Jun Yang, a consultant at NUH’s department of urology, notes that such providers have raised awareness and improved accessibility on issues that used to be taboo, but cautions that one should ensure supplements are from credible sources and to seek help from professionals with relevant expertise.
The cost of Singapore’s taboo around sex
Experts speaking to ST pin the blame for many of these misconceptions on a culture of social conservatism and discomfort with discussing not only STDs, but also deeply personal issues relating to one’s sexual experiences and reproductive health.
For instance, experts say that a common misconception is that fertility is either solely a female or male issue, when the issue can stem from either half of a couple. One in six couples face infertility issues, according to the World Health Organisation.
Many of these taboos start in the home.
A 2020 survey by the non-profit Association of Women for Action and Research (Aware) and analytics firm Blackbox finds that, of the more than 500 parents surveyed, only 57 per cent were comfortable with discussing sexual health with their children. That figure dropped to 51 and 49 per cent respectively for those comfortable with discussing romantic relationships or sex.
A 2018 study by Aware of almost 800 young people aged 16 to 25 found that for half the questions posted to respondents about sexual health, more than half of those surveyed were unsure of the answer or answered incorrectly.

Experts say a common misconception is that fertility is either solely a female or male issue, when the issue can stem from either half of a couple.
PHOTO: ADOBE STOCK
Ms Cheong says: “A fear of embarrassment often stops women from seeking support from loved ones and treatment from healthcare professionals, making the experience a lonely and fearful one.”
She notes that it often translates to anger and confusion, as women grapple with a sense of failure at being unable to do something which they perceive should come “naturally”.
Similarly, stigma surrounding men’s health issues “keeps men silent, when the reality is, these issues are often linked to stress, lifestyle or underlying cardiovascular or metabolic issues”, says Noah’s Mr Low.
At the heart of it is a commonly held belief that sexual health solely means the absence of disease or dysfunction, says Dr Tham. Sexual health messaging often relies on fear-based approaches, emphasising “high-risk behaviours” and disease prevention.
In reality, sexual health “encompasses positive aspects of sexuality, sexual identity and preferences, as well as having healthy and safe sexual relationships”, he says, adding that there remains limited emphasis on these broader aspects of sexual health.
Dr Tan Tse Yeun adds: “A fulfilling sex life is an important part of health, and sexual satisfaction contributes to overall quality of life.”
Correction note: An earlier version of the story misspelled the name of Dr Tham Sai Meng. This has been corrected. We are sorry for the error.



