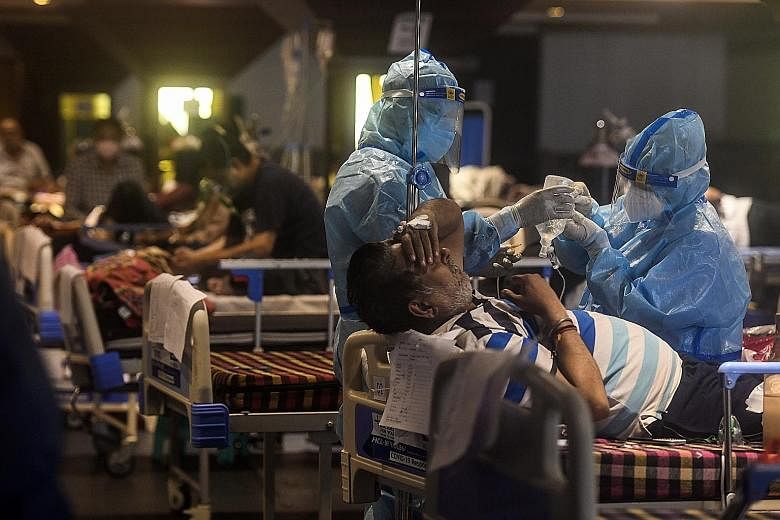
BANGALORE • Nearly two-thirds of people tested in India have shown exposure to Covid-19, a chain of private laboratories has said, indicating a runaway spread of the virus as the daily death toll rose to a record 4,529.
India reported 267,334 new daily infections yesterday, taking its tally to 25.5 million - the world's second highest after the United States - with a death toll of 283,248, Health Ministry data showed.
For months, no other nation has been hit harder than India by the pandemic, as a new variant discovered there fuelled a surge of up to more than 400,000 new infections a day. Only the US has had a worse single-day death toll, when it lost 5,444 people on Feb 12, a Reuters tracker shows.
With hospitals and crematoriums overflowing and the health system overwhelmed, it is widely accepted that the official figures grossly underestimate the real impact of the pandemic, with some experts saying infections and deaths could be five to 10 times higher.
There are fears that the new, highly infectious variant is out of control and that many cases are going unreported because of a lack of testing, particularly in the vast countryside.
Data from Thyrocare, a chain of private laboratories, appeared to back up those fears, showing that 63.5 per cent of people tested positive for Covid-19 antibodies on average over the last seven days, up from 45 per cent a month ago.
The data from 25 states included individuals who were previously infected, vaccinated, uninfected and those who had not been vaccinated, chief executive Arokiaswamy Velumani said on Twitter.
Criticism of Prime Minister Narendra Modi has been rising, but Mr M. Govinda Rao, a former member of the Economic Advisory Council to the Prime Minister, said the rate at which the virus was spreading had caught everyone by surprise.
"The unprecedented speed at which the second wave of the pandemic spread completely took the (state) governments as well as the people off guard," Mr Rao told The Hindu newspaper.
Daily testing hit a record two million on Tuesday, figures from the state-run Indian Council of Medical Research showed.
But that still falls short of India's claimed daily testing capacity of 3.3 million, said Professor Rijo M. John of Rajagiri College of Social Sciences in the southern city of Kochi.
He also questioned how useful the results of the tests were.
"Many of these tests are being deployed in urban centres, where cases may have peaked and so they don't serve much purpose," Prof John said.
"It's time they were diverted to more rural areas, but I doubt that is being done."
Mr Modi's approval ratings have fallen to a new low, two surveys showed.
A polling agency found that for the first time in seven years Mr Modi has been in office, there were more people expressing dissatisfaction with his government's performance than satisfaction.
India is the world's largest vaccine maker, but criticism has also mounted over its slow vaccination campaign, plagued by a lack of supplies.
The government said about 98 per cent of the population of 1.3 billion remain susceptible to infection.
India halted vaccine exports a month ago after donating or selling more than 66 million doses, and government sources told Reuters it was unlikely to resume major exports of vaccines until at least October as it prioritises domestic needs.
At midnight on Monday, Mumbai's municipal commissioner Iqbal Singh Chahal learnt that six hospitals in his city would run out of oxygen within hours, putting the lives of 168 patients at risk.
That night - which he described as the scariest he had - offered a look at tactics India's financial capital used to quell its outbreak faster, and with fewer casualties, than other parts of the country.
Amid the ensuing scramble, the patients were rushed to the temporary hospitals Mr Chahal's team had set up during the city's first wave last year. He kept the facilities even when cases dipped.
Unlike most Indian hospitals that relied on cylinders, they had been equipped with pipes that supplied oxygen directly to patients' beds. All 168 survived.
That localised approach helped as affluent neighbourhoods were worse hit during the second wave.
The local war rooms got test reports and reduced the spread of infection by pointing patients to the nearest available hospital beds.
The city administration negotiated with private hospitals to allocate beds for Covid-19 patients at government-decided rates.
"We set up an excellent public-private partnership between hospitals which is still today not visible in the rest of the country," Mr Chahal said.
Even India's Supreme Court has suggested that aspects of Mumbai's model could be adopted in other parts of the nation like New Delhi.
Still, the risks to Mumbai are far from over.
The city has recorded 688,696 cases since the pandemic began, adding 1,544 on Sunday.
REUTERS, BLOOMBERG