The Asian Voice
Build up equitable vaccination practices before the next pandemic: Jakarta Post contributor
The writer says seamless regional and global trade is key to equitable vaccine distribution.
Sign up now: Get insights on Asia's fast-moving developments
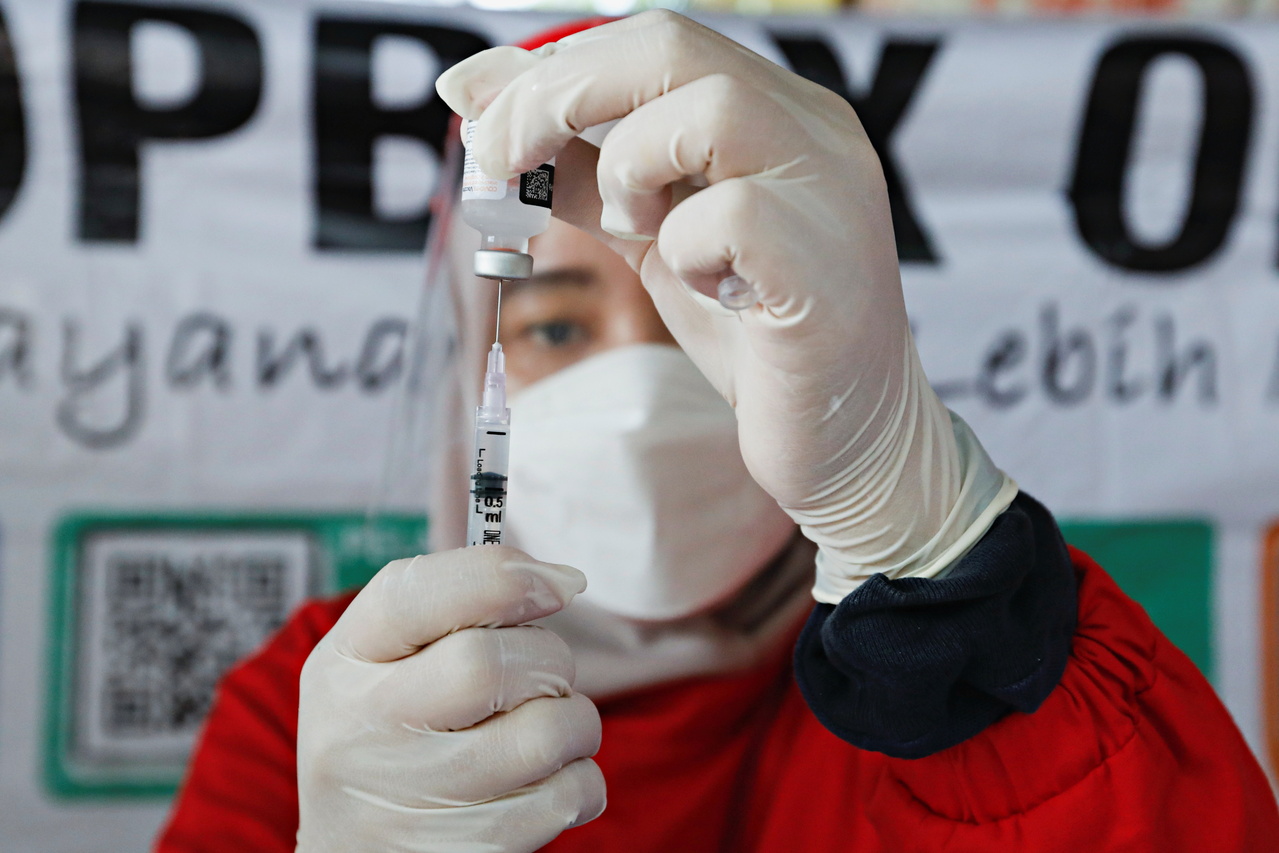
A healthcare worker prepares a dose of China's Sinovac Biotech vaccine against Covid-19 in Jakarta on Dec 10, 2021.
PHOTO: REUTERS
JAKARTA (THE JAKARTA POST/ASIA NEWS NETWORK) -Indonesia's successful Covid-19 vaccination campaign has become a model for the rest of the world.
