SINGAPORE - Infectious disease doctors in Singapore are cautiously optimistic that an old and cheap steroid drug can cut Covid-19 deaths by a third, based on early results from a British study.
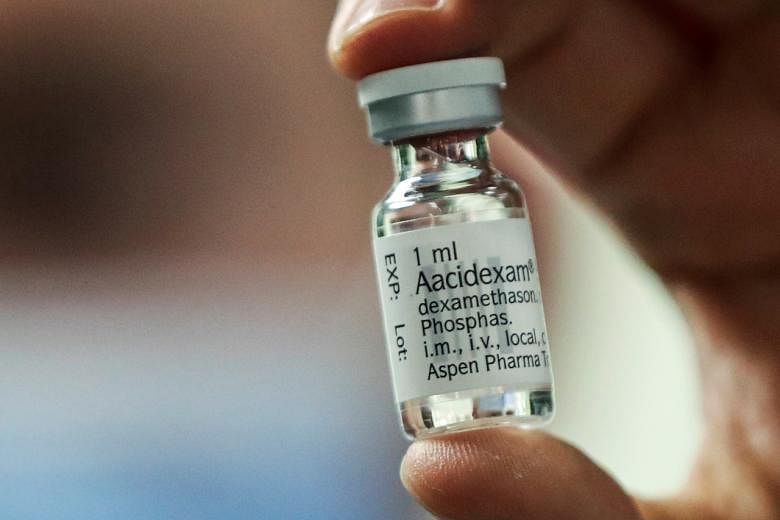
A team from Oxford University had given the steroid drug, dexamethasone, to more than 2,000 patients and compared their outcome with over 4,000 patients who were not given the drug.
The risk of death for patients on ventilators, which is used to help them breathe, was cut from 40 per cent to 28 per cent after they were put on the steroid for 10 days.
The team's chief investigator Professor Peter Horby told the BBC: "This is the only drug so far that has been shown to reduce mortality - and it reduces it significantly. It's a major breakthrough."
The team said it was particularly effective for those who are seriously ill, and claim it can save the lives of one out of eight patients who are on ventilators, and one out of 20 to 25 who need to be given oxygen.
Prof Horby added that the benefit is clear for patients who are sick enough to require oxygen treatment, "so dexamethasone should now become standard of care in these patients".
But it does not help patients who do not have difficulty breathing.
Experts here say they need to see the full results of the study, though Associate Professor Hsu Liyang, an infectious disease specialist and epidemiologist at the NUS Saw Swee Hock School of Public Health said there is "biological plausibility" that the drug can help seriously ill Covid-19 patients.
He said it "only appears to work on those who are more ill, which is consistent with its mechanism of action of suppressing the immune system. In many cases, the deterioration in Covid-19 is due to immune system overdrive".
Dr Asok Kurup, who chairs the Academy of Medicine's Chapter of Infectious Disease Physicians, said: "Yes, it's indeed very promising being the first agent to show an effect on reducing mortality."
He added that it is also very cost effective "but we are waiting for more details of the study and will be making recommendations locally".
Prof Leo Yee Sin, executive director of the National Centre for Infectious Diseases (NCID), said the drug is low cost and easy to administer, but further discussion is needed on "how this finding will influence and modify current treatment approach".
She added: "Nonetheless, we eagerly await more detailed information and formal publications with special attention to adverse effects."
But Prof Dale Fisher, a senior infectious diseases expert at the National University Hospital (NUH) is more confident, as he said Prof Horby "leads a strong team".
He said: "We have been afraid to use it because of the risk of secondary infections but I think this will give intensivists (specialist doctors working in intensive care) a lot of confidence to use it in the critically ill or even those needing supplemental oxygen."
Furthermore, Prof Fisher said the dose needed is just 6mg, "so it is working by immune suppression but the dose is not massive".
The drug is on the World Health Organisation's (WHO) list of essential medicines and is used for a host of conditions, including skin diseases, severe allergies, asthma, brain swelling and eye pain following eye surgery.
It is a generic drug that has been around since the 1960s, and would cost about 20 cents a day if taken orally.
The WHO said it is looking forward to the full data analysis in the coming days, as the researchers have shared only initial insights about the results of the trial.
Its director-general, Dr Tedros Adhanom Ghebreyesus, said: "This is the first treatment to be shown to reduce mortality in patients with Covid-19 requiring oxygen or ventilator support."