Prostate cancer: Opting for robotic surgery
Sign up now: Get ST's newsletters delivered to your inbox
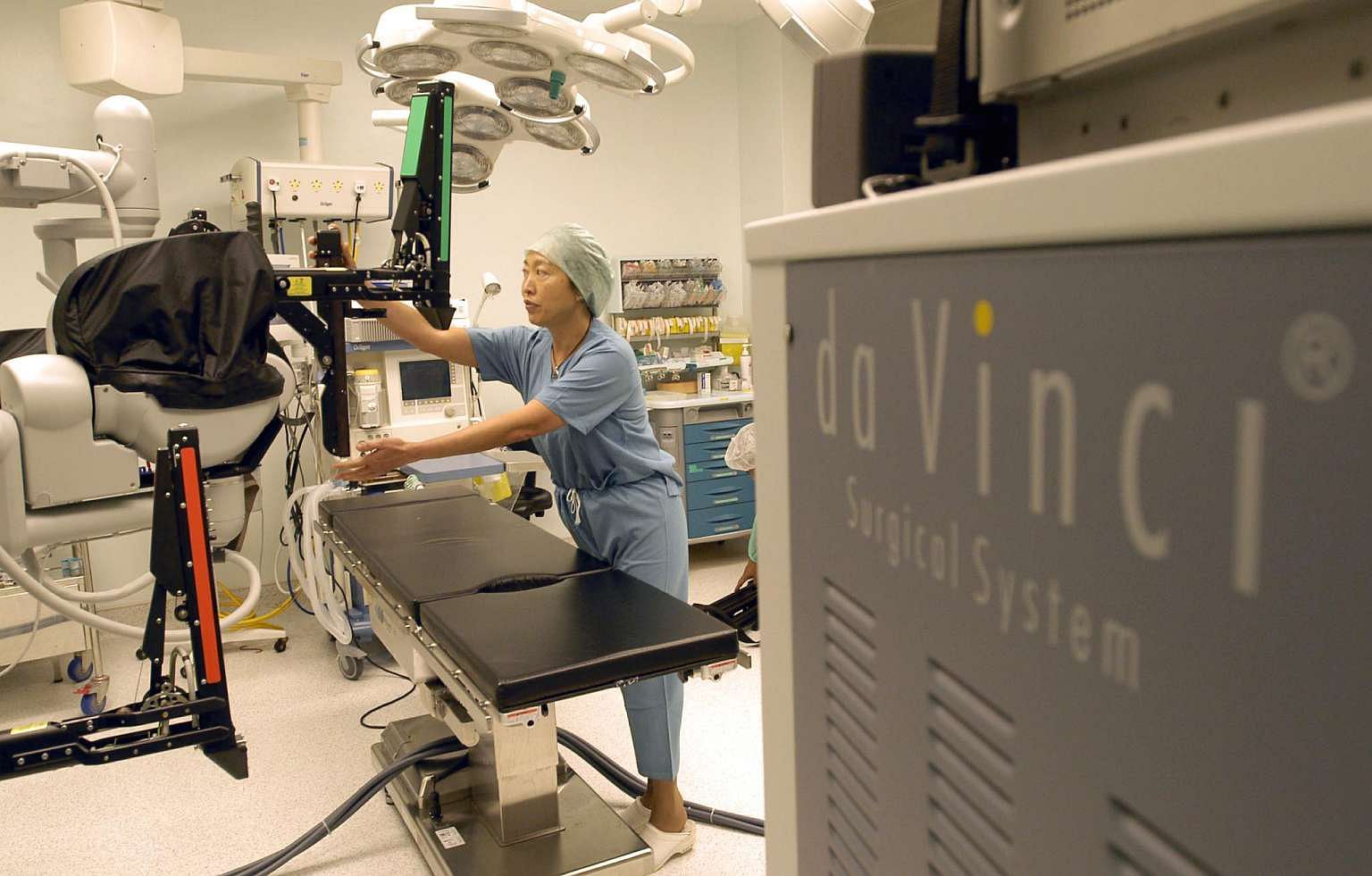
The patient is put under general anesthesia and surgical ports are placed through six keyhole incisions in the abdomen.
PHOTO: ST FILE
What happens during robotic surgery to remove prostate cancer? How long do I have to stay in hospital after the surgery, and will there be side effects from the procedure? My doctor told me that my prostate cancer is more aggressive than usual, and I should consider conventional open surgery or radiation instead.
Can I still be a suitable candidate for robotic surgery?
During robot-assisted surgery to remove the prostate (radical prostatectomy), the patient is put under general anaesthesia and surgical ports are placed through six keyhole incisions in the abdomen, each measuring less than 1cm across. Robotic instruments, including a special camera lens, are inserted into these ports.
The prostate and seminal vesicles, which are a pair of glands that are positioned below the bladder, are removed using the robotic instruments.
This is to ensure that the tissues most likely to harbour cancer cells are removed completely. If the cancer cells have spread outside the prostate gland, they would have most likely reached the seminal vesicles, the vas deferens (tubes carrying sperm from the testicles), and the surrounding lymph nodes.
The bladder is then reattached to the urethra - through which urine flows out - using sutures.
A urinary catheter is left in the bladder for five to seven days to allow urine to drain out of the body while preventing the bladder from filling up, as this may tear the sutures.
In low-risk prostate cancer, surgeons usually attempt to avoid damaging the nerves that control erectile and urinary functions, to facilitate earlier recovery of these vital functions. Those under 65 and who have no other significant health issues, will benefit the most from curative prostate cancer surgery.
Most prostate cancer patients who undergo robotic surgery experience much less bleeding and pain than they would in conventional open surgery.
As the surgical incisions are small, there is usually little pain after the operation, and patients are able to sit up in bed and walk the following day.
Most people are discharged after two or three days. A week after surgery, they return to the clinic or hospital to have the urinary catheter removed. They are usually able to resume most normal daily activities and return to work two to three weeks after the operation.
Some urinary leakage is usually experienced after the catheter is removed, so patients may have to wear pads or diapers till their pelvic floor muscles regain strength.
With improved techniques of robotic surgery, most patients usually recover full urinary control within three to four months.
Erectile dysfunction is another common side effect, due to injury to the nerves during the operation. It tends to take at least nine months to recover from this.
In recent years, many centres have reported positive outcomes after using robotic surgery to treat aggressive prostate cancer, with cancer recurrence rates that are similar to or lower than those who had open surgery.
In such high-risk patients, removing the pelvic lymph nodes helps to reduce the likelihood of the recurrence of cancer.
For those who find that the cancer has spread outside the prostate capsule or involves the attached seminal vesicles, a short course of radiation may be necessary to completely eradicate the cancer cells in the pelvis.


