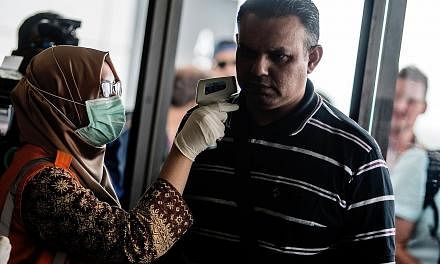
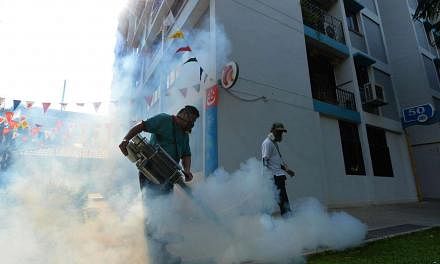It did not come as a surprise, given the millions of visitors passing through Singapore yearly, but when Zika reared its head among residents, it did give a jolt as the number of cases identified was high. Comparisons with incidences elsewhere cannot be accurately made as the disease is significantly underreported and underdiagnosed. Four in five people who are infected have no symptoms at all, while the remaining ones who suffer from a fever, rash and joint pains tend to recover within a week.
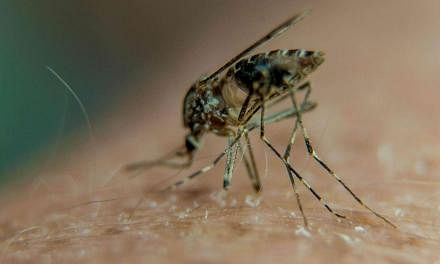
Another disease that is also spread by the Aedes mosquito, chikungunya, is generally self-limiting as well, lasting two to three days. However, mosquito-borne dengue occasionally develops into "a potentially lethal complication" and is a "leading cause of serious illness and death among children in some Asian and Latin American countries", as noted by the World Health Organisation. That scourge has been the focus of Singapore's well-oiled machinery to combat mosquitoes over decades. First World status does not grant immunity as climate and public habits can conspire to keep mosquitoes buzzing. Even bioengineering them to reduce numbers will come to naught if their breeding habitats remain intact, for example, stagnant water in plant pots, litter in public areas and blocked drains. As a progressive reduction in the mosquito population is never permanent, the battle against them never ends.
What has caused some alarm about Zika is the link between the virus and microcephaly (the impaired brain development of babies) as well as Guillain-Barre syndrome (an autoimmune disease that leads to weakness and paralysis). The risk for microcephaly with Zika infections in the first trimester of pregnancy ranges from 1 per cent to 13 per cent, according to a study. Babies being precious, no risk is too small for all efforts to be taken to eradicate the chain of infection here.
As Zika's symptoms are similar to those of dengue and chikungunya, all credit should be given to the neighbourhood doctors at Sims Drive Medical Clinic who were alert enough to notice that something was amiss among patients seen by different staff at the clinic.
Looking out for trends and factors that could impact public health should be viewed as the personal responsibility of not just healthcare professionals but also ordinary citizens. The tasks of disease monitoring, laboratory verification and epidemiologic investigation might be well institutionalised but public involvement remains crucial. Alongside new threats, even old ones might resurface. Tuberculosis, for example, was brought under control from the mid-20th century. Consequently, programmes were phased out in many countries, which left people unprepared for the rise of the curable disease in recent decades. All should stand sentinel against pathogenic invaders.