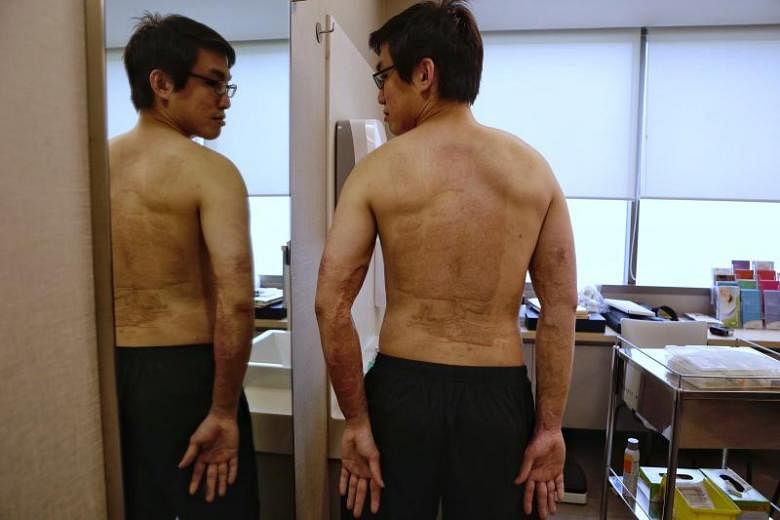
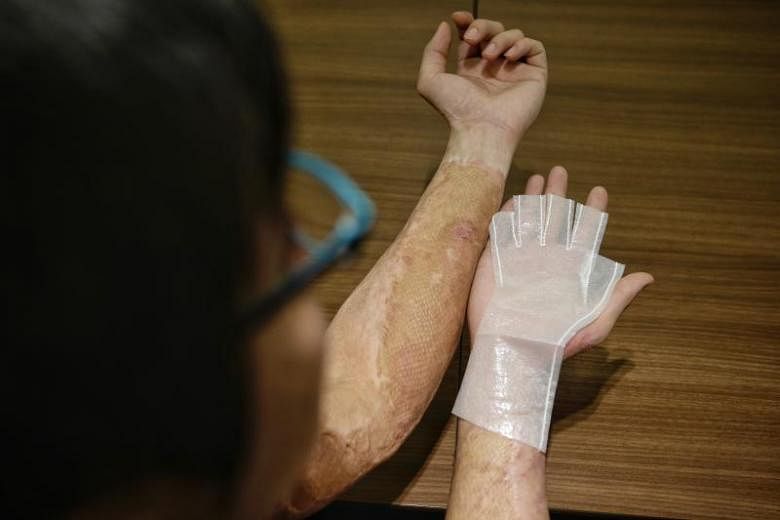
SINGAPORE - Three years ago, Mr Lim Ming Tat, 29, had been pouring fuel as part of his work conducting outdoor activities for schools, when it suddenly caught fire and doused him in flames.
Hours later, he underwent surgery where doctors used artificial skin instead of conventional wound dressing, and a recently adopted skin-grafting method to treat the burns, which covered two-thirds of his body.
Thanks to the new modes of treatment, Mr Lim needed to have only eight operations instead of more than 20, and stayed in the hospital for one a half months, versus the usual five.
These methods became routine at the Singapore General Hospital's (SGH) Burns Centre in July 2014, after small-scale studies proved their effectiveness.
Together with ensuring that patients undergo surgery within 24 hours, the new protocol have reduced deaths of burns patients from 2.7 per cent during 2011-2013, to less than 0.5 per cent between 2016 and last year.
The patients' hospital stays, which averaged 13 days, were also four days shorter than those who were treated before the changes were introduced.
In addition, infection rates were down by 70 per cent after doctors adopted the newer methods, according to the findings of a two-year SGH study on 250 patientsreleased today (March 23).
SGH runs the only specialised burns centre in Singapore, managing 93 per cent of adult burns patients here. It sees an average of 220 inpatients each year, and is the major burns referral centre for South-east Asia.
The skin grafting method used for major burns, which is called micro-grafting, has also cut back on the usage of donated skin by two-thirds - a boon for the local skin bank, which receives only around 20 skin donations a year, said Assistant Professor Si Jack Chong, a consultant at SGH's department of plastics, reconstruction and aesthetic surgery, who also led the development of the new treatment protocol.
Micro-grafting involves cutting undamaged skin from the patient and arranging it onto donated skin, which is then used to cover the patient's burn wounds and stimulate skin growth. However, it leaves a chequerboard appearance as the skin heals.
Previously, unmodified donated skin would be used to temporarily cover the wound. This donor skin would then be replaced, bit by bit, with the donor's own skin. This is a more painful process that had to be repeated as many as 20 times, he added.
"In the past, we had to buy a little bit (of donated skin) from overseas...(but) over the last few years our (local) stockpile has really gone up, so Singapore can manage a significant amount of big burns casualty," said Prof Chong of the micro-grafting process.
Meanwhile, the other new protocol of using artificial skin helps to reduce pain for patients. The artificial skin, which is made of silicone, collagen and nylon, also allows patients' wounds to be monitored more easily. And because it does not need to be changed, but rather, drops off after nine to 14 days when the skin has healed, fewer changes of wound dressing are needed.
Mr Lim, whose front torso, arms and legs were badly burnt, took one year to recover and move normally again. He said he is grateful for the shorter and less painful treatment period and it had allowed him return to his some of his favourite outdoor activities more quickly.
He plans to start scuba diving again in a year, but has to take care from being under the sun for too long in case his skin blisters.
Said Mr Lim, who works part-time: "Life is not as perfect as before, but I can still do most things that I did previously."