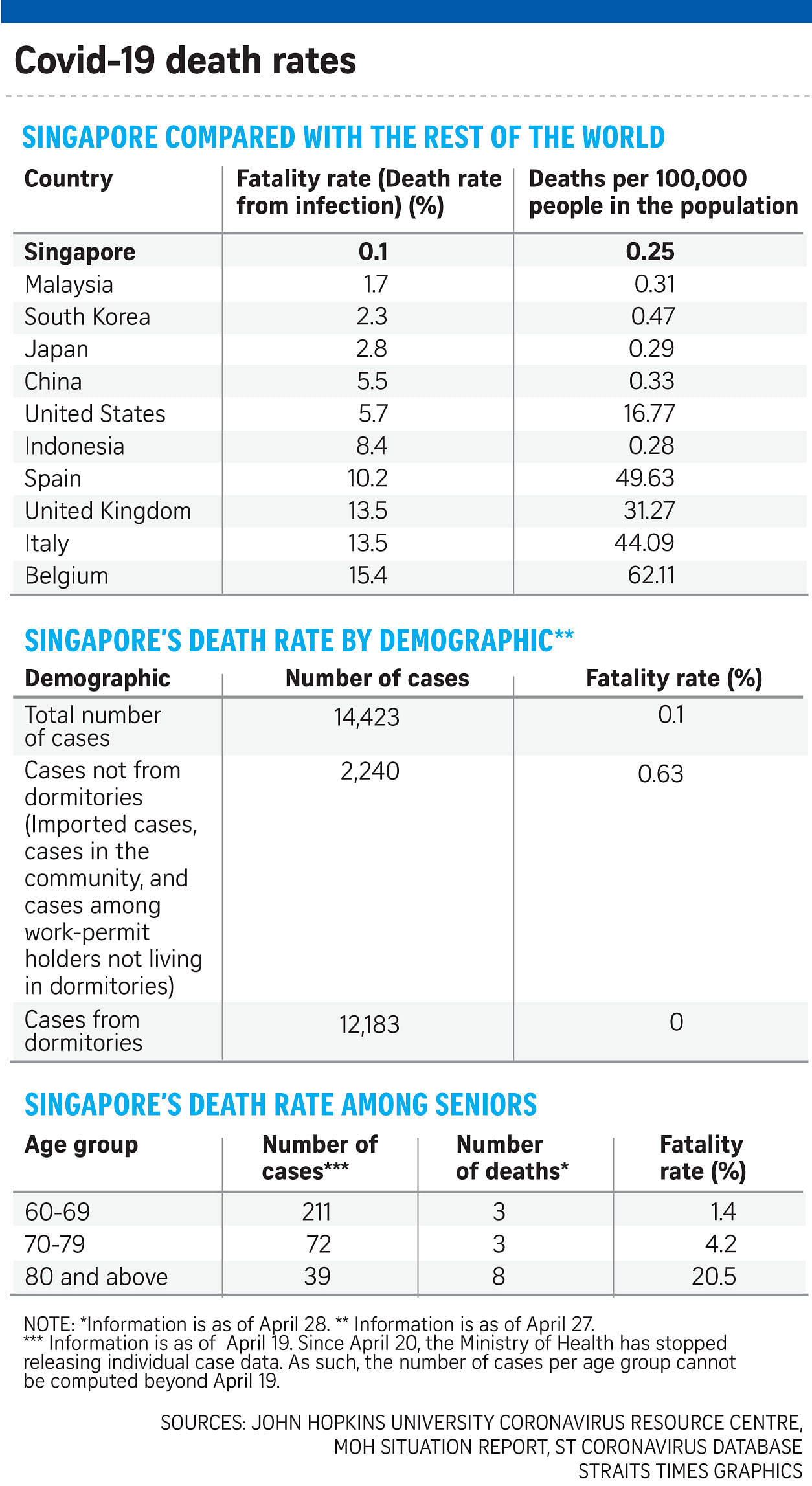
Singapore's Covid-19 death rate is among the world's lowest, with only about 0.1 per cent of patients succumbing to the illness here.
But the figure turns grim when it comes to older patients.
For those who are 80 and older here who tested positive, about one in five has not survived the virus infection.
At least 39 people in this age group have been infected, and eight have died, accounting for more than half of the 14 deaths that Singapore has suffered so far.
In addition, all 14 deaths involved people aged 64 to 95, showing just how vulnerable older people are to the disease.
Dr Sitoh Yih Yiow, a geriatrician at Age-Link Specialist Clinic for Older Persons, said that seniors are at risk because they have a higher chance of developing severe complications from the virus.
This risk stems from several factors, including a weaker immune system, and a higher prevalence of multiple medical conditions such as heart disease, diabetes, hypertension and chronic obstructive lung disease, he pointed out.
"Older persons tend to have diminished physiological reserves, meaning they are less able to accommodate stressors to the body and, hence, succumb more easily," he explained.
In recent weeks, cases among older persons have emerged from nursing homes and homes for the destitute, where residents are even more vulnerable because they live in groups.
On Monday, the Ministry of Social and Family Development announced a new cluster of infections at Acacia Home, a welfare home for the destitute in Admiralty.
Fifteen cases are now linked to the cluster, which comprises 13 residents and two staff.
While the vast majority of the more than 14,000 infected in the country are workers living in dormitories, these individuals are generally young and healthy, with very few needing oxygen or intensive care.
In addition, through extensive contact tracing and ring-fencing efforts, as well as strict circuit breaker measures, Singapore has been able to ensure that intensive care unit (ICU) facilities have the capacity to cope with any patient who needs such treatment.
But cases in nursing homes and other such care facilities could easily flare up.
In Europe and the United States, for example, they were death traps for residents when infections spiralled out of control.
Associate Professor Kenneth Mak, director of medical services at the Ministry of Health, said yesterday that vulnerable groups are identified quickly, before being removed from an environment where they are at an increased risk of being exposed to the virus.
Nonetheless, some will not do as well, may develop complications, end up in the ICU, or even die, he noted.
"It is therefore important for us to keep a close watch, look for people who are deteriorating, get to them as soon as is possible, and look after them as best as we can."