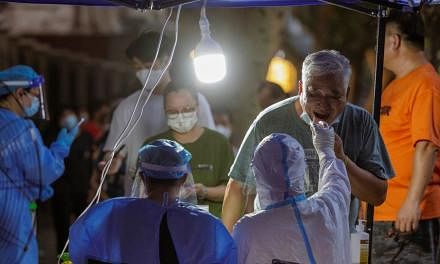
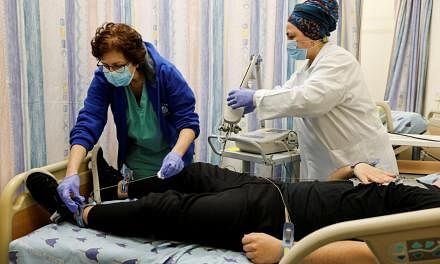
(FINANCIAL TIMES) - A surge in Covid-19 hospital admissions driven by the BA.5 sub-variant of Omicron, accompanied by the inability of vaccines to prevent reinfection, has prompted health policymakers to rethink their approach to boosters.
United States regulators last week recommended changing the design of vaccines to produce a new booster targeting Omicron - the first change to the make-up of shots since their introduction in late 2020.
Research into immune imprinting, whereby exposure to the virus via either infection or vaccination determines an individual's level of protection, is now driving the debate over the make-up of Covid-19 vaccines.
Immunologists say that, more than two years into the coronavirus pandemic, people have acquired very different types of immunity to the Sars-CoV-2 virus, depending on which strain or combination of strains they have been exposed to - leading to big differences in Covid-19 outcomes between individuals and countries.
"The effect is more nuanced than 'more times you have it, less protection you get'," said Professor Danny Altmann of Imperial College London, who is investigating the phenomenon with colleagues. "It's more helpful to consider it as progressive fine-tuning of a huge repertoire. Sometimes this will be beneficial for the next wave, sometimes not."
What is immune imprinting?
After someone encounters a virus for the first time, through infection or vaccination, the immune system remembers its initial response in a way that usually weakens the response to future variants of the same pathogen but may sometimes strengthen it. Proteins on the "spike", which the virus uses to bind with human cells, play a key role.
"Our first encounter with the spike antigen, either through infection or vaccination, shapes our subsequent pattern of immunity through immune imprinting," said Professor Rosemary Boyton of Imperial College.
The pattern has been observed for many years in flu and dengue virus, when it was usually called original antigenic sin. Studies are now demonstrating that it applies to Sars-CoV-2 too, although the effects are hard to pin down, according to Prof Altmann, who prefers the term "immune imprinting" to the biblical connotations of original sin.
A study of 700 United Kingdom healthcare workers by the Imperial team, published last month in the journal Science, found that Omicron infection had little or no beneficial effect of boosting any part of the immune system - antibodies, B-cells or T-cells - among people who had been imprinted with earlier Sars-CoV-2 variants.
"Omicron is far from a benign natural booster of vaccine immunity, as we might have thought, but it is an especially stealthy immune evader," said Prof Altmann.
Vaccines currently in use were designed to target the virus as it first emerged from Wuhan, China, more than two years ago. They retain high protection against severe disease and hospital admissions but their efficacy against transmission and mild infection wanes quickly, especially against Omicron.
Understanding the effect of immune imprinting will help health officials to decide which vaccines to use in future booster campaigns. Prof Boyton said immune imprinting has "important implications for future-proofing vaccine design and dosing strategies".
Does immune imprinting help to explain breakthrough infections?
Most people in the industrialised world have been infected with or vaccinated against Covid-19 - or both. England's Schools Infection Survey, run by the London School of Hygiene and Tropical Medicine, last week released data showing that 99 per cent of secondary schoolchildren tested positive for Covid-19 antibodies from natural infection.
By this stage of the pandemic, the vast majority of Covid-19 cases are reinfections in people whose immune defences acquired from vaccines or earlier infections do not hold up against Omicron BA.4 and BA.5.

Nor are these "breakthrough" infections necessarily as mild as many people believe, said Dr Ziyad Al-Aly, a clinical epidemiologist at Washington University in St Louis.
He analysed the health records of 34,000 people with breakthrough Covid-19 infections in the database of the US veterans administration, which provides healthcare services for retired soldiers. The cumulative risk of serious damage to heart, brain and lungs rose significantly with each repeated infection.
In another study, Dr Al-Aly and colleagues found that, while vaccines are good at preventing acute Covid-19, they were just 15 per cent effective at preventing long Covid, which is defined as suffering symptoms for 12 weeks or more after a Covid-19 diagnosis.
"Getting Covid, even among vaccinated people, seems almost unavoidable nowadays," he said.
Has immune imprinting influenced vaccine debates?
Some anti-vaxxers have enlisted immune imprinting in their arguments, on the grounds that vaccines become less effective as the virus evolves - an objection that immunologists reject forcefully.
"While our latest findings highlight clear concerns about the nature of Omicron infection, vaccination remains effective against severe disease," said Prof Altmann. "Those who are eligible to receive a booster should be encouraged to do so."
Professor Christian Drosten, a leading German virologist, said in an interview with Der Spiegel that extending the interval between jabs could help reduce the impact of immune imprinting.
"I suspect the effect (of vaccination) will get better, the greater the interval from the previous vaccination," he said. "But it is not yet known how long the interval between vaccinations should actually be."
How has differing immunity affected decisions on vaccines?
The World Health Organisation last month said Omicron-based jabs may be beneficial as boosters because they would broaden protection against different variants.
And, last Tuesday, the US Food and Drug Administration (FDA) advisory committee voted 19 to two in favour of incorporating genetic material from Omicron into new booster jabs.
"We're trying to use every last ounce of what we can from predictive modelling, and from the data that is emerging, to try to get ahead of a virus that has been very crafty," said Dr Peter Marks, director of the FDA's Centre for Biologics Evaluation and Research.
Last Thursday, the FDA recommended including a component of the BA.4/BA.5 Omicron sub-variants in a new shot for autumn booster campaigns. But the agency has not advised a change to the existing vaccine for first doses.
Moderna and BioNTech/Pfizer, the leading manufacturers of mRNA vaccines, have submitted laboratory data showing that their latest versions, targeted at Omicron, produce a potent antibody response against BA.4 and BA.5. But some immunologists remain uncertain whether they will be more effective than receiving another dose of the original Wuhan vaccine.
"Due to immune imprinting, patterns of anti-spike immunity in different people and populations have become heterogeneous, complex and unpredictable," said Prof Boyton. "This makes the argument for moving forward in a careful, considered and evidence-based way.
"The challenge for next-generation Covid vaccines is to design vaccines that broaden the immune response to protect against future variants of concern."