As men age, something as basic as urination can start to give them problems.
They might have trouble peeing, find the flow to be weak or feel the need to go more frequently. Some might be unable to hold their urine or might have to get up a lot at night.
Such prostate gland issues increase with age - often caused by benign prostatic hyperplasia (BPH), an enlargement of the prostate with age. It is the most common non-cancerous swelling of the prostate.
When urinary problems appear, the first thought for many men is to see a specialist in case they have prostate cancer, said Dr Ng Kok Kit, the vice-president of the Society for Men's Health, who is also a senior consultant and the director of andrology service at Changi General Hospital's urology department.
Prostate cancer is the third most common cancer among men here.
Not many immediately think of consulting their general practitioner (GP). Even those who do so could end up seeking help elsewhere.
"When patients have urinary problems, the GP will refer him to a specialist," said Dr Ng.
"Most doctors are capable of doing rectal exams to check for prostate size and when there is suspicion of prostate cancer, but not all patients are comfortable with it."
Some primary-care doctors are not keen either for various reasons, thinking it is troublesome and dirty, for instance, said Dr Lim Kok Bin, a specialist in urology and a consultant at the Raffles Urology Centre.
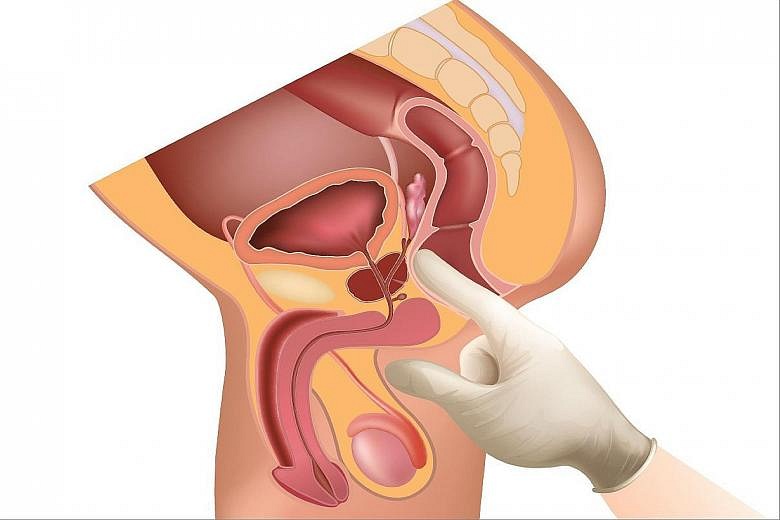
However, a digital rectal examination is exactly what should be done by the GP as part of the assessment for BPH, said Dr Ng. The procedure involves using a gloved, lubricated finger to check for abnormalities.
Indeed, new recommendations for the treatment of prostate problems say GPs should pick up crucial red flags that point to the need for specialist attention, said Dr Ng, who chaired the group that drew up the Better Prostate Health Guidelines.
For example, they should do a rectal exam and a prostate-specific antigen (PSA) blood test to look for prostate cancer.
Developed specially for GPs here, the guidelines were launched on Nov 19 by the Society for Men's Health Singapore.
The previous set of guidelines was issued a decade ago and targeted more at specialists than at GPs.
Since then, new drugs have been introduced to treat prostate problems, and now, the treatment regime can be tailored to match the conditions and needs of different patients, said Dr Ng.
For example, some patients have BPH symptoms as well as sexual dysfunction, which would affect the choice of drugs used, he said.
Some drugs can treat both sexual dysfunction and urinary problems at the same time. Others might be effective for urinary symptoms, but have side effects such as decreased libido and ejaculation problems.
Dr Ng noted that many BPH cases can be treated with medication available from the GP.
Those who are at higher risk of getting prostate cancer can also first see their GP, who can then do a simple blood test to check for PSA, a tumour marker for prostate cancer. It can help to detect the cancer early, but not all prostate cancers require treatment.
"Patients above 50 should discuss with their GPs the pros and cons of prostate screening," said Dr Ng.