Today around 98.5 per cent of Indonesians have antibodies against the virus due either to vaccination or past infection. Nearly 100 per cent of eligible Indonesians have received at least one vaccine dose, and 80 per cent at least two, according to the Vaccine Alliance (Gavi), a group that works to promote equitable global access to vaccination.
Still, it took over a year to reach these high levels of vaccine uptake, and other developing nations have not been as successful. Of an estimated 31.4 million potential pandemic deaths in the first year of the global vaccination program, vaccines prevented 20 million.
But many more lives could have been in low-income countries if there had not been delays in getting vaccines to all those who needed them, irrespective of where they lived. We should capture the lessons of this pandemic while they are still fresh - and act now to build equity improvements into pandemic preparedness.
With the recently announced Berlin Declaration, the innovative bio-pharmaceutical industry has set forth a vision for a new social contract for more collaborative and equitable roll-out of vaccines, treatments, and diagnostics.
We are proposing that a tangible way to do so is to ensure vaccines can be distributed and shared real-time to all those who need them. We are calling on world leaders and other key stakeholders to join industry to reach an agreement on how to do this in advance of any future pandemic.
As global health leaders visit Bali for meetings of the Group of 20 Health Working Group on Aug 22-23, Indonesia will have the perfect opportunity for leadership in laying the ground for global solidarity acting in synergy with innovation for the benefit of global health.
From the perspective of someone based in Geneva, Indonesia's vaccine success wasn't a foregone conclusion. Some experts doubted the possibility of vaccinating more than 250 million people - many in rural villages on remote islands. And yet, through careful planning, inventory management, and a key public-private partnership, the country's leaders pulled together a campaign that succeeded brilliantly.
Reproducing this model of success is one of the main goals of the Berlin Declaration. The innovative pharmaceutical industry wants to work with governments to make sure future vaccines don't get stuck on the way to their intended beneficiaries.
Start with innovation. Governments must strive to ensure the conditions that produced Covid-19 vaccines in record time remain in place. What helped speed up the science and delivery of billions of vaccines was a predictable, tried and tested foundation for inventors to share their discoveries with manufacturers worldwide. It eventually led to hundreds of partnerships globally.
Looking to future pandemics, the key objectives are fostering sustainable innovation year on year (since one does not know where the next innovation will come from to tackle a future pandemic), while maintaining the ability to quickly scale up production in geographically diverse areas.
For proven models of partnerships to scale up, manufacturers and governments need only look to the successful voluntary licensing agreements put in place for Covid-19: for example, AstraZeneca's with the biggest Indian generics manufacturer, the Serum Institute; and Pfizer's with the South African vaccine-maker Biovac.
Agreements like these, however, will be significantly less effective if governments impose export bans and other trade barriers, as occurred with Covid-19 vaccines. We cannot afford a repeat of trade barriers stopping the lion's share of vaccines produced in India from reaching Africans. Nor should it be acceptable that rich countries prohibit the trade of products needed to make vaccines in the name of national security - or horde millions of unused vaccine doses, which have a relatively short shelf life, when they are badly needed elsewhere.
Seamless regional and global trade is thus key to equitable vaccine distribution. Countries must work together to remove any bottlenecks.
Finally, governments of developing countries can expedite vaccine equity for their people by availing themselves of resources to create thorough plans for "last mile" vaccine delivery. Every country has unique local concerns that may hinder vaccine uptake even if doses are available. Each state needs a clear plan for delivery.
Global industry can work with governments to put the necessary systems in place to execute those plans. Such planning worked for Indonesia. The government built an app to help assuage vaccine hesitancy and track doses received and administered, enabling officials to identify and prioritise at-risk groups for distribution.
Many leading global health equity organisations support the Berlin Declaration - including Gavi and the Coalition for Epidemic Preparedness Innovations. If they and other backers are able to persuade governments to support it too, the world can then be ready to face the next pandemic not only united but with a clear plan on how it will deliver on the promise of global solidarity.
- The writer is director general of the International Federation of Pharmaceutical Manufacturers and Associations (IFPMA). The Jakarta Post is a member of The Straits Times media partner Asia News Network, an alliance of 22 news media organisations.


