SINGAPORE - Singapore scientists say they are working with international partners to develop a trial for a vaccine for the coronavirus, with plans to begin testing it in as soon as four months.
At the same time, promising anti-viral drugs such as those used to treat HIV are being used on patients here, in efforts to locate a "magic drug" against the virus.
The Health Ministry's (MOH) chief health scientist, Professor Tan Chorh Chuan, said that Duke-NUS Medical School is working with the Coalition for Epidemic Preparedness Innovations (CEPI) to roll out a vaccine trial here.
This Straits Times understands this could happen as soon as in four months.
Time is needed to develop the vaccine and to test its safety and suitability for use on patients, he said during a press conference on Monday (Feb 10).
The meeting saw nine of Singapore's infectious disease experts gathering to detail what is being done to fight the virus, on both the science and health fronts.
The trial will involve giving the vaccine to healthy volunteers, who will be monitored for side effects.
They will also be observed to see the effects the vaccine has on their immune system.
A vaccine essentially works by stimulating a person's immune system so that it mounts a protective response against the virus.

CEPI, headquartered in Norway, is a public-private alliance that aims to derail epidemics by speeding up the development of vaccines.
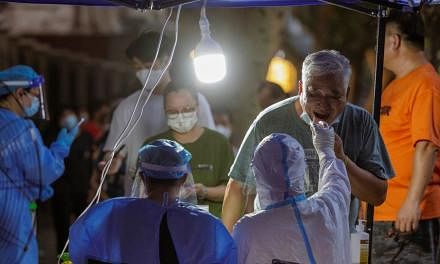
The novel coronavirus is spreading more widely in Singapore, with about half of the 43 people infected here now being locally transmitted cases.
Six of the patients are in critical condition.
Globally, scientists are racing to develop a vaccine against the virus, which has killed over 900 people and infected more than 40,000, with cases reported in two dozen other countries.
Coming up with any vaccine typically takes years, and involves a lengthy process of testing on animals, clinical trials on humans and regulatory approvals.
But, said the director of Duke-NUS' Programme in Emerging Infectious Diseases, Professor Wang Linfa, CEPI already has several processes prepared, including methods of production, that can be quickly used when a new virus emerges.
"So when the virus comes, it's just plug-and-play," he said.
Treatment
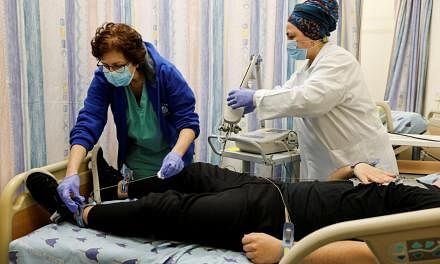
Research is also under way to develop anti-viral drugs, which can benefit the patients in the nearer term.
Prof Tan said that the National Centre for Infectious Diseases (NCID) is working with various parties to repurpose currently available drugs for patients who are severely ill.
Associate Professor David Lye, director of NCID's Infectious Disease Research and Training Office, who was also at the press conference, explained: "Repurposed drugs are drugs which have been shown to work in the lab on animal models. They have a safety profile which allows them to be tested on humans."
However, he noted that there is a need for further trials to test the efficacy of such drugs.
"We cannot do what we did during Sars - just using trial and error," he said.
China has been testing how effective such drugs are in combating the coronavirus, and Thailand's health ministry had previously said Thai doctors who gave the drugs to coronavirus patients have reported promising initial results.
So NCID has been in discussion with global experts, including those from the World Health Organisation (WHO), to develop a randomised controlled trial protocol.
"We hope to bring to our Singapore patients a proper randomised trial very, very soon," he said.
Having a trial here would mean that patients would benefit from the latest discoveries and treatments.
Currently, some patients here are being treated with anti-HIV drugs, namely lopinavir and ritonavir, to fight the disease.
However, Assoc Prof Lye noted: "The anti-HIV drug is not designed to (specifically) treat this virus, so we have to tell the patients about the side effects, and they have to agree to use it... The data is currently depending on models in an unrandomised study during Sars, so whether this is a 'magic drug' for the coronavirus remains to be seen."
Who will be worst hit?
Speaking at the same conference, NCID's executive director, Professor Leo Yee Sin, said that 19 patients with the virus have been recruited into a study to better understand the virus and identify who would be most at risk.
To do so, biological samples from the patients, including blood, urine and stool, are collected for analysis.
They will be compared against the clinical progression of the patients as their conditions develop, with the hope of seeing how their immune systems change with the progression of the infection.
This may pave the way for researchers to determine key periods for treatment and intervention.
"We're now able to run research and analyse some of the key characteristics we're looking at," said Prof Leo.
Known as Protect, the prospective study is the result of a protocol which was developed in 2012.
It aims to detect new pathogens and characterise their clinical features, as well as determine their transmission risk, and how they interact with their hosts, among other things.
The study also hopes to find out what populations are more at risk of the disease.
Prof Tan said: "To fight a war, you must know your enemy. This is a new virus, we need to know what we're dealing with."