Fate of India-made ventilators up in the air as non-invasive treatments become main mode of care
Sign up now: Get insights on Asia's fast-moving developments
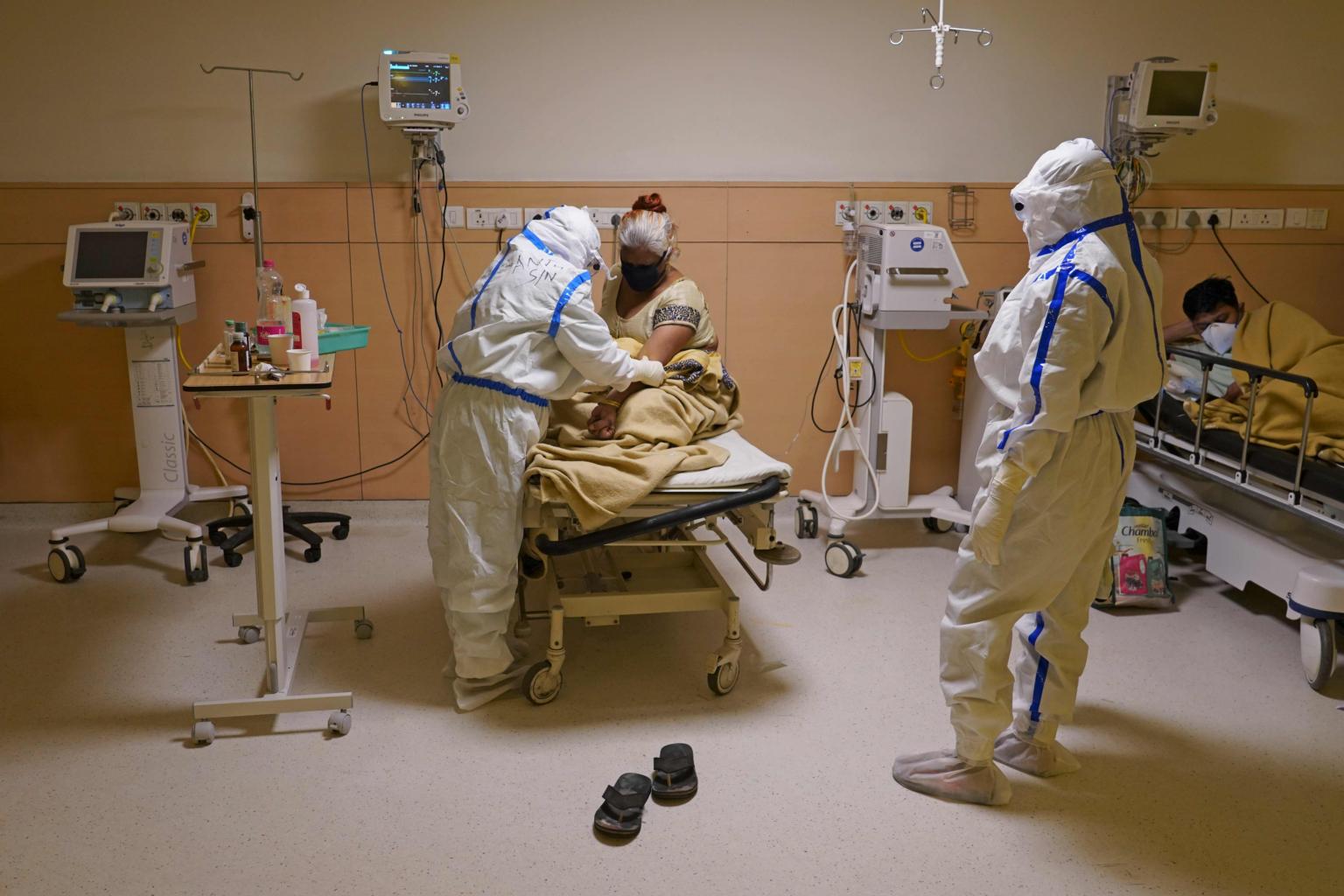
Doctors in four major hospitals had rejected hundreds of the ventilators.
PHOTO: AFP
BANGALORE - Indian-made ventilators are at the centre of a controversy after doctors in four major hospitals rejected hundreds of them as not fit for use for Covid-19 patients last week.
What's more, in the two months that manufacturers had produced thousands of ventilators, it also emerged that ventilators might not be as vital to Covid-19 care as previously thought.
With over 826,000 Covid-19 infections and over 22,600 deaths, India is now the third worst-affected country in the world. When hospitals sounded the alarm that there were only 47,000 existing ventilators in the country, and imports were costly and difficult given global travel restrictions, the government decided to go local.
In May, the Indian government contracted 16 local manufacturers to make 60,000 cost-effective ventilators in two months. It allotted 20 billion rupees (S$372 million) from the PM CARES Fund to purchase these machines. Most of the manufacturers sped up production and cut costs by skipping more advanced features.
Start-up AgVa Healthcare and state-owned Bharat Electronics Ltd or BEL (in collaboration with healthcare company Skanray) received the bulk of the order - 10,000 and 20,000 each respectively.
However, after receiving 175 ventilators funded by the PM CARES fund, the Lok Nayak Jai Prakash Narayan Hospital, Delhi's largest for Covid-19 care, said last week the machines did not have BiPAP, a key non-invasive option to supply oxygen without intubation. Of these, 155 were from BEL and 20 from AgVa.
Most Covid-19 patients in India have needed only non-invasive ventilation and only those with worsening conditions are put on invasive ventilation.
In invasive ventilation, a tube is inserted into the lungs of a patient through the throat, and the machine takes over breathing. The non-invasive technique supplies oxygen through a face mask.
"Mild to moderate cases improve with oxygen therapy or non-invasive ventilation (BiPAP). If the patient is unable to breathe on his own then we intubate. Both methods are important for the management of Covid, but we try a non-invasive method first to prevent any possibility of further damage to the lungs," said Dr Sumit Ray, an intensivist at Delhi's Holy Family Hospital.
A BEL representative The Straits Times contacted for comment did not respond. AgVa said its 20 machines were "not even opened from their boxes" at the Delhi hospital.
That was not all. In May, doctors at the Mumbai-based Sir J J Group of Hospitals complained that AgVa ventilators supplied to them did not have a control knob to set the fraction of inspired oxygen (FiO2). Without this, the doctors would have to manually change the right proportion of oxygen in the air being supplied to the patient and the air pressure at the end of exhalation and inhalation.
Dr Ray, who works in critical care in Delhi, said that being unable to control the oxygen level and pressure at the press of a button could harm a patient: "A ventilator without it is very low-end and it's totally unacceptable."
A report the Mumbai doctors sent to the Director of Medical Education and Research said the AgVa machines weren't able to reach peak targets of oxygen saturation and indicate the actual levels of FiO2 delivered to the patients. Patients who were perspiring and becoming "restless" while using this ventilator showed "immediate signs of improvement" when shifted to other brands of ventilators.
"We are of the opinion that the AgVa ventilators cannot cater to the critical care of Covid patients," the doctors concluded, and returned 81 machines.
Dr Deepak Agarwal, a neurologist and co-inventor of AgVa ventilators, said he stands by their machines: "Someone donated our lower-end model of ventilators to the Mumbai hospitals. These don't have a built-in oxygen blender, but are perfectly suitable for Covid care through intubation. A third-party technician's improper demonstration and installation led to the dissatisfaction of the doctors."
But an official from the Sir JJ Group of Hospitals said their report had brought forth deficiencies that "cannot be simply attributed to improper installation". In a May 26 letter to the medical superintendent, doctors in St George's hospital said an AgVa technician had visited to upgrade the software in some machines, but control settings they needed for oxygen therapy were available only in the next advanced version.
Dr Agarwal said AgVa had already shipped these advanced versions to Mumbai "free of cost", but they were still in the courier office, awaiting a report from the doctors.
"Indian doctors are used to imported high-end ventilators priced at 1.5 to 2 million rupees. Although our ventilator lacks all the bells and whistles, it provides the same core functionalities," he asserted.
AgVa ventilators are priced at 150,000 rupees, a tenth of the imported ones. BEL's machines are priced at 400,000 rupees each.
Dr Jagadish Hiremath, an interventional cardiologist who evaluated the BEL ventilators explained that the non-invasive option (BiPAP) was "a luxury" and not a standard requirement by the technical committee. Including it would have also "prolonged the manufacture while India was panicking about not having enough ventilators," he said.
"A technical reason for deciding against including a non-invasive option is that aerosolisation is very high in BiPAP. (This means) the mask through which the Covid patient gets oxygen has holes from which droplets can get out, increasing the risk of medical staff being infected with coronavirus, especially in modern ICUs that have air-conditioning and no windows," Dr Hiremath added.
The issues have raised questions about what type of ventilators are best suited for Covid care, and if the Indian government overestimated the country's need for them.
Like most at the beginning of the pandemic, India had assumed that ventilators were crucial to save patients with severe illness. But as understanding of Covid-19 evolved, more doctors are using non-invasive techniques.
Health ministry data as on June 23 shows that only 4.16 per cent of Covid infected patients required ventilator support, while about 16 per cent needed oxygen.
"When a person infected with the coronavirus deteriorates, it is not necessarily a problem with the lungs. The blood vessels could be inflamed and the body thinks it's not getting oxygen but the lungs are still compliant. We then need to pump more oxygen and help the patient breathe better," said Dr Lancelot Pinto, a consultant respirologist with Mumbai's Hinduja Hospital.
If a patient came in late with acute respiratory disorder, doctors would immediately intubate him. But Dr Pinto said at least 60-70 per cent of his Covid-19 patients recovered with only non-invasive care.
Intensivist Dr Ray said: "That earlier fear of healthcare staff getting infected through aerosolisation in non-invasive care has decreased now because we know droplets don't reach too far and there's more availability of personal protective gear."
Given the complex decisions they had to make, critical care doctors insisted on ventilators with both invasive and non-invasive options for Covid-19 care. The Indian government's technical specifications also require both types.
The Straits Times could not independently verify the features of the Indian-made ventilators supplied to the hospitals, but thanks to the complaints and rejections, many doctors now worry if the machines are reliable. BEL and AgVa representatives are speaking with the hospitals concerned and exploring upgrades.
Meanwhile, with production underway for 60,000 machines, India's initial alarm about ventilator shortages has now turned into a problem of surplus. Winded Indian manufacturers now hope that foreign markets with shortages will buy their ventilators.
Mr Rajiv Nath, the coordinator of the Association of Indian Medical Device Industry, said: "We have sought lifting of export restrictions."


