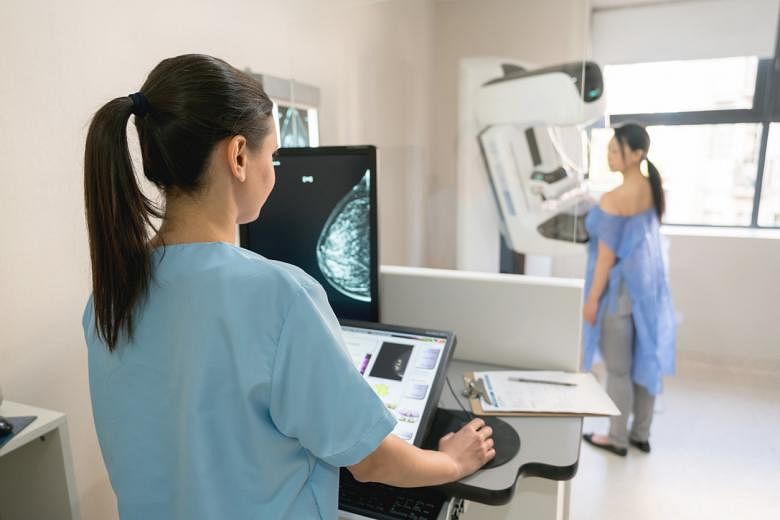
Can exposure to radiation cause breast cancer? Does getting a Pap smear hurt?
When it comes to women's health, there are certain intimate questions that you may be too embarrassed to ask. However, it is important to stay informed so that you are able to make decisions that will help to improve your overall health.
We sit down with doctors from Gleneagles Hospital to get to the bottom of some of your blush-worthy questions.
Breast cancer
According to Dr Andrew Clayton Lee, an oncoplastic breast surgeon at Gleneagles Hospital, breast cancer is becoming more common. Early detection saves lives and treatment may be less intense. Community awareness together with a monthly self-examination and routine breast screening are keys to a better outcome.
Dr Lee addresses key questions that we have about breast cancer screening and prevention.
Q: How often should I go for a mammogram and does it hurt?
A: The guideline is that women between the ages of 40 and 50 should go for a mammogram once a year. Women above the age of 50 should go for mammograms every two years. The screening test is not painful. Ladies with sensitive breasts can consider having their mammograms after their menses when their breasts are less sensitive.
Q: Will exposure to radiation during a mammogram cause breast cancer?
A: People think going for mammograms is dangerous because of the radiation, but the test only involves a very small amount of radiation. It is equivalent to the amount of radiation we get from the sun when we fly from Singapore to London and back five times. No, mammograms do not cause breast cancer.
Q: How can I keep my breasts healthy?
A: Maintain a healthy weight and daily exercise. If you look at all cancers, including cancers of the womb, oesophagus and pancreas, your risk of developing them increases if you are overweight. In addition, avoid daily consumption of alcohol and smoking.
It is also important for ladies to do a self-examination once a month, around seven days after the start of menses for ladies who have menses. For ladies who have past their menopause, any day of the month is good. This may help you to detect the faster growing cancers that can develop in between screening.
HPV and cervical cancer

Many of us know that it is a sexually transmitted infection. However, the truth is that HPV is a lot more common than you think.
To clear up the confusion surrounding HPV, Dr Quek Swee Chong, an obstetrician and gynaecologist at Gleneagles Hospital, weighs in on burning questions and concerns about the viral infection.
Q: Why should I be concerned about HPV?
A:Eight out of 10 men and women would have had contact with HPV in their lifetime. Most HPV infections will go away after a couple of months as the body's immune system is able to get rid of it. Only in a small proportion of cases, the virus stays in the body and causes the cells of the cervix to change.
Q: Will long-term use of contraceptives, like birth control pills and intrauterine devices (IUDs), increase the risk of cervical cancer?
A: Data shows that IUDs do not increase a person's risk of developing cervical cancer. There is some conflicting evidence that shows that being on the pill for a long period of time increases the risk of cervical cancer. The pill itself does not cause cancer but it probably changes the characteristics of the cervix, making it more susceptible to HPV.
Q: How can I reduce my risk of getting cervical cancer?
A: Women should go for yearly Pap smears from the age of 25. If you are aged 30 and above, you should do the HPV test every three to five years in place of a Pap smear. In addition, they should also avail themselves of the HPV vaccine which can dramatically reduce the chances of getting cervical cancer.
Q: Does the HPV test hurt?
A: Undergoing an HPV test is similar to getting a Pap smear. A properly done test is painless and usually completed within one to two minutes. During the test, a small plastic device is inserted through the vagina and to obtain a swab from your cervix. This will be sent to the lab for testing.
Strong bones

According to a study by the International Osteoporosis Foundation, more than 200 million people around the world have osteoporosis. One-third of them are women aged 50 and above. Women who have gone through menopause are more susceptible to osteoporosis because the loss of oestrogen accelerates bone loss.
Dr Lo Ngai Nung, an orthopaedic surgeon at Gleneagles Hospital, talks about preventive measures against the bone disease.
Q: How can I tweak my diet to help fight osteoporosis?
A: There are three things to bear in mind. One is ensuring that you have adequate calcium in your diet. If you have a calcium-deficient diet, buy fortified milk or take supplements.
Next, lead a healthy lifestyle. Avoid excessive smoking and alcohol consumption, and heavy doses of caffeine. Last but not least, you need to stimulate the bones with exercises. If you are going to load up on calcium but just lie in bed, then your bones are not going to get stronger. Some weight-bearing exercises that you can try include brisk walking, dancing and tai chi.
Q: How much calcium is too much?
A: In life, it is all about moderation. You have to look at the patient's dietary requirements and problems. If you are calcium-deficient, you need supplements to keep your calcium levels up.
The recommended calcium intake for healthy adults aged 51 and above 1000mg/day, and 800mg/day for those under 51. If you're young and you go overboard with calcium, then you can run into other issues like kidney stones. Some reports have found that excessive calcium supplements may lead to an increase in heart disease because the calcium could be deposited in the coronary arteries. This is a bit controversial, which is why you have to do things in moderation.
Skin cancer

Skin cancer is one of the top 10 most common cancers in Singapore among both men and women. There are three main types of skin cancers, two of which are not fatal. The third type is melanoma skin cancer, which arises from pigment-producing cells in the skin called melanocytes.
Learn more about the risk factors for skin cancer from Dr Rachael Teo, a dermatologist at Gleneagles Hospital.
Q: Will excessive exposure to sunlight cause melanoma skin cancer?
A: Yes, sun exposure is one of the risk factors of melanoma.
Q: Is sunblock a fail-safe way of preventing skin cancer?
A: Application of sunscreen or sunblock is just one aspect of sun protection. It is not 100 per cent fool-proof. At the same time, try to avoid the sun when its rays are the strongest. This is usually between 10am and 4pm. Cover up by wearing a broad-brimmed hat, sunglasses and long sleeves. Seek the shade if you are able to and remember to reapply sunscreen after 4 hours.
Q: If I am noticing more pigmentation on my face, am I at risk of getting skin cancer?
A: Your risk of getting skin cancer increases if you have very fair skin or have had a lot of sunburns. If you notice pigmented lesions or spots on the face that appear to change with time, then they should be professionally evaluated.