Ng Teng Fong General Hospital pilots system to remotely monitor non-ICU patients on ventilators
Sign up now: Get ST's newsletters delivered to your inbox
Ng Teng Fong General Hospital develops remote monitoring system for a faster response time from medical staff when attending to patients with chronic respiratory conditions.
Yeo Shu Hui
Follow topic:
SINGAPORE - Ng Teng Fong General Hospital has completed a pilot for a new system that allows respiratory therapists to monitor the condition of patients on oxygen therapy via ventilator in its general wards and respond more quickly to any issues.
The idea was sparked by the hospital's intensive care medicine team about 20 months ago, when it saw how the Covid-19 pandemic had severely strained healthcare resources and expertise globally, especially for respiratory-related intensive care services.
Dr Faheem Ahmed Khan, head and senior consultant of the hospital's intensive care medicine team, said: "When we had to evolve our care with the ongoing pandemic, we saw the opportunity to innovate and came up with this unique process using the existing infrastructure and equipment."
The new system mitigates demand on intensive care unit (ICU) manpower and beds during a pandemic, as non-Covid-19 patients who require non-invasive ventilation (NIV) can be moved to general wards. NIV provides patients with pressurised air concentrated with oxygen via masks to help them breathe.
Respiratory therapists, who are usually based in the ICU, can monitor the condition of patients on oxygen therapy via ventilator in its general wards.
Resident physician Nikhil Gautam added: "In the event that there is a big surge (in Covid-19 cases) and all the ICU beds are filled up, this remote monitoring process will give us the confidence and assurance of being able to monitor patients who may require NIV therapy."
The trial - involving 21 patients on NIV - was conducted by Dr Khan, Dr Gautam and head of respiratory therapy Ian Cendana, together with a multi-disciplinary team of respiratory therapists and nurses.
Patients' vitals - such as their pulse rate and oxygen level - and ventilator data are monitored simultaneously. The system triggers an alarm in six pre-determined situations on the ventilator, such as if it detects deterioration in patient conditions or technical issues like "power disconnect" or "oxygen disconnect".
Respiratory therapists would be alerted with an SMS, e-mail and on their computer dashboard. They can remotely review the patient's vital signs and ventilator data, sent to their mobile devices or computers over wireless data transfer, and call the ward nurse to resolve the situation or go to the ward if necessary.
This system enhances patient safety, as it allows early detection of any issues, and also improves operational efficiency at the hospital.
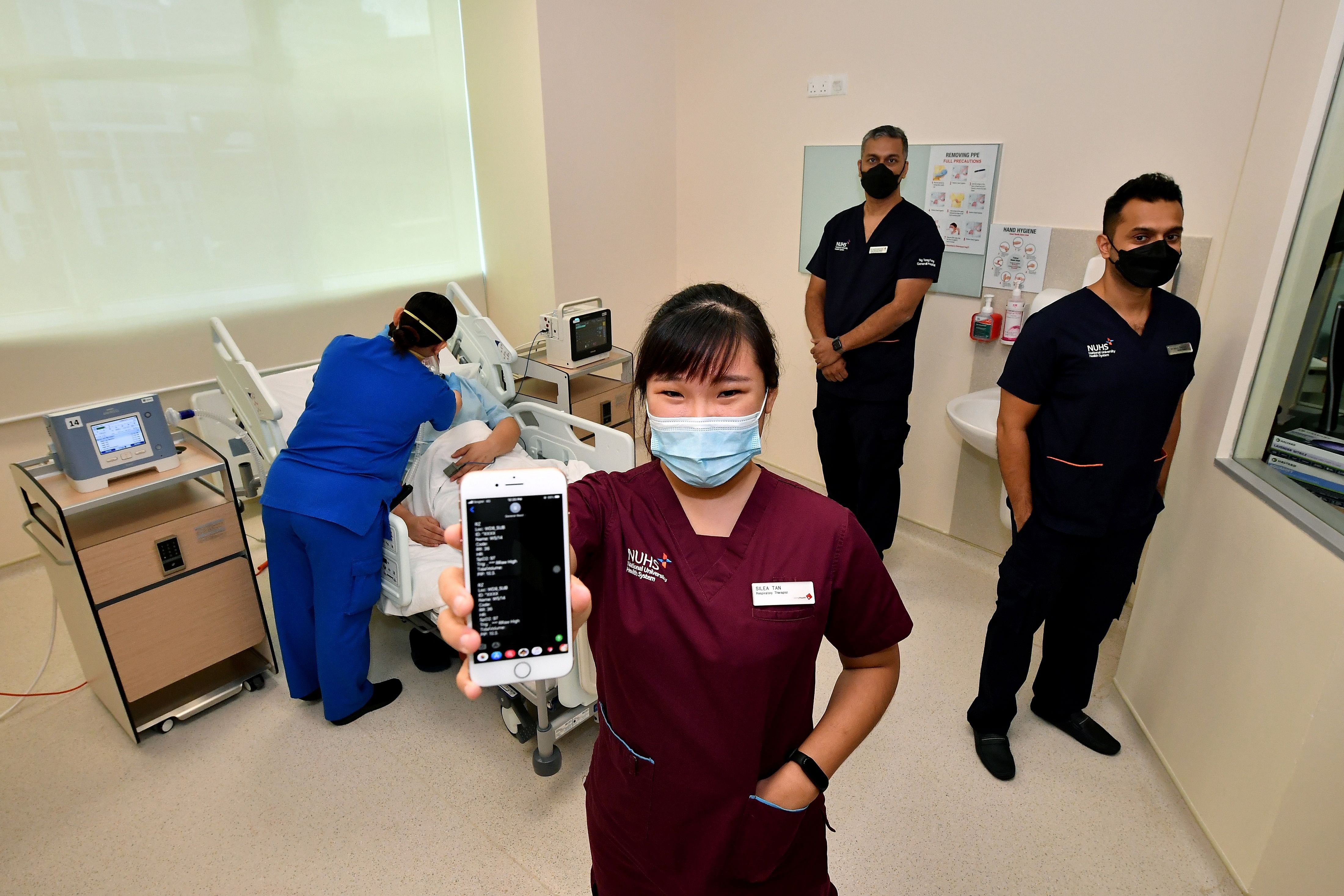
Respiratory therapist Tan Si Lea said that it cut down reaction times from the five to 15 minutes to under two minutes, and also eased respiratory therapists' workloads.
Under current protocols, a general ward nurse who notices any issues has to telephone the respiratory therapist in the ICU, who may then go to the ward to assess the situation and take action. The respiratory therapist may escalate the case to ICU doctors if the patient's condition deteriorates.
The team documented a total of 95 instances where the alarm was triggered, and the subsequent actions taken by the respiratory therapists and nurses.

Respiratory therapists can remotely review the patient’s vital signs and ventilator data, even when on the go.
ST PHOTO: LIM YAOHUI
Among these were seven instances where they captured acutely deteriorating conditions in patients and were able to provide intervention efficiently.
There were also many other episodes where the respiratory therapists were able to detect issues early and prevent the patients' condition from further deteriorating.
The hospital plans to roll out this new system in April next year. In the meantime, the team is moving to the next stage of the trial, to further improve the system, Dr Gautam said.
This includes creating an app to improve the two-way communication between the respiratory therapists and the nurses in the ward. They are also exploring using the monitoring system to track a patient's respiratory rate, and may expand its use to suitable patients in the community.